01 March 2021: Clinical Research
Types of Parenchymal Changes Diagnosed on DMSA Scans of Kidneys Affected by Different Grades of Vesicoureteral Reflux
Adela Arapović1ABCDEF, Ante Punda2ABDF, Dubravka Brdar3BCDF, Vesna Čapkun3BCDF, Diana Bajo4BCEF, Daniela Veljačić1BCEF, Hrvoje Punda5BDEF, Ana Simičić-Majce1BDEF, Mirna Saraga-Babić6CDEF, Katarina Vukojević6CDEF, Marijan Saraga12ABCDEF*DOI: 10.12659/MSM.929617
Med Sci Monit 2021; 27:e929617
Abstract
BACKGROUND: Renal parenchymal damage and scarring usually is associated with urinary tract infection (UTI), whereas the impact of vesicoureteral reflux (VUR) on the kidneys is unclear. We aimed to compare kidneys with all grades of VUR (grades Io–V) and those without VUR by using direct radionuclide cystography, voiding cystourethrography, and findings from 99mTc-DMSA scintigraphy (DMSA scan).
MATERIAL AND METHODS: The present analysis included 253 renal ureteral units (RUU) from 129 children with VUR and recurrent UTI and children with a single febrile UTI associated with abnormal ultrasonographic findings. The 6 grades of VUR (Io, I, II, III, IV, and V) and 35 RUUs without VUR were divided into 4 groups: 1. Non-dilated VUR (grades Io–II); 2. Mildly dilated VUR (grade III); 3. Dilated VUR (grades IV–V); and 4. The control group.
RESULTS: DMSA scanning showed significant differences between the groups with non-dilated VUR, grade III VUR, grades IV–V VUR, and the control group in kidney width (χ²=30.5; P<0.001); position and shape (χ²=30.6; P<0.001); intensity of activity (χ²=38.1; P<0.001); distribution of activity (χ²=34.5; P<0.001); and existence of scars (χ²=16; P<0.001). The probability of abnormalities on DMSA scans increased with the VUR grade. However, inside the groups of dilated and non-dilated VUR we found no significant statistical differences between those characteristics.
CONCLUSIONS: Our results indicate that kidneys without VUR or with non-dilated lateral VUR and dilated VUR on the contralateral side represent 2 different categories of parenchymal changes.
Keywords: Radionuclide Imaging, Urinary Tract Infections, Vesico-Ureteral Reflux, Child, Child, Preschool, Cicatrix, Infant, Infant, Newborn, Kidney, Parenchymal Tissue, Radiopharmaceuticals, Technetium Tc 99m Dimercaptosuccinic Acid, Ureter, Urination
Background
Vesicoureteral reflux (VUR) is defined as backflow of urine from the urinary bladder to the proximal part of the urinary tract, including the kidney parenchyma. VUR occurs in 1% to 2% of the pediatric population [1], and about one-third of children with VUR will experience a urinary tract infection (UTI). Although UTI is mostly responsible for the renal parenchyma damage, hydrostatic pressure from urine backflow also can influence the severity of disease [2–7]. Therefore, it is important to evaluate whether urine backflow reaches the renal parenchyma, and if so, its volume [8–12]. Many studies have reported a correlation between parenchymal damage and the grade of VUR [13–16]. In many countries, the traditional method for detecting VUR is still voiding cystourethrography (VCUG), which is more descriptive but less sensitive than direct radionuclide cystography (DRNC), according to the majority of authors [17–23]. There are rare studies, however, which have reported the opposite results [24,25]. Compared to DRNC, VCUG results in a 50 to 200 times higher dose of radiation to the patient.
DRNC, in contrast, can distinguish between more grades of VUR than is possible with VCUG [17,19–23]. According to the International Reflux Study in Children (IRSC) grading classification, VUR is divided into 5 grades [26]. When DRNC is incorporated into patient evaluation, 9% to 18.5% more cases of VUR can be found than with VCUG [19,21]. DRNC can discriminate among 3 grades of VUR (small, medium, and large) [19,27]. To assess damage to the renal parenchyma caused by VUR and/or UTI, a 99mTc-dimercaptosuccinic (DMSA) scanning can be performed, which is still the criterion standard for imaging of functional kidney tissue [28–30].
Sometimes, interpretation of results from kidney tests can be complicated, especially when renal length is estimated and several different specialists in nuclear medicine are involved [28,31,32]. The formulas and nomograms for renal length are not always in accordance with results from ultrasonography. Renal length usually is longer on DMSA than when meaured on ultrasonography. Although ultrasonography is more accurate for measuring renal length, more readily available, and harmless, DMSA scanning is superior to ultrasonography for assessment of parenchymal damage and function [32]. In the present study, we aimed to correlate all grades of VUR with specific damage to the kidney parenchyma, as diagnosed on DMSA scan. We also wanted to compare kidneys with VUR and those without VUR using the same method. Our hypothesis was that in patients with recurrent UTI and VUR, parenchymal damage worsens as the grade of VUR increases. We also believe that in previous analyses of findings from DMSA scanning, some characteristics of the testing were not adequately evaluated.
