29 March 2021: Clinical Research
A Real-World Study on the Use of the Alcohol Use Disorders Identification Test (AUDIT) in Men Admitted to a Psychiatric Hospital
Martin Anders1ADE, Eva Kitzlerová1BDE*, Sylva Racková2B, Václav Ćapek1ACDDOI: 10.12659/MSM.929667
Med Sci Monit 2021; 27:e929667
Abstract
BACKGROUND: This real-world study aimed to investigate the use of the Alcohol Use Disorders Identification Test (AUDIT) in men admitted to a psychiatric hospital.
MATERIAL AND METHODS: The AUDIT questionnaire (10 items) was consecutively administered for a period of 3 years to male patients admitted to a psychiatric hospital (n=636). Laboratory blood tests of biochemical parameters were measured as biomarkers of alcohol consumption. Data were evaluated using linear models with mixed effects in the case of continuous dependent variables and logistic regression models with mixed effects in the case of categorical dependent variables.
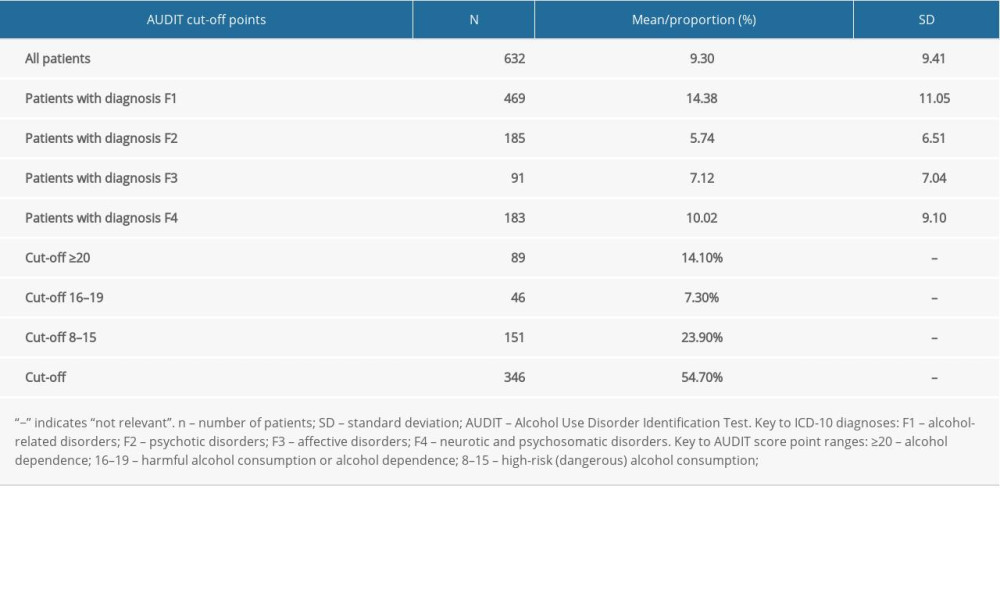
RESULTS: We found that 45.3% of the patients had a high risk of alcohol consumption or alcohol dependence and 54.7% had a low risk of alcohol consumption. The ICD-10 diagnoses of alcohol-related disorders (F1x), psychotic disorders (F2x), affective disorders (F3x), neurotic and psychosomatic disorders (F4x) were statistically significantly associated with total AUDIT score (P<0.001). There was a statistically significant association between the total AUDIT score and length of hospitalization (P=0.004) and the incidence of suicidal thoughts (P=0.003). Plasma concentrations of alanine aminotransferase (P=0.005), aspartate aminotransferase (P<0.001), gamma glutamyltransferase (P=0.001), total cholesterol (P=0.027) and mean corpuscular value of erythrocytes (P<0.001) were statistically significantly increased with a higher AUDIT score.
CONCLUSIONS: This real-world study showed that the AUDIT questionnaire evaluated the severity of disorders caused by alcohol and their impact on comorbid mental disorders. These results may be helpful in improving targeted interventions in this group of patients.
