30 November 2021: Animal Study
Moxibustion Regulates Gastrointestinal Motility via HCN1 in Functional Dyspepsia Rats
Hong-ling Xiao12ABCDEF, Yun-jiu Xiao3BCD, Qian Wang3BCD, Mei-ling Chen3BCD, An-li Jiang1ABCD*DOI: 10.12659/MSM.932885
Med Sci Monit 2021; 27:e932885
Abstract
BACKGROUND: Moxibustion therapy has been found to ameliorate clinical symptoms of functional dyspepsia (FD). We aimed to examine the regulatory effect of moxibustion on the gastrointestinal (GI) motility in FD and explore the underlying mechanism based on the hyperpolarization-activated cyclic nucleotide-gated cation channel 1 (HCN1).
MATERIAL AND METHODS: Moxibustion therapy was used in FD rats induced by using classic tail-pinch and irregular feeding. Weight gain and food intake were recorded weekly, followed by detecting gastric residual rate (GRR) and small intestine propulsion rate (IPR). Next, western blotting was performed to determine the expression levels of HCN1 in the gastric antrum. qRT-PCR was used to detect HCN1 in the small intestine and hypothalamic satiety center. Double immunolabeling was used for HCN1 and ICCs in gastric antrum and small intestine.
RESULTS: The obtained results suggested that moxibustion treatment could increase weight gain and food intake in FD rats. The GRR and IPR were compared among the groups, which showed that moxibustion treatment could decrease GRR and increase IPR. Moxibustion increased the expression of HCN1 in the gastric antrum, small intestine, and hypothalamic satiety center. Histologically, the co-expressions of HCN1 and ICCs tended to increase in gastric antrum and small intestine. Meanwhile, HCN channel inhibitor ZD7288 prevented the above-mentioned therapeutic effects of moxibustion.
CONCLUSIONS: The results of the present study suggest that moxibustion can effectively improve the GI motility of FD rats, which may be related to the upregulation of HCN1 expression in gastric antrum, small intestine, and satiety center.
Keywords: Dyspepsia, Gastrointestinal Motility, Hyperpolarization-Activated Cyclic Nucleotide-Gated Channels, Moxibustion, Animals, Disease Models, Animal, Potassium Channels, Rats
Background
Functional dyspepsia (FD) is a prevalent gastrointestinal (GI) disorder in adults, with a global incidence of 40% based on the Rome IV criteria [1–4]. It is characterized by chronic or recurrent symptoms, including early satiation, postprandial fullness, epigastric pain, and unreasonable burning sensation. FD affects all major dimensions of health-related quality of life in the general population, including physical, mental, and social aspects [5,6]. Although prokinetics, antacids, and antidepressants are available to treat FD, adverse effects and drug resistance necessitate the development of novel therapies [7,8].
GI motor dysfunction, visceral hypersensitivity,
The presence of HCN has been widely reported in the ICCs, which can generate a basic slow electrical rhythm that modulates the phasic contractions of gastrointestinal smooth muscle cells [20]. Reported studies have shown the role of HCN in gastrointestinal peristalsis, with an elevated expression of HCN1–2 in the GI tract [21,22]. HCN1, as the starting channel for spontaneous electric rhythm, is specifically expressed on the ICCs [20,23,24]. Blocking HCN channels caused vomiting in least shrews, according to Zhong and Darmani [25]. The medial hypothalamus nuclear satiety center regulates GI motility, and the HCN1 channel expressed in the hypothalamic nuclei plays a key role in the CNS. However, the underlying pathophysiology of HCN1 is not fully understood.
Moxibustion therapy is based on traditional Chinese medicine. It uses burning moxa leaves as medicinal materials and uses its thermal, radiological, and pharmacological effects to stimulate specific acupuncture points and meridians to prevent and treat diseases [26–29]. It has been reported that moxibustion can regulate visceral and endocrine functions, improve metabolism, enhance immune function, regulate GI motility, and reduce anxiety [30–33]. Moxibustion is a simple, cheap, safe, non-invasive, painless, self-administered technique for the treatment of FD. Moxibustion has been shown to be effective in the treatment of FD in previous studies, but its underlying mechanism is not fully understood [34,35]. The present study was undertaken to observe the regulatory effect of moxibustion on GI motility and explore the targeted role of HCN1 in regulation of GI motility in FD rats.