Material and Methods
The present study enrolled 129 children with VUR and recurrent UTI or a single episode of febrile UTI who had abnormal findings on ultrasonography. Patients were included if they had a single pyelocaliceal system and single ureter, whereas those with a duplex collecting system were excluded. Of the patients enrolled, 49 (38%) were boys and 80 (62%) were girls. All of the patients underwent DRNC and VCUG. When both of the tests were positive, grading of VUR was based on the IRSC classification. When DRNC was positive and VCUG was negative, a patient was considered to have Io-grade VUR.
Renal ureteral units (RUUs) were analyzed based on 5 grades of VUR, according to the IRSC classification, plus a single grade detected solely by DRNC (Io, I, II, III, IV, and V); patients with no VUR served as the control group. Patients were divided into 4 groups: 1. Non-dilating VUR (grades Io-II); 2. Mildly dilated VUR (grade III); 3. Dilated VUR (grades IV–V); and 4. Controls (no VUR). DRNC was performed based on the 2014 recommendations from the American College of Radiology (ACR) [27]. Catheterization was done with the patient in the horizontal position with a double-lumen, sterile Foley catheter (8–14F). After the bladder was drained, it was filled with warm saline containing 99mTc pertechnetate (74 MBq/500 mL) under a hydrostatic pressure of 60 to 70 cmH2O until the bladder was full or the child expressed the urge to void. When the bladder capacity was reached, the catheter was removed and the patient was moved to a sitting position. In most cases, the patient started to void. For visualization of radiotracer, a computerized gamma camera (Siemens LFOV) equipped with a parallel, low-energy, all-purpose collimator was used. The data were stored in the computer (Digital PDP 11/34) dynamic mode: 1 frame/5 s. Dynamic analog images were produced, 1/60 s during the filling phase and 1/5 s during voiding [19].
VCUG was performed based on recommendations from the ACR (revised 2019; Resolution 10) [26]. Catheterization was done with a feeding tube (8F) and the bladder was filled with warmed saline mixed with contrast medium (Telebrix) in a 12% dilution under hydrostatic pressure of 60 to 70 cmH2O. The patient was in the horizontal position. When the bladder reached full capacity or the patient expressed an urge to void, the filling was stopped and the patient was placed in a seated or upright position. When the catheter was removed, in most cases, patients started to void. Two overhead abdominal films were made during both the filling and voiding phases. Fluoroscopy also was used to monitor the patients during the examination [19].
After VUR had been diagnosed, patients underwent a DMSA scan following guidelines from the European Association of Nuclear Medicine [28]. For this purpose, we used 99mTc DMSA injected intravenously in doses adjusted according to the body surface of each child. Images were acquired with a double-headed gamma camera with a low-energy, high-resolution collimator. A child was placed in a supine position and both posterior and anterior images were taken. It was possible to acquire both views simultaneously with the double-headed gamma camera. Images of both kidneys were acquired with a total of 300 000 to 500 000 counts with a matrix of 128×128.
Visual measurements were estimated by 3 independent specialists in nuclear medicine. Parenchymal thickness and presence of ectopic and malrotated kidneys were estimated visually and by calculating a differential renal function percentage. Regarding positioning, the kidneys usually are located between the Th12 and L3 vertebral segments. The intensity of uptake was estimated visually, but also based on total DMSA uptake in each kidney, which was calculated by determining the counts in each region of interest. The parameters for homogeneity were estimated visually, while the presence of scars was assessed visually and was characterized by lack of 99mTc DMSA uptake and loss of kidney contour. The size of kidneys was measured visually on the planar 99mTc-DMSA images.
The results were analyzed by 3 independent specialists in nuclear medicine. Observers were not aware of the results of previously performed VCUG, DRNC, or ultrasonography. The DMSA scans were analyzed for the following characteristics: 1. Parenchymal width; 2. Position, rotation and outline; 3. Intensity of radiotracer uptake; 4. Distribution of radiotracer uptake; 5. Presence of scars; and 6. Other renal impairments.
Finally, only findings that were confirmed by at least 2 specialists were taken into account. In the present study, we used the χ2 test and logistic regression because of adaptation of groups according to the age and time interval between diagnosis of VUR and DMSA scanning. Results with
Results
PARENCHYMA WIDTH:
The percentage of kidneys with thinned parenchyma in the non-dilated group of VURs was the same as in the control group.
Compared with that in the control group, there were 2.3 times more kidneys with parenchymal thinning in the group with grade III VUR and 3.5 times more in the group with grade IV–V VUR, as well as in the group with non-dilated VUR (χ2=30.5;
There were 4.9 times fewer kidneys with parenchymal thinning than with normal parenchymal width in the control group and in the group with non-dilated VUR and 1.6 times fewer in the group with grade III VUR, whereas parenchymal thinning was 1.5 times more common in the group with grade IV–V VUR.