Keywords: Alcohol-Related Disorders, Pragmatic Clinical Trials as Topic, Mental Disorders, Substance Abuse Detection, Early Diagnosis, Alcohol Drinking, Alcoholism, Biometry, Czech Republic, Hospitalization, Hospitals, Psychiatric, Mass Screening, Surveys and Questionnaires
Background
HYPOTHESES AND AIMS:
The primary purpose of this study was to evaluate the use of the AUDIT questionnaire in a group of men admitted to a psychiatric hospital, measuring the severity of disorders caused by alcohol consumption and its impact on patients’ comorbid mental disorders and somatic health.
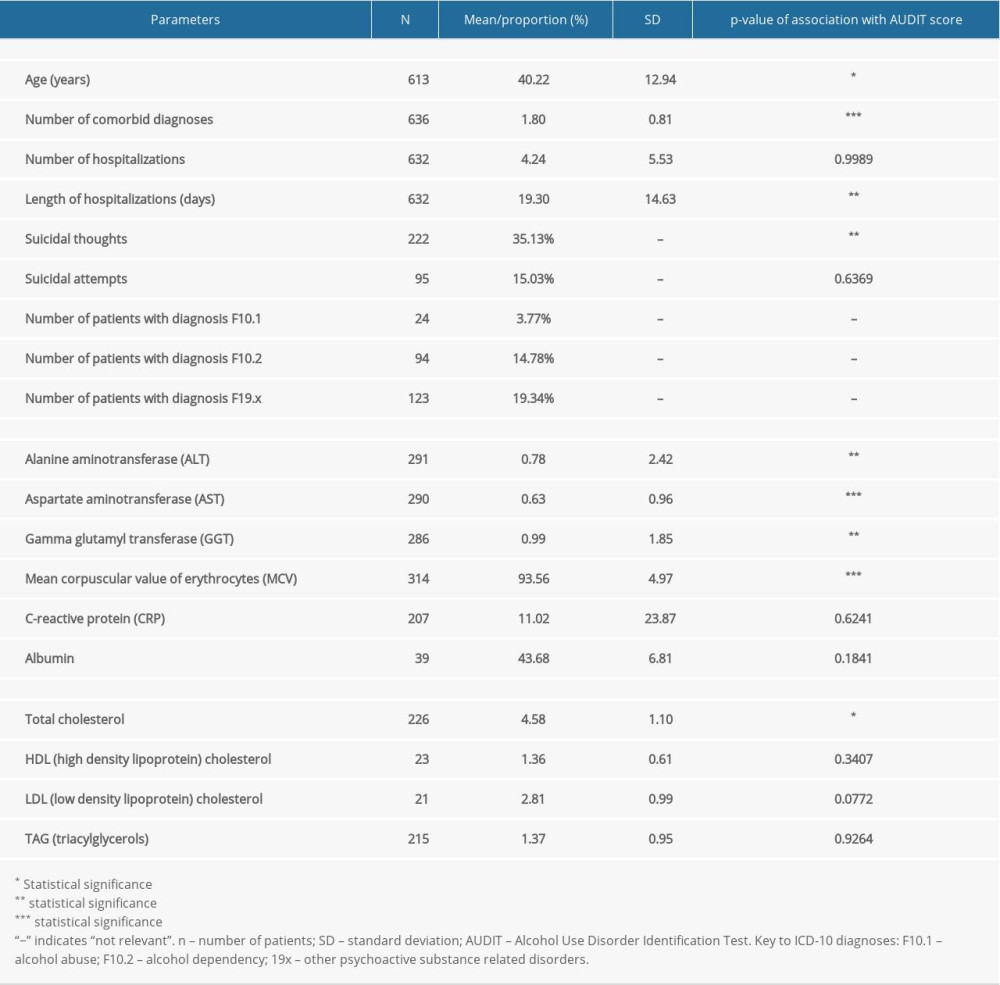
First, we evaluated the association of the total score of the AUDIT questionnaire with the following clinical comorbidities and demographic parameters: diagnosis, number of diagnoses (incidence of comorbidities), age, number of hospitalizations, length of hospitalization, occurrence of suicidal thoughts, and suicide attempts. Second, we evaluated the association of the total score in the AUDIT questionnaire with biochemical parameters (biomarkers) evaluating somatic health, including liver function tests (alanine aminotransferase [ALT], aspartate aminotransferase [AST], and gamma glutamyl transferase [GGT]), mean corpuscular value of erythrocytes (MCV), C-reactive protein (CRP), albumin, and lipid metabolism (total cholesterol, low-density lipoprotein (LDL) cholesterol, and high-density lipoprotein (HDL) cholesterol).