Material and Methods
EXPERIMENTAL ANIMALS:
In vivo experiments were conducted according to the Guideline for Animal Experimentation of the Anhui University of Chinese Medicine. Adult Sprague-Dawley (SD) rats weighing 200±20 g were purchased from the Hunan STJ Laboratory Animal Co., Ltd. (Hunan, China; License No. SCXK [Xiang] 2019–0004). All the animals were housed in a specific pathogen-free environment at 23–25°C with 50–70% humidity and 12-h light/dark cycle and given ad libitum access to food and water. Body weights were recorded weekly throughout the study period. The experimental protocols of the study were approved by the Institutional Animal Ethics Committee (No. 20200013).
After 7 days of acclimatization, rats (n = 50) were randomly divided into 5 groups (n=10 per group): normal (N), model (M), domperidone (MD) (control group), moxibustion (MM), and HCN blocker (MB).
ESTABLISHMENT OF FD MODEL:
The FD models were established in all groups except for the N group, using classic tail-pinch and irregular feeding [36]. Gauze-wrapped hemostatic forceps were used to clamp the first third of the tail and then they were immediately released to provoke the mice to fight for 30 min, twice daily (9 AM and 6 PM). If skin lesions were caused by clamping or fighting, the skin was disinfected with 2% iodophor to prevent secondary infection. Animals were fasted on Wednesdays, Fridays, and Sundays. Animals received tail pinching and irregular feeding for 4 weeks.
HCN CHANNEL BLOCKING:
HCN channel inhibitor ZD7288 (1 mL, Tocris Bioscience, UK) in normal saline (0.5 mM) was intravenously injected in the MB group rats, and an equal amount of normal saline was injected in the remaining groups before moxibustion [37].
ESTABLISHMENT OF POSITIVE CONTROL:
The rats in the MD group were given 2 mL of domperidone (Xian Janssen, China) solution (0.5 mg/ml) per day, while the other rats were given an equal amount of normal saline.
MOXIBUSTION TREATMENT:
Moxibustion points ST36 (Zusanli) and RN12 (Zhongwan) were selected based on the principles and practice of traditional Chinese medicine for treating FD. Moxibustion was performed by trained operators. ST36 was located 5 mm below and lateral to the anterior tubercle of the tibia in adult rats, and RN12 was located at the midpoint of the midline of the upper abdomen of adult rats. After the head, tail, and limbs of rats were fixed, the hair around the acupoints was shaved to expose the local skin before application. Moxibustion sticks (containing 3-year-old pure moxa, 0.5×12 cm, Nanyang Hanyi Moxa Co., China) were burned aimed approximately 2–3 cm over the acupoints aiming at ST36 and RN12 of rats in the MM and MB groups to avoid skin burns, which may be associated with the stress response. The moxibustion treatments were performed for 20 min per day at 7: 00–9: 00 AM for 2 weeks in a row, with a 1-day rest on the seventh day of each week [33,38]. Rats in other groups received the above procedures except for moxibustion.
WEIGHT GAIN AND FOOD INTAKE:
To observe the difference between the groups more intuitively, we used gained weight to assess the influence of moxibustion. The body weights and food intake were recorded once weekly. Weight gain (g)=weight measured this week–weight measured last week.
DETECTION OF GASTRIC RESIDUE AND INTESTINAL PROPULSION:
Sugar (8 g), milk powder (16 g), activated carbon powder (2 g), and starch (8 g) were added to carboxymethylcellulose sodium (10 g; Sangon, China) in normal saline (250 mL), followed by vortexing. Then, the volume was adjusted to 300 mL black semi-solid paste with normal saline.
Rats were fasted for 12 h and then administered black semi-solid paste (100 g/mL) via oral gavage. After 30 min, rats were sacrificed by cervical dislocation. The cardia and pylorus were ligated after laparotomy, and the stomach was collected, weighed, and measured. The stomach was then opened along the larger curvature, and the contents were washed out, and the empty stomach was weighed again. Also, the small intestine was collected, and the distance traveled by the semi-solid paste and the total length of the small intestine were measured. The gastric residue rate (GRR) and intestinal propulsion rate (IPR) were calculated as follows: GRR (%)=(total stomach weight-empty stomach weight)/semi-solid paste quality×100; IPR (%)=distance traveled by semi-solid paste/total length of small intestine×100.