POSITION, ROTATION, AND OUTLINE:
We found a statistically significant difference among the groups (χ2=30.6;
INTENSITY OF RADIOTRACER UPTAKE (NORMAL/DIMINISHED):
We found a statistically significant difference among the groups (χ2=38.1;
DISTRIBUTION OF RADIOTRACER UPTAKE (HOMOGENEOUS/NONHOMOGENEOUS):
We found a statistically significant difference among the groups (χ2=34.5;
In the control group, a single kidney had nonhomogeneous distribution of activity. Nonhomogeneous distribution of activity was 3.7 times less common in the group with non-dilated VUR, while the incidence of homogenous and nonhomogeneous activity was equal in patients with grade III VUR. In the patients with grade IV–V VUR, in contrast, nonhomogeneous distribution of radiotracer was 1.2 times more common. A logistic regression analysis with adjustment for age at diagnosis confirmed the difference in activity between the control group and the group with non-dilated VUR (OR 9.9%, CI 1.2–68,
SCARS (YES/NO):
The incidence of kidney scarring increased with the grade of VUR and the differences among groups were statistically significant (χ2=16;
In the group with non-dilated VUR, there were 17 times more kidneys without than with scars, whereas in the group with grade III VUR, there were 5.2 times more kidneys without scars. In the group with grade IV–V VUR, there were 3.3 times more kidneys without scars than with scars.
OTHER RENAL IMPAIRMENTS (SHRINKING, SMALL SIZE, ENLARGEMENT, AND THINNING):
Among other renal impairments in the studied group, 14.6% of kidneys overall were small. Incidence of small kidneys was 13.4% in the group with non-dilated VUR, 12.5% in the group with grade III VUR, and 34% in the group with IV–V VUR. In contrast, only a single kidney in the control group was small.
RENAL CHARACTERISTICS IN THE GROUP WITH GRADE IO-II VUR:
In the group with non-dilated VUR, the grade of VUR did not influence the parenchymal width of kidneys (χ2=1.77, P=0.412) or the intensity (χ2=1.33, P=0.513) or distribution of activity in them (χ2=1.17, P=0.556) (Table 4). In terms of kidney position and scarring in the group with non-dilated VUR, only 2.4% of the kidneys were irregularly positioned and 5.6% were scarred.
KIDNEY CHARACTERISTICS IN THE GROUP WITH GRADE IO-II VUR VS CONTROLS:
There were no statistically significant differences between kidneys in the control group and those in the group with non-dilated VUR in terms of parenchymal width (χ2=0;
KIDNEY CHARACTERISTICS IN THE GROUPS WITH GRADE III VS GRADE IV–V VUR:
There were no statistically significant differences between kidneys in the groups with grade III and grade IV–V VUR in terms of parenchymal width (χ2=2.9;
PROBABILITY OF CHANGES ON DMSA SCAN WITH INCREASED VUR GRADE:
Because the time interval between diagnosis of VUR and DMSA scanning was very long in some cases, we used logistic regression to assess the influence of VUR grade (no VUR, Io-II, III, and IV–V) on kidney impairment for each studied parameter, as measured with DMSA scan, with adjustment for age and the time interval between the diagnosis of VUR and the DMSA scan. Time intervals were divided into 4 categories, based on quartiles and medians.
We found that the probability of decreased parenchymal width more than doubled (95%CI 1.8–3.6) with each increase in VUR grade compared with normal parenchymal width and that the probability of abnormal kidney position was increased 4.8 times (95%CI 2.4–9.3). For each increase in VUR grade, the probability of decreased isotope activity and decreased distribution of activity was 2.8 times higher (95%CI 1.9–4) and the probability of scar formation was 3.1 times higher (95%CI 1.8–5.5) (Table 5).
Discussion
In 37% to 68% of cases, kidneys with UTI accompanied by VUR developed scars and abnormal DMSA findings, whereas the incidence was only 6% to 33% in kidneys with UTI unrelated to VUR. Scarring of the kidney itself is indicative of VUR [3,7,29,30]. All those findings suggest a strong relationship between VUR and parenchymal injury. Our study clearly showed a relationship between VUR and abnormalities on DMSA scanning, as well as a correlation between increases in abnormalities on DMSA scanning and progression of each grade of VUR.
For reasons that have yet to be clarified other than infection, VUR on its own, whether congenital or acquired, can be a significant risk factor for development of renal parenchymal injury [4,30,33]. Preexisting and acquired parenchymal scars have been reported more frequently in older children in association with multiple episodes of febrile UTI, and more often in children with grade IV VUR than in children with lower-grade VUR [14], thus indicating that parenchymal changes are silent and slowly accumulate over time [33]. The suggestion that VUR is not serious on its own, is only a significant risk factor for UTI, and does not contribute to scar formation and renal insufficiency [34] is not acceptable, given that the present study showed that the rate of abnormalities on DMSA scanning was significantly higher in kidneys with VUR than in kidneys with UTI but without VUR in our control group.
Snodgrass found a high percentage (50%) of abnormal DMSA scans in patients with high-grade VUR and no abnormalities on DMSA scans in patients with grade II VUR [13]. Our study, however, showed that both a high percentage of abnormalities on DMSA scans associated with higher-grade VUR and a significant percentage of such abnormalities also were associated with lower-grade VUR.
Moreover, some other studies [6,7], as well as ours, have shown abnormalities on DMSA scans in 6% to 33% of patients with UTI who do not have VUR, thus confirming the role of infection in the development of parenchymal changes.