Further, we investigated the association between a higher total score in the AUDIT questionnaire and the presence of a diagnosis of alcohol abuse (ICD-10 F10.1), alcohol dependence (ICD-10 F10.2), or other psychoactive substance-related disorders (ICD-10 F 19.x).
Material and Methods
STATEMENT OF ETHICS:
Approval by an ethics committee and patient informed consent were not required by the authorities for this type of study in the Czech Republic. Patients included in this observational survey followed a standard examination algorithm. The AUDIT questionnaire was administered to patients as part of the initial examination to evaluate alcohol consumption. Laboratory examination, including the testing of basic biochemical parameters including liver enzymes as biomarkers for the detection of alcohol abuse or alcohol dependence, is recommended by guidelines for treatment of patients with mental disorders [30]. All included patients received information about the initial procedures and the evaluation of their consumption of alcohol and gave their oral consent to participate in the study.
STUDY SAMPLE AND PROCEDURE:
In this study, disorders caused by alcohol consumption (ICD-10 F1x) were evaluated according to the AUDIT questionnaire (10 items), which was consecutively administered for a period of 3 years to male patients (n=636) admitted to the Department of Psychiatry First Faculty of Medicine, Charles University and the General University Hospital in Prague, Czech Republic. The written version of the questionnaire was administered in the first 3 days after admission. The patients also completed a 28-day history of alcohol consumption.
Our male study population did not differ from the general male population in its common parameters. The description of the study sample, including biochemical parameters, is listed in Table 1. From the total number of included patients (n=636), 45.3% had high-risk alcohol consumption or alcohol dependence and 54.7% had low-risk alcohol consumption, according to the AUDIT total score (Table 2). Control participants were not included in the study.
Biochemical parameters from the patients’ peripheral blood laboratory examinations, such as plasma concentrations of liver enzymes (ALT, AST, and GGT), MCV, CRP albumin, and lipid metabolism (total cholesterol, LDL cholesterol, and HDL cholesterol) were measured as biomarkers of alcohol consumption and for assessment of the patients’ somatic health. Biomarkers were evaluated at the same time as patients completed the AUDIT questionnaire.
EVALUATION OF THE AUDIT QUESTIONNAIRE:
The evaluation of the AUDIT questionnaire responses was conducted as previously reported [22]. The answers in the questionnaire were assigned points ranging from 0 to 4. The points from the 10 items were then added together. The total score can range from 0 to 40 points. The higher the total score, the greater the patient’s problems with alcohol consumption.
A total score of 8 or more points is considered an indicator of high-risk and harmful alcohol consumption and potential alcohol dependence (the limit of 10 points provides higher specificity, but at the expense of the sensitivity of the test). Because the effect of alcohol fluctuates depending on average body weight and differences in metabolism, stipulating the limit for all women and men over the age of 35 as 1 level lower, for example to 7 points, increases the sensitivity of the test for this group.
INTERPRETATION OF CUTOFF POINTS:
The interpretation of the AUDIT questionnaire scores was conducted as previously reported [22]. The range of 0 to 7 points indicated low-risk alcohol consumption. Although no intervention is required in this range, guidance about alcohol use is suitable for many people because it contributes to general awareness of the risks related to alcohol use and has a preventive effect, which may be effective for people who indicated a lower level of consumption when completing the test.
The range of 8 to 15 points indicates high-risk or dangerous alcohol consumption. However, there may be individuals in the higher range of harmful alcohol consumption and dependence even in this range. The most suitable intervention is simple advice focused on limiting high-risk alcohol consumption.