SAMPLE COLLECTION AND PROCESSING:
At the end of week 6, rats were sacrificed by cervical dislocation, and the gastric antrum tissues above the greater curvature, upper segments of the small intestine, and the ventromedial nucleus of the hypothalamus (satiety center) were collected and stored in liquid nitrogen.
WESTERN BLOTTING:
Total proteins were extracted from gastric tissues (gastric antrum above the greater curvature). The proteins (100 μg) were fractionated by using a NATIVE-PAGE, and then transferred onto a PVDF membrane. Next, the membrane blockage was performed with 5% skimmed milk. After washing, the membranes were incubated for 1.5 h with an anti-HCN1 antibody (ab176304, Abcam; 1: 1000). After washing 3 times with TBST (5 min each time), the membranes were incubated with secondary antibody conjugated with horseradish peroxidase (ab205718, Abcam; 1: 1000) for 1.5 h and then visualized using an ECL reagent kit (Pierce/Thermo Scientific). The optical density of each band was analyzed using Image J software (Labworks™ Analysis Software, USA). The expression of HCN1 was normalized to that of internal reference.
QUANTITATIVE RT-PCR:
TRIzol reagent was used to extract total RNA from the upper small intestine and hypothalamic medial nucleus. Then, a reverse transcription system (Bio-Rad, USA) was used to quantify RNA concentrations. Quantitative RT-PCR was conducted using a fluorescence quantitative PCR reaction system (Bio-Rad, USA). The primers used were:
IMMUNOFLUORESCENCE DOUBLE STAINING OF C-KIT AND HCN1 IN HASTRIC AND INTESTINAL TISSUES:
The paraffin embedded tissues were cut into 5-μm sections, which were then processed for immunofluorescence staining. The antibodies included anti-c-kit (ab32363, Abcam; 1: 150), anti-HCN1 (ab176304, Abcam; 1: 150), goat anti-rabbit IgG H&L (Cy3®) pre-adsorbed (ab6939, Abcam; 1: 800), and anti-c-Myc [Y69] (FITC) (ab223913, Abcam; 1: 800) antibodies. After staining with DAPI in the dark, the images were observed and captured using a laser scanning confocal microscope.
STATISTICAL ANALYSIS:
Statistical analyses were performed using SPSS version 21.0 and the obtained data were expressed as mean±standard deviation. Results of food intake, weight gain, gastric residual rate, intestinal prolapse ratio, RT-qPCR, and western blot were analyzed by one-way ANOVA, with intervention as the influencing factor. The LSD test was used for further pair comparison between groups, and Tamhane’s T2 test was used for uneven variances. The selected rank-sum test was used for comparing groups that did not conform to normal distribution, and the Kruskal-Wallis test was used for further pairwise comparison. A value of
Results
EFFECT OF MOXIBUSTION ON WEIGHT GAIN:
According to the obtained results, moxibustion improved the weight gain of FD rats. The FD model was successfully established in rats at week 4, with substantially less weight gain in the M, MD, MM, and MB groups than in the N group (Figure 1A). Rats in the MD and MM group exhibited substantially more weight gain than in the M group at weeks 5 and 6, suggesting that the effect of moxibustion on the weight gain of FD rats was similar to that of domperidone. Moxibustion’s effect on weight gain in FD rats was inhibited after HCN inhibition, suggesting a possible role for HCN in the effect of moxibustion on weight gain in FD rats.
EFFECT OF MOXIBUSTION ON FOOD INTAKE:
To assess the effect of moxibustion on food intake, rats in each group were chosen with similar food intake patterns. The results revealed a significant difference between group N and other groups after establishment of the FD model (Figure 1B). The MM and MD groups showed substantially increased food intake at weeks 5 and 6 than in the FD group (P<0.001). Thus, both moxibustion and domperidone could improve the food intake of FD rats. The food intake in the MM group significantly increased as compared to the MB group, but it was markedly lower than that in the MD group (P<0.01) during the study period.