Garin et al found insufficient evidence that non-dilated VUR increased the incidence of parenchymal scarring, whereas they reported insufficient data on which to base a conclusion about the group with high-grade VUR [35]. Because our study included a significant number of cases of non-dilated and dilated VUR, we were able to show that the number of abnormalities on DMSA scans rose significantly as the grade of VUR increased.
It is obvious that the incidence of parenchymal changes is higher in patients with VUR, with or without UTI. VUR can transmit bacteria or chemicals into the tubulointerstitial space, leading to a self-progressing process of fibrosis in that space. Only in a minority of cases does parenchymal damage develop without VUR, probably as a result of bacterial infection, whereas in the majority of cases, such damage develops in the presence of VUR, suggesting that VUR plays a crucial role in the development of renal scars.
In our study, the fact that the incidence of ectopic and rotated kidneys and of kidneys with altered outlines increased significantly with the grade of VUR gives credence to the theory that those characteristics are potential predictors of VUR. This is consistent with a 2010 study by Van den Bosch et al, which proved that incidence of VUR is increased and relative renal function decreased in patients with ectopic kidneys [36].
Regarding the timing of cystography and DMSA scanning, spacing between them of at least 6 months is recommended [4,7]. In our study, that elapsed period was 1.9 years, which was sufficient time to reveal definitive changes in renal parenchyma caused by VUR or UTI. In the present study, the abnormalities most frequently seen on DMSA scans were diminished uptake of radiotracer, decreased parenchymal width, and nonhomogeneous distribution of radiotracer uptake.
Significant differences were observed among groups with non-dilating VUR, mildly dilated VUR, dilated VUR, and kidneys without VUR in terms of parenchymal width, kidney shape, rotation and position, intensity and distribution of isotope activity, and existence of parenchymal scars.
In the group with non-dilating VUR, however, there were no statistically significant differences between grades of VUR in parenchymal width; kidney position, rotation, and outline; intensity of radiotracer activity; distribution of renal activity; or presence of scars. Moreover, there were no statistically significant differences between the kidneys in the group with non-dilated VUR and those in the control group in terms of parenchymal width, intensity of activity, or presence of scars. That means that patients with kidneys with non-dilating VUR and the controls probably represent a low-risk group in terms of prognosis and approach to therapy [14,34,37–40].
The present study showed no statistically significant differences among the groups with dilated VUR in terms of the aforementioned characteristics on DMSA scans.
Therefore, those patients also have a group of diseases that share the same prognoses and for which the approach to therapy should be similar [15].
Finally, on DMSA scans, we found approximately the same percentage of small kidneys in all cases with non-dilated VUR and a higher percentage (34%) of small kidneys in the group with dilated VURs, which is consistent with the findings of Guarino et al [16].
Conclusions
DMSA scans revealed statistically significant differences between the kidneys with non-dilated, mildly dilated, and dilated VURs and the kidneys with no VUR. The probability for progression of abnormalities on DMSA increased in proportion to the grade of VUR.
According to the results of the present study, patients with non-dilating VUR and without VUR are significantly different from those with mildly and highly dilated VUR. Non-dilating and dilating VUR clearly represent 2 totally different categories of disease that likely have different clinical courses and prognoses.
We have found that despite possible variability in the interpretation of DMSA scans by different observers – what could be considered as the bias in the present study – some DMSA scans probably have not been used properly in diagnosis of kidneys affected by VUR. In conclusion, the results of the present study prove that DMSA scanning is still a reliable and predictive tool for diagnosing VUR.
Tables
Table 1. Total number of cases of VUR of all grades in the study group and number of analyzed RUUs in the control group by side.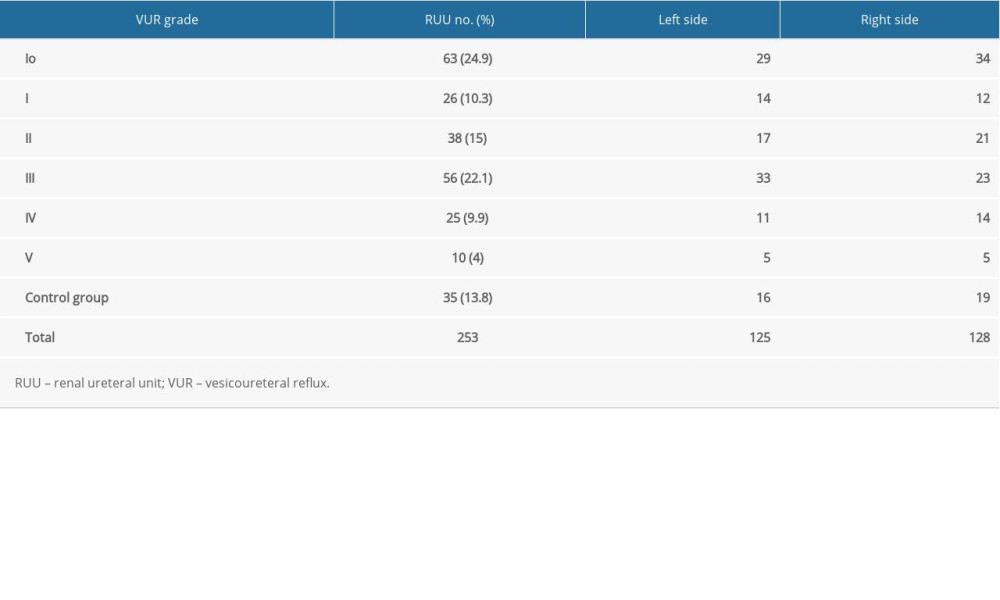 Table 2. Comparison of mean ages (median, min–max) at VUR diagnosis and DMSA scan and VUR grade versus time elapsed (median, min–max) from VUR diagnosis to DMSA scan.