The range of 16 to 19 points indicates harmful alcohol consumption or dependence. A score of 16 points or more corresponds to a high degree of problems with alcohol use. Patients in this range require a combination of simple guidance, concise advice, and consistent monitoring.
The range of 20 to 40 points indicates alcohol dependence. However, the AUDIT questionnaire is not a diagnostic instrument and therefore does not allow for the formal diagnosis of alcohol dependence; further diagnostic evaluation is required.
Given the lack of more accurate research findings, the above recommendations should be considered preliminary and should be subjected to clinical assessment, which takes into account the patient’s health, family anamnesis of problems with alcohol, and the patient’s truthfulness answering the questions in the AUDIT questionnaire. A clinical assessment is required to distinguish situations where the total score in the questionnaire may not represent the real level of risk, for instance, if a relatively low level of alcohol consumption conceals significant harmfulness or dependence. Likewise, the dividing points are not substantiated by a sufficient amount of evidence to be normative for all groups of individuals, and clinical decision making about interventions is necessary to best correspond to a patient’s individual situation [13].
A detailed analysis of an individual’s total score can be obtained by identifying the questions in which they obtained the most points. Generally, 1 or more points in question 2 or question 3, indicate a risky level of alcohol consumption. Points obtained from questions 4 to 6 (especially for weekly or daily symptoms) indicate existing or incipient alcohol dependence. Points obtained for questions 7 to 10 indicate that a patient’s health has already been damaged due to alcohol consumption.
STATISTICAL ANALYSIS:
Because some patients were hospitalized more than once, the acquired data were evaluated using linear models with mixed effects in the case of continuous dependent variables and by logistic regression with mixed effects in the case of categorical dependent variables (occurrence of suicidal thoughts and suicide attempts). As the random effect, the patient characteristics were considered. The continuous dependent variables were transformed using the Box-Cox type of transformation to meet the conditions of the models used. The analysis was conducted in the statistical package R version 3.5.1 [31].
Results
The total score of the AUDIT questionnaire was significantly associated (
Because alcohol abuse belongs to the common comorbidities of psychiatric disorders and can complicate the course of patients’ disorders and treatment [2–6], we analyzed the association between the total AUDIT score and the number of diagnoses of individual patients. The results showed that the total AUDIT score and number of comorbidity diagnoses were significantly associated (
Although alcohol consumption increased the incidence of mental disorders and affected their course and treatment, the results of this study did not show a significant association between the total AUDIT score and the number of hospitalizations (
We evaluated the association of alcohol consumption with the incidence of suicidal thoughts and suicide attempts. The total AUDIT score was significantly associated with the incidence of suicidal thoughts (
Further, we evaluated the association of the total AUDIT score with biochemical parameters (biomarkers) used to evaluate the patients’ somatic health. The total AUDIT score was significantly associated with plasma concentrations of ALT (
Alcohol consumption also affects the lipid spectrum and may lead to hyperlipoproteinemia. There was a statistically significant association between the total AUDIT score and concentration of total cholesterol (
The total AUDIT score was statistically significantly associated (
Discussion
The primary goals of this study were met. We have shown that half of the male patients included in this study had high-risk alcohol consumption and the number of comorbid mental disorders increased with the severity of alcohol consumption. Further, the somatic health of the included patients was assessed by biochemical measurements (Tables 1, 2).
The average age of the studied population was 40.2 years, and because the total AUDIT score declined with an increase in age, it can be assumed that younger patients in particular are at the greatest risk of having alcohol-related disorders. The ICD-10 diagnoses F1.x, F2.x, F3.x, and F4.x, for which the patients were hospitalized at a psychiatric hospital, were significantly associated with the total AUDIT scores, indicating the risk of or existence of alcohol abuse or alcohol dependence in these patients. Among the patients who were primarily hospitalized with alcohol-related disorders (F1x.x) (n=241), the proportion of the individual diagnoses were as follows: F10.1 (3.77%), F10.2 (14.78%), and F19.x (19.34%) (Table 1); the total AUDIT score showed a moderate degree of severity of these disorders. The total AUDIT score was also associated with the number of diagnoses patients had, demonstrating that the number of comorbid diagnoses increased with the increase in total questionnaire score (Table 1). Alcohol-related disorders represent very frequent comorbid diagnoses themselves. However, the more serious these alcohol-related disorders are, the greater is the risk of development of other mental disorders. Despite these facts, our study did not show any statistically significant association between the total AUDIT score and the number of hospitalizations (Table 1). On the contrary, a statistically significant association was identified between the length of hospitalization and total AUDIT score, with length of hospitalization decreasing with the increase in AUDIT score (Table 1). This may be because patients with more serious diagnoses of alcohol dependence, after receiving treatment for the acute phase of illness (usually within several days of hospitalization), were transferred for further treatment to a specialized addictology department, or more often were discharged prematurely, because of their low adherence or nonadherence to treatment.