EFFECT OF MOXIBUSTION ON GRR AND IPR:
After establishment of the FD model, significant GRR increase and an IPR decrease were observed in the M group, as compared to the N group (P<0.001), while the MM and MD groups showed a significantly decreased GRR and an increased IPR when compared to the M group (
EFFECT OF MOXIBUSTION ON HCN1 PROTEIN EXPRESSION IN GASTRIC ANTRUM TISSUES:
According to the obtained results, moxibustion improved HCN1 protein expression in the gastric antrum tissues (Figure 2). There was a marked difference in the HCN1 protein expression between the N and the M group (P<0.001). In addition, HCN1 expression in the MM group was significantly higher than in the M and MB groups (P<0.01; P<0.05, respectively), but markedly lower than in the MD group (P<0.001). This indicates that moxibustion could enhance the HCN1 protein expression of FD rats, but failed to increase HCN1 protein expressions after HCN1 inhibition. The double immunofluorescence staining of HCN1 and c-kit in the gastric antrum above the greater curvature showed the expressions of HCN1 and c-kit were lower in the M group than in the N group (red, c-kit; Green, HCN1; Blue, DAPI), and the expressions of HCN1 and c-kit in the MM group and MD group were higher than in the M group and MB group (Figure 3). Quantitative analysis showed that the increase was statistically significant for c-kit and HCN1 (Figure 4A). The obtained results suggest that moxibustion can improve HCN1 level in the gastric antrum of FD rats.
EFFECT OF MOXIBUSTION ON HCN1 EXPRESSION IN THE INTESTINE:
Moxibustion enhanced the HCN1 expressions in the upper segments of the small intestine in FD rats (Figure 5A). After the establishment of the rat FD model, there was a marked difference in HCN1 expression between the N and the M group (P< 0.001). HCN1 expression in the MM group was significantly higher than in the M (P<0.001) and MB groups (P<0.01), but lower than in the MD group (P<0.001). The double immunofluorescence staining of HCN1 and c-kit in the upper small intestine showed that co-expressions of HCN1 and c-kit were lower in the M group than in the N group, and the co-expressions in the MM group and MD group were higher than in the M and MB groups (Figure 6). Quantitative analysis showed that the increase was statistically significant for c-kit and HCN1 (Figure 4B).
EFFECT OF MOXIBUSTION ON HCN1 EXPRESSION IN THE SATIETY CENTER OF THE HYPOTHALAMUS:
Moxibustion increased HCN1expression in the satiety center of the hypothalamus of FD rats (Figure 5B). There was a marked difference in HCN1 expression between the N group and the M group (P<0.001). HCN1 expression was significantly higher in the MM group than in the M (P<0.001) and MB group (P<0.01), but it was markedly lower than in the MD group (P<0.001). HCN1 expression was similar in the hypothalamus and intestine.
Discussion
FD causes recurrent or persistent dyspeptic symptoms, including postprandial fullness, early satiation, epigastric pain, and burning sensation that originates in the gastroduodenal region. In this study, we proposed that moxibustion had a therapeutic effect on FD via modulating GI motility through the HCN1 channel. The hypothesis was validated at molecular (HCN1 expression in the antrum, small intestine, and satiety center), cellular (HCN1 co-expression with c-kit in the antrum and small intestine), organ (gastric residual rate and intestinal propulsion ratio), and organism (weight gain and food intake) levels in animal experiments.
Although there are various methods for establishing FD rat models, the classic two-factor method of tail-pinch and irregular feeding is generally accepted at present [36]. To acquire a better understanding of the pathophysiology of FD, we used the standard two-factor procedure of tail-pinch and irregular feeding to generate the FD model. Reported studies have revealed that anxiety and depression are positively correlated with the severity of FD [39]. Tail-pinch stimulation induces a chronic stress response in rats through physical and psychological stress, which is similar to psychosocial stress inducement in FD patients. Irregular feeding simulates the main cause of irregular eating in FD patients. The times of tail-pinch stimulation were twice per day for 4 weeks. The daily amount of stimulation was reduced and the modeling period was longer, which was more consistent with the onset characteristics of FD chronic stress. FD model rats showed significantly increased GRR and decreased IPR, indicating that the FD models were successfully established.