Table 2. Comparison of mean ages (median, min–max) at VUR diagnosis and DMSA scan and VUR grade versus time elapsed (median, min–max) from VUR diagnosis to DMSA scan.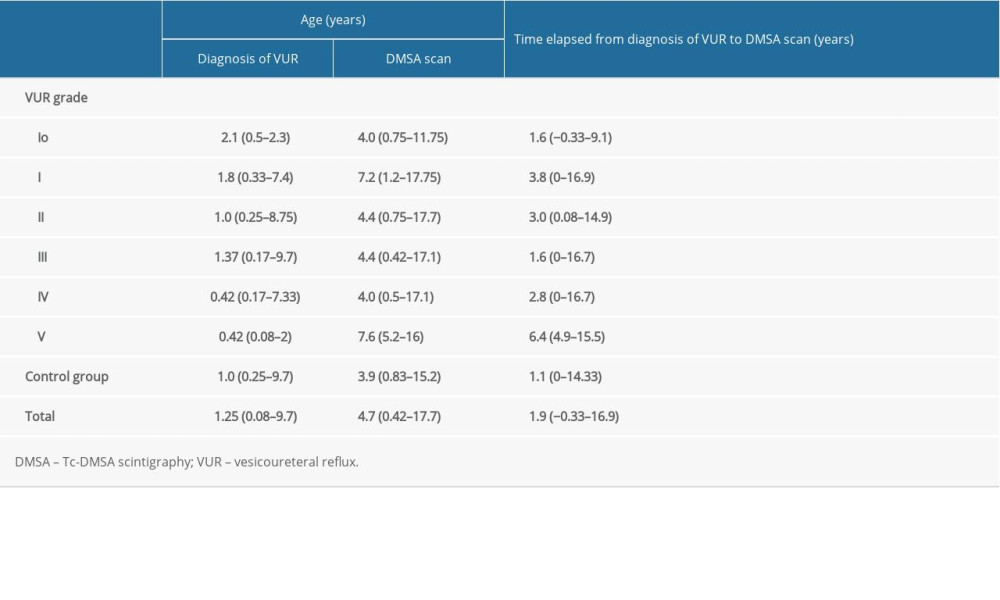 Table 3. Comparison of abnormalities on DMSA scan (number and percentage of kidneys) in groups with non-dilated and dilated VUR and no VUR.
Table 3. Comparison of abnormalities on DMSA scan (number and percentage of kidneys) in groups with non-dilated and dilated VUR and no VUR.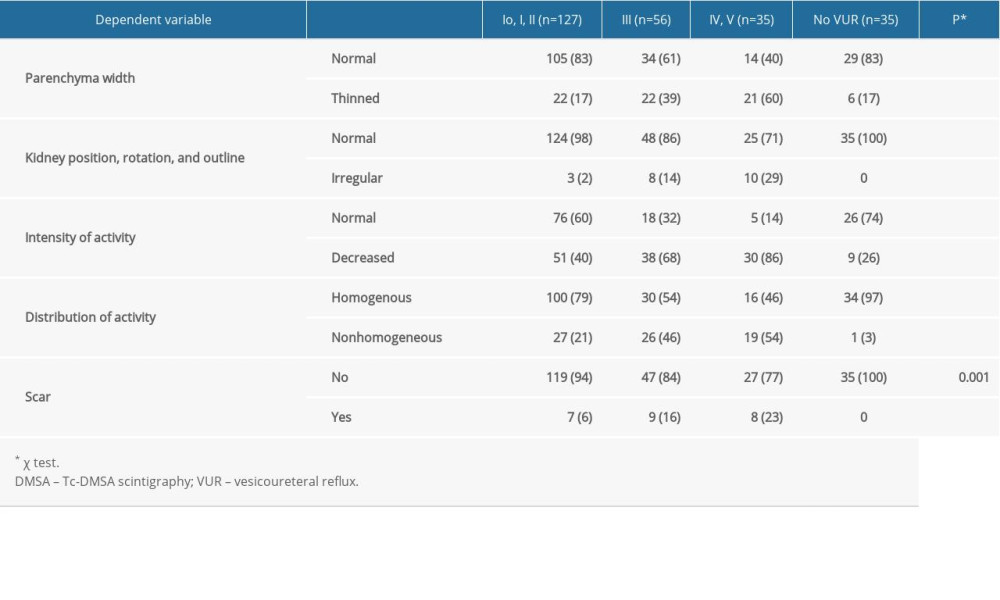 Table 4. Number and percentage of kidneys in the group with non-dilated VUR (Io-II) that had abnormalities on DMSA scans and their relationships to VUR grade.