We assessed the somatic health of patients using selected biochemical parameters (Table 1). The plasma concentrations of ALT, AST, and GGT increased with the increase in AUDIT questionnaire scores, which indicated a relationship between the severity of liver tissue damage and the severity of alcohol-related disorders. The mean values of plasma concentrations of liver enzymes in the studied population were within the limits of the broader normal population.
Our results did not show any association between the AUDIT score and albumin level. CRP levels tend to be elevated in the case of alcohol dependence, but our results did not show an elevation of CRP values with an increase in total AUDIT score.
Concerning the effects of alcohol on blood lipid levels, the regular consumption of even small doses of alcohol leads to the elevation of HDL cholesterol, which has a protective effect on cardiovascular functions. However, alcohol consumption very often leads to secondary hyperlipoproteinemia. In our evaluation, only total cholesterol was significantly increased with the increase in AUDIT score, and the protective effect of HDL cholesterol was not shown.
The increased MCV of erythrocytes was found in our study. The range of the MCV of erythrocytes is 98 to100 fL in the case of long-term alcohol abuse and is normalized only after a significant period of abstinence lasting from 2 to 4 months [11,14].
The WHO developmental study of AUDIT [32] evaluated the relationship of AUDIT scores to commonly used biochemical measures of excessive alcohol use. In a sample of patients in the United States who had been drinking in the past year, the AUDIT was associated with the low to moderate range of GGT, AST, ALT, and macrocytic volume, which is comparable with our results. Interestingly, the associations tended to be higher for women than for men [33].
Of some relevance as well, in a large-scale trial among general hospital patients in Mexico, 44% of those with AUDIT scores of at least 8 also had serum GGT levels >50 mmoL/L, the conventional normal cutoff range for GGT [34].
The study of Tsai et al in 2005 showed that, in a Chinese population, men had significantly higher AUDIT and AUDIT-C scores than did women and were also significantly more likely than women to be diagnosed as harmful or alcohol-dependent users [24]. The relationships between AUDIT scores and distal drinking consequences tended to also be higher for men than for women. The reasons for this are unclear; it may reflect different ages of onset of problem drinking and varying patterns and levels of alcohol consumption [33].
Our study had some limitations. First, our real-world study included only men. This restriction may limit the study results. However, there is no comparison with women because only men hospitalized at the psychiatric hospital were examined. We plan to conduct the same research in the same sized group of women in the near future. Second, a control group was not used in the study. Third, research was conducted only at a single research center. However, it must be emphasized that this study is not a comparative, multicenter study. It was designed as a cross-sectional, observational survey mapping the common practice with consecutively admitted patients to the psychiatric department with acute mental disorders. Finally, limitations of the main study methods used were based on the health status and cooperation of patients after their admission and their abilities to truthfully provide information about their alcohol consumption.
Conclusions
In this study, we mapped the alcohol consumption and determined the alcohol-related disorders of male patients hospitalized at a psychiatric hospital using the easy-to-administer AUDIT questionnaire and biomarker measurements. We have shown that about half of all male patients admitted to a psychiatric hospital with ICD-10 diagnoses of F1x.x, F2x.x, F3x.x, and F4x.x have high-risk alcohol consumption or alcohol dependence. The younger patients were at the greatest risk. The number of hospitalizations was not related to AUDIT score, whereas the length of hospitalizations decreased with the severity of the alcohol abuse. The plasma concentrations of liver enzymes, total cholesterol, and MCV were statistically significantly associated with the total AUDIT questionnaire score.