Table 4. Number and percentage of kidneys in the group with non-dilated VUR (Io-II) that had abnormalities on DMSA scans and their relationships to VUR grade.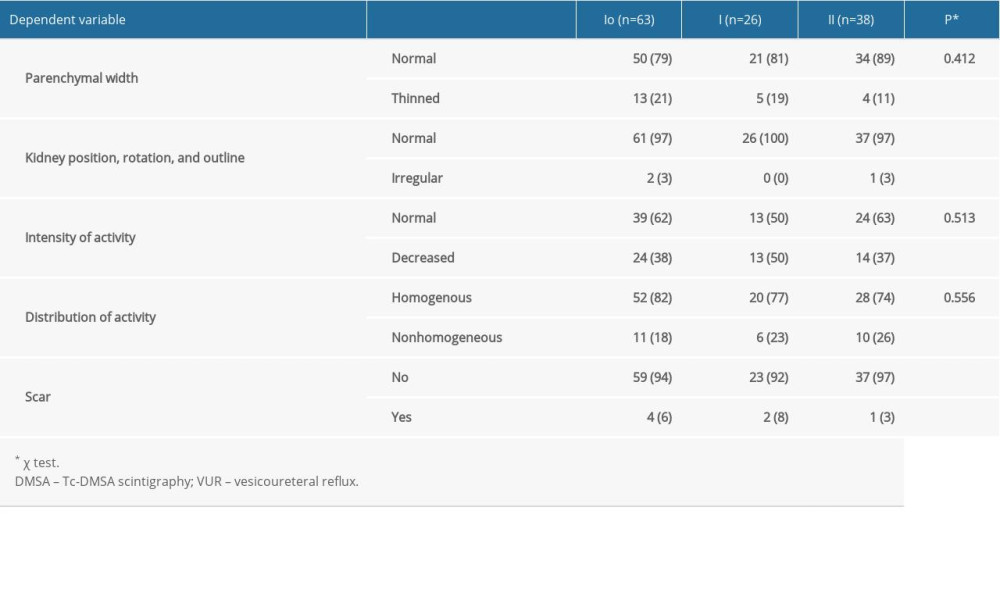 Table 5. Logistic regression analysis of the influence of VUR grade on kidney impairment as shown on DMSA scan, adjusted for age and time interval between VUR diagnosis and DMSA scan.
Table 5. Logistic regression analysis of the influence of VUR grade on kidney impairment as shown on DMSA scan, adjusted for age and time interval between VUR diagnosis and DMSA scan.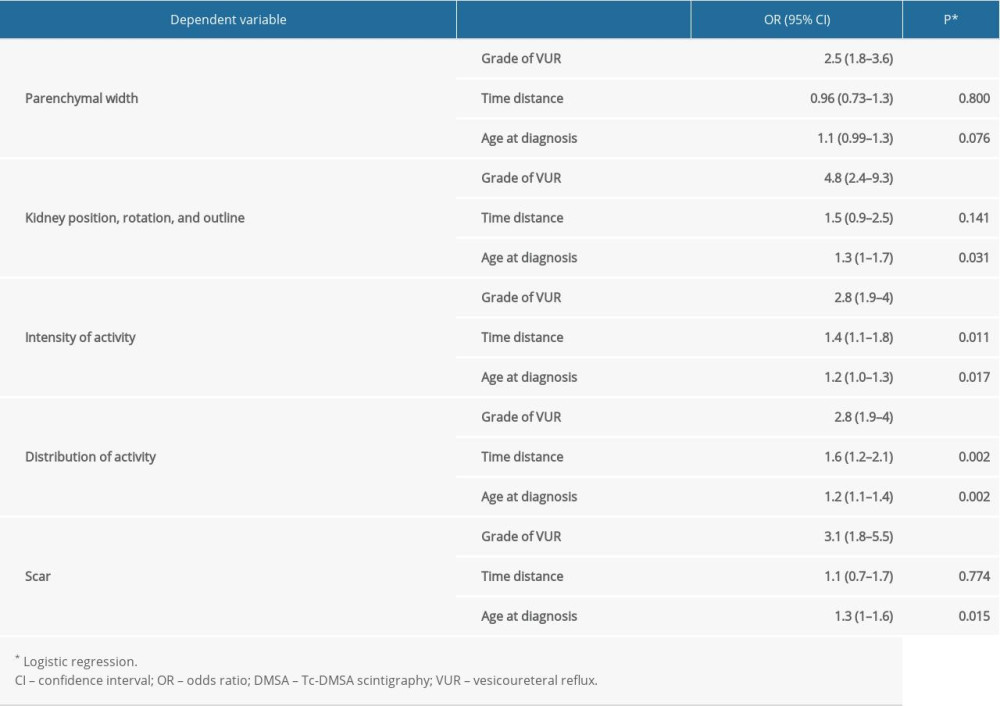
References
1. Bailey RR: Reflux nephropathy, 1979; 59-61, New York, Masson
2. Hodson CJ, Edwards D, Chronic pyelonephritis and vesico-ureteric reflux: Clin Radiol, 1960; 11; 219-31
3. Gleeson FV, Gordon I, Imaging in urinary tract infection: Arch Dis Child, 1991; 66; 1282-83
4. Jakobsson B, Nolstedt L, Svensson L, 99mTechnetium dimercaptosuccinic acid scan in the diagnosis of acute pyelonephritis in children: Relation to clinical and radiological findings: Pediatr Nephrol, 1992; 6; 328-34
5. Wennerstrom M, Hansson S, Jodal U, Primary and acquired renal scarring in boys and girls with urinary tract infection: J Pediatr, 2000; 136; 30-34
6. Roger M, Wilkinson AG, Cystoscopic and DMSA findings in relation to types of reflux demonstrated on percutaneous direct radionuclide cystography in children: Pediatr Radiol, 2004; 34; 222-26
7. Polito C, Rambaldi PF, Signoriello G, Permanent renal parenchymal defects after febrile UTI are closely associated with vesicoureteric reflux: Pediatr Nephrol, 2006; 21(4); 521-26
8. Kim SW, Im YJ, Hong CH, The clinical significance of intrarenal reflux in voiding cystourethrography (VCUG): Korean J Urol, 2010; 51(1); 60-63
9. Boubnova J, Sergent-Alaoui A, Deschenes G, Evolution and prognosis value of intrarenal reflux: J Pediatr Urol, 2011; 7; 638-43
10. Rolleston GL, Maling TMJ, Hodson CJ, Intrarenal reflux and scarred kidney: Arch Dis Child, 1974; 49; 531-37
11. Fukui S, Watanbe M, Yoshino K, Intrarenal reflux in primary vesicoureteric reflux: Int J Urol, 2013; 20; 631-36
12. Schneider KO, Lindemeyer K, Kammer B, Intrarenal reflux, an overlooked entity-retrospective analysis of 1166 voiding cysturethrographies in children: Ped Radiol, 2019; 49; 617-25
13. Snodgrass WT, Shah A, Yang M, Prevalence and risk factors for renal scars in children with febrile UTI and/or VUR. A cross-sectional observational study of 565 consecutive patients: J Pediatr Urol, 2013; 9; 856-63
14. Mattoo TK, Chesney RW, Greenfield SPfor the RIVUR Trial Investigators, Renal scarring in the randomized intervention for children with vesicoureteral reflux (RIVUR) trial: Clin J Am Soc Nephrol, 2016; 7; 54-61
15. Brandstrom P, Neveus T, Sixt R, The Swedish reflux trial in children: IV. Renal damage: J Urol, 2010; 184; 292-97
16. Guarino S, Capalbo D, Martin N, In children with urinary tract infection reduced kidney length and vesicoureteric reflux predict abnormal DMSA scan: Pediatr Res, 2019; 87(4); 779-84
17. Grunberg J, Bonelli S, Velasco M, Recurrent febrile urinary tract infections with normal voiding cystography. Absent or elusive vesico-ureteric reflux?: (Letter) Pediatr Nephrol, 1991; 5; 761-63
18. Dikshit MP, Acharya VN, Shikare S, Comparison of direct radionuclide cystography with micturating cystourethrography for the diagnosis of vesicoureteric reflux, and its correlation with cystoscopic appearances of the ureteric oriffices: Nephrol Dial Transplant, 1993; 8; 600-2
19. Saraga M, Staničić A, Marković V, The role of direct radionuclide cystography in evaluation of vesicoureteral reflux: Scand J Urol Nephrol, 1996; 30; 367-71
20. Poli-Merol ML, Francois S, Pfliger F, Interest of direct radionuclide cystography in repeated urinary tract infection exploration in childhood: Eur J Pediatr Surg, 1998; 8(6); 339-42
21. Polito C, Rambaldi PF, La Manna A, Enhanced detection of vesicoureteric raflux with isotopic cystography: Pediatr Nephrol, 2000; 14; 827-30
22. Mclaren CJ, Simpson ET, Direct comparison of radiology and nuclear medicine cystograms in young infants with vesico-ureteric reflux: BMJ, 2001; 87; 93-97
23. Dalirani R, Mahyar A, Sharifian M, The value of direct radionuclide cystography in the detection of vesicoureteral reflux in children with normal voiding cystourethrography: Pediatr Nephrol, 2014; 29; 2341-45
24. Blaufox MD, Gruskin A, Sandler P, Radionuclide scintigraphy for detection of vesicoureteral reflux in children: J Pediatr, 1971; 79(2); 239-46
25. Unver T, Alpay H, Biyikli NK, Ones T, Comparison of direct radionuclide cystography and voiding cystourethrography in detecting vesicoureteral reflux: Pediatr Int, 2006; 48; 287-91
26. American College of Radiology: ACR-SPR practice parameter for the performance of fluoroscopic and sonographic voiding cystourethrography in children . Revised 2019 (Resolution 10)https://www.arc.org/Clinical-Resources/Practice-Parameters-and-Technical-Standards
27. American College of Radiology: ACR-SNM-SPR practice parameter for the performance of radionuclide cystography, 2014, Amended (Resolution 39)
28. Piepsz A, Colarinha P, Gordon IPaediatric Committee of the European Association of Nuclear Medicine, Guidelines on 99mTc-DMSA scintigraphy in children. Revised guidelines on 99mTc-DMSA scintigraphy in children (2009): Original version published in: Eur J Nucl Med, 2001; 28(3); 37-41
29. Camacho V, Estorch M, Fraga G, DMSA study performed during febrile urinary tract infection: A predictor of patient outcome?: Eur J Nucl Med Mol Imaging, 2004; 173(4); 1364
30. Mattoo TK, Skoog SJ, Gravens-Mueller Lfor the RIVUR Trial Investigators, Interobserver variability for interpretation of DMSA scans in the RIVUR trial: J Pediatr Urol, 2017; 13(6); 616.e1-e6
31. Buonomo C, Treves ST, Jones B, Silent renal damage in dymptom-free siblings of children with vesicoureteral reflux: Assessment with technetium Tc 99m dimercaptosuccinic acid scintigraphy: J Pediatr, 1993; 122(5); 721-23
32. Lee MJ, Son MK, Kwak BO, Kidney size estimation in Korean children with Tehnetium-99m dimercaptosuccinic acid scintigraphy: Korean J Pediatr, 2014; 57(1); 41-45
33. Kosmeri C, Kalaitzidis R, Simou E, An update on renal scarring after urinary tract infection in children: What are the risk factors?: J Pediatr Urol, 2019; 15; 598-603
34. Johnston DL, Quereshi AH, Irvine RW, Contemporary management of vesicoureteral reflux: Curr Treat Options Pediatr, 2016; 2(2); 82-93