These findings from this real-world study showed that the AUDIT questionnaire effectively evaluated the severity of disorders caused by alcohol and the impact on comorbid mental disorders. These results may be helpful in improving targeted interventions in this group of patients.
References
1. Racková S, Kitzlerová E, Anders M, Raboch J, Screening evaluation of the degree of severity of alcohol abuse: Česká a Slovenská Psychiatrie, 2018; 114(1); 24-28
2. Boschloo L, Vogelzangs N, Smit JH, Comorbidity and risk indicators for alcohol use disorders among persons with anxiety and/or depressive disorders: Findings from the Netherlands Study of Depression and Anxiety (NESDA): J Affect Disord, 2011; 131(1–3); 233-42
3. Boschloo L, Vogelzangs N, Smit JH, The performance of the Alcohol Use Disorder Identification Test (AUDIT) in detecting alcohol abuse and dependence in a population of depressed or anxious persons: J Affect Disord, 2010; 126(3); 441-46
4. Boden JM, Fergusson DM, Alcohol and depression: Addiction, 2011; 106(5); 906-14
5. Gimeno C, Dorado ML, Roncero C, Treatment of comorbid alcohol dependence and anxiety disorder: Review of the scientific evidence and recommendations for treatment: Front Psychiatry, 2017; 22(8); 173
6. Iovieno N, Tedeschini E, Bentley KH, Antidepressants for major depressive disorder and dysthymic disorder in patients with comorbid alcohol use disorders: A meta-analysis of placebo-controlled randomized trials: J Clin Psychiatry, 2011; 72(8); 1144-51
7. Schoepf D, Heun R, Alcohol dependence and physical comorbidity: Increased prevalence but reduced relevance of individual comorbidities for hospital-based mortality during a 12.5-year observation period in general hospital admissions in urban North-West England: Eur Psychiatry, 2015; 30(4); 459-68
8. Cornelius JR, Chung TA, Douaihy AB, A review of the literature of mirtazapine in co-occurring depression and an alcohol use disorder: J Addict Behav Ther Rehabil, 2016; 5(4); 159
9. Pompili M, Serafini G, Innamorati M, Suicidal behavior and alcohol abuse: Int J Environ Res Public Health, 2010; 7(4); 1392-431
10. Masferrer L, Caparrós B, Risk of suicide and dysfunctional patterns of personality among bereaved substance users: Int J Environ Res Public Health, 2017; 14(3); 316
11. Samokhvalov AV, Popova S, Room R, Disability associated with alcohol abuse and dependence: Alcohol Clin Exp Res, 2010; 34; 1871-78
12. Dawson DA, Alcohol consumption, alcohol dependence, and all-cause mortality: Alcohol Clin Exp Res, 2000; 24; 72-81
13. Laramée P, Kusel J, Leonard S, The economic burden of alcohol dependence in Europe: Alcohol Addiction, 2013; 48; 259-69
14. Schomerus G, Lucht M, Holzinger A, The stigma of alcohol dependence compared with other mental disorders: A review of population studies: Alcohol Addiction, 2011; 46; 105-12
15. Ösby U, Liljenberg J, Kockum I, Genes and alcohol: Eur Psychiatry, 2010; 25(5); 281-83
16. Saunders JB, Aasland OG, Babor TF, Development of the alcohol use disorders identification test (AUDIT): WHO collaborative project on early detection of persons with harmful alcohol consumption-II: Addiction, 1993; 88; 791-804
17. Pal HR, Jena R, Yadav D, Validation of the alcohol use disorders identification test (AUDIT) in urban community outreach and de-addiction center samples in North India: J Stud Alcohol, 2004; 65; 794-800
18. Benegal V, India: Alcohol and public health: Addiction, 2005; 100; 1051-56
19. Glass JE, Hamilton AM, Powell BJ, Specialty substance use disorder services following brief alcohol intervention: A meta-analysis of randomized controlled trials: Addiction, 2015; 110; 1404-15
20. Allen J, Litten R, Fertig J, Babor T, A review of research on the Alcohol Use Disorders Identification Test (AUDIT): Alcohol Clin Exp Res, 1997; 21; 613-19
21. Boschloo L, Vogelzangs N, Smit J, The performance of the Alcohol Use Disorder Identification Test (AUDIT) in detecting alcohol abuse and dependence in a population of depressed or anxious persons: J Affect Disord, 2010; 126; 441-46
22. Babor TF, Higgins-Biddle JC, Saunders JB, Monteiro MG, AUDIT: The Alcohol Use Disorders Identification Test: Guidelines for use in primary care, 2001, Geneva, World Health Organization
23. Fiellin DA, Carrington RM, O’Connor PG, Screening for alcohol problems in primary care: A systematic review: Arch Intern Med, 2000; 160; 1977-89
24. Tsai MC, Tsai YF, Chen CY, Liu CY, Alcohol Use Disorders Identification Test (AUDIT): Establishment of cut-off scores in a hospitalized Chinese population: Alcohol Clin Exp Res, 2005; 29; 53-57
25. Kokotailo PK, Egan J, Gangnon R, Validity of the Alcohol Use Disorders Identification Test in college students: Alcohol Clin Exp Res, 2004; 28; 914-19
26. Hays RD, Merz JF, Nicholas R, Response burden, reliability, and validity of the CAGE, Short MAST, and AUDIT alcohol screening measures: Behav Res Methods Instrum Comput, 1995; 27; 277-80
27. Sinclair M, McRee B, Babor TF: Evaluation of the Reliability of AUDIT, 1992, University of Connecticut School of Medicine, Alcohol Research Center (unpublished report)
28. Allen JP, Reinert DF, Volk R, The Alcohol Use Disorders Identification Tests: An aid to recognition of alcohol problems in primary care patients: Prev Med, 2001; 33; 428-33
29. Nadkarni A, Weiss HA, Velleman R, Feasibility, acceptability and cost-effectiveness of a brief, lay counsellor-delivered psychological treatment for men with alcohol dependence in primary care: An exploratory randomized controlled trial: Addiction, 2019; 114; 1192-203
30. Raboch J, Anders M, Hellerova P, Doporučené postupy psychiatrické péče IV: Česká Psychiatrická Společnost JEP, 2010 [in Czech]
31. R Core Team: A language and environment for statistical computing, 2018, Vienna, Austria, R Foundation for Statistical Computing https://www.R-project.org/
32. Saunders JB, Aasland OG, Babor TF, Development of the Alcohol Use Disorders Identification Test (AUDIT): WHO collaborative project on early detection of persons with harmful alcohol consumption. Part 11: Addiction, 1993; 88; 791-804
33. Bohn MJ, Babor TF, Kranzler HR, The Alcohol Use Disorders Identification Test (AUDIT): Validation of a screening instrument for use in medical settings: J Stud Alcohol, 1995; 56; 423-32
34. Guevara-Arnal L, Zapata L, Kaplan M, Alcohol-related studies group: Hazardous alcohol consumption among Mexican inpatients: A multicenter study: Am J Addict, 1995; 4; 170-76
In Press
21 Mar 2024 : Meta-Analysis
Economic Evaluation of COVID-19 Screening Tests and Surveillance Strategies in Low-Income, Middle-Income, a...Med Sci Monit In Press; DOI: 10.12659/MSM.943863
10 Apr 2024 : Clinical Research
Predicting Acute Cardiovascular Complications in COVID-19: Insights from a Specialized Cardiac Referral Dep...Med Sci Monit In Press; DOI: 10.12659/MSM.942612
06 Mar 2024 : Clinical Research
Enhanced Surgical Outcomes of Popliteal Cyst Excision: A Retrospective Study Comparing Arthroscopic Debride...Med Sci Monit In Press; DOI: 10.12659/MSM.941102
06 Mar 2024 : Clinical Research
Prevalence and Variation of Medical Comorbidities in Oral Surgery Patients: A Retrospective Study at Jazan ...Med Sci Monit In Press; DOI: 10.12659/MSM.943884
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952