35. Garin EH, Primary vesicoureteral reflux;What have we learnt from the recently published randomized, controlled trials?: Pediatr Nephrol, 2019; 34; 1513-19
36. van den Bosch CM, van Wijk JA, Beckers GM, Urological and nephrological findings of renal ectopia: J Urol, 2010; 183(4); 1574-78
37. Hoberman A, Charron M, Hickey RW, Imaging studies after a first febrile urinary tract infection in young children: N Engl J Med, 2003; 348; 195-202
38. Wadie GM, Moriarty KP, The impact of vesicoureteral reflux treatment on the incidence of urinary tract infection: Pediatr Nephrol, 2012; 27; 529-38
39. Tullus K, Vesicoureteric reflux in children: Lancet, 2015; 385; 371-79
40. Brandstrom P, Hansson S, Long-term, low-dose prophylaxis against urinary tract infections in young children: Pediatr Nephrol, 2015; 30; 425-32
Tables
 Table 1. Total number of cases of VUR of all grades in the study group and number of analyzed RUUs in the control group by side.
Table 1. Total number of cases of VUR of all grades in the study group and number of analyzed RUUs in the control group by side. Table 2. Comparison of mean ages (median, min–max) at VUR diagnosis and DMSA scan and VUR grade versus time elapsed (median, min–max) from VUR diagnosis to DMSA scan.
Table 2. Comparison of mean ages (median, min–max) at VUR diagnosis and DMSA scan and VUR grade versus time elapsed (median, min–max) from VUR diagnosis to DMSA scan. Table 3. Comparison of abnormalities on DMSA scan (number and percentage of kidneys) in groups with non-dilated and dilated VUR and no VUR.
Table 3. Comparison of abnormalities on DMSA scan (number and percentage of kidneys) in groups with non-dilated and dilated VUR and no VUR. Table 4. Number and percentage of kidneys in the group with non-dilated VUR (Io-II) that had abnormalities on DMSA scans and their relationships to VUR grade.
Table 4. Number and percentage of kidneys in the group with non-dilated VUR (Io-II) that had abnormalities on DMSA scans and their relationships to VUR grade. Table 5. Logistic regression analysis of the influence of VUR grade on kidney impairment as shown on DMSA scan, adjusted for age and time interval between VUR diagnosis and DMSA scan.
Table 5. Logistic regression analysis of the influence of VUR grade on kidney impairment as shown on DMSA scan, adjusted for age and time interval between VUR diagnosis and DMSA scan. In Press
08 Mar 2024 : Clinical Research
Evaluation of Foot Structure in Preschool Children Based on Body MassMed Sci Monit In Press; DOI: 10.12659/MSM.943765
15 Apr 2024 : Laboratory Research
The Role of Copper-Induced M2 Macrophage Polarization in Protecting Cartilage Matrix in OsteoarthritisMed Sci Monit In Press; DOI: 10.12659/MSM.943738
07 Mar 2024 : Clinical Research
Knowledge of and Attitudes Toward Clinical Trials: A Questionnaire-Based Study of 179 Male Third- and Fourt...Med Sci Monit In Press; DOI: 10.12659/MSM.943468
08 Mar 2024 : Animal Research
Modification of Experimental Model of Necrotizing Enterocolitis (NEC) in Rat Pups by Single Exposure to Hyp...Med Sci Monit In Press; DOI: 10.12659/MSM.943443
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952