In recent decades, it has been revealed that the hyperpolarization-activated cyclic nucleotide-gated cation channel (HCN) is a voltage-gated ion channel that works in a time-dependent manner [40,41]. The HCN channels consist of 4 subunits (HCN1–4). HCN is similar in structure to voltage-dependent potassium channels and cyclic adenylate gated channels, and it consists of 3 parts: the N-terminal, the transmembrane segment (S1~S6), and the C-terminal of the region bound to cyclic nucleotides. They are pacemaker channels of pacemaker cells, closing during depolarization and opening during hyperpolarization [40]. HCN channels are found in both neuronal and non-neuronal cells, where they play a variety of physiological roles, including pain perception, neuronal pacing, and dendritic integration. They are also involved in the pathogenesis of a variety of CNS disorders and pathological states [42–46], as well as regulating rhythmic activity of the heart and brain [47]. Cs+ and ZD7288 can inhibit HCN channels, while cAMP can stimulate them. Studies have shown that overexpression of HCN1 channels in bladder ICCs is associated with the occurrence of bladder hyperactivity [48]. There is growing evidence that the HCN1 channel is responsible for GI motility. In the present study, the presence of HCN1 in the ICCs of gastric antrum (Figure 3) and upper small intestine (Figure 6) was confirmed by double immunofluorescence staining of HCN1 and c-kit. Quantitative analysis showed that moxibustion could enrich the co-expression of HCN1 and c-kit (Figure 4). The HCN1 channel is also expressed in the satiation center, in which neural signaling is related to food intake. We used QRT-PCR to confirm the expression of HCN1 in satiety centers (Figure 5B).
Moxibustion is a common method of treating FD in Southeast Asia, and it is verified by thousands of years of clinical practice. Through warm and near-infrared stimulation, the effective substances of moxa penetrate local acupuncture points, transmit into the human body meridian, improve GI motility disorders, and repair body abnormalities [49]. In this study, moxibustion was found to have a substantial therapeutic impact on FD rats. The weight gain and food intake were significantly increased in the MM group, as shown in Figure 1. GRR and IPR are important indicators that improve the symptoms of early satiety and abdominal distention in patients with FD. Figure 7 shows that moxibustion can significantly reduce the gastric residual rate and increase the intestinal propulsion ratio in FD rats. These results demonstrated that moxibustion had a beneficial effect on FD. To explore the role of HCN, we added an HCN channel blocking group. The effects of moxibustion on weight gain and food intake in FD rats were dramatically reduced by blocking HCN channels with ZD7288, and the effects of moxibustion on reducing GRR and improving IPR were also significantly affected. The results suggested that HCN channels played a critical role in treating FD rats with moxibustion.
To further explore the role of the HCN1 channel in regulating gastrointestinal movement, western blotting was used to detect the expression of HCN1 protein in the gastric antrum, showing that moxibustion could significantly increase the expression of HCN1 protein in FD rats, as shown in Figure 2. qRT-PCR was used to detect the expression of the HCN1 channel in the upper small intestine (Figure 5A) and the satiation center (Figure 5B), and it was found that moxibustion could significantly increase the expression of HCN1 in the small intestine and the satiation center of FD rats. Moreover, moxibustion significantly enhanced the co-expression of c-kit and HCN1, and the co-expression was significantly decreased when HCN1 was blocked (Figure 4). This study confirmed that HCN1 was as important in the pacing of GI ICCs as HCN1 was in bladder ICCs [48]. Increased HCN1 can activate GI ICCs, and ICCs pacemaker slow waves enhanced GI motility. In addition, increased HCN1 can stimulate the hypothalamus satiety center, which acts on the GI tract to regulate GI motility. Increased GI peristalsis resulted in decreased GRR and increased IPR. The present results suggest that moxibustion probably regulated GI motility in FD rats through HCN1 target, which may be the common mechanism in the hypothalamus and GI tract.
In the present experiment, domperidone had greater significantly influences on weight gain, food intake, and GRR and HCN1 expression in the gastric antrum, small intestine, and satiation center than moxibustion. But there was no difference in PIR between domperidone and moxibustion, perhaps because moxibustion stimulates the maximum physiological potential via “benign stimulation” with very little energy sent to the overall bidirectional regulation of body balance. When this regulation reaches the body’s balance, the effect of mild stimulus gradually diminishes. Therefore, the effect of this benign stimulation of moxibustion will not accumulate in the body and produce adverse effects. As domperidone directly blocks dopamine receptors and mainly works on the stomach, its effect on PIR is relatively weak and long-term use can have adverse effects [50].
There were some limitations in this study. The treatment period was short and the expression of HCN is not adequately presented. Moreover, recent studies have found that HCN2 and HCN4 also play a role in regulating gastrointestinal motility, and their role in the treatment of FD by moxibustion remains to be further explored. More studies with long-term treatment are needed to confirm our findings. In addition, electrophysiological examinations may be employed to assess gastric and intestinal function.
Conclusions
We found that moxibustion can effectively improve FD by enhancing GI motility, which may be related to the regulation of HCN1 expression in the ICCs of the GI and the satiety center of the hypothalamus.
Figures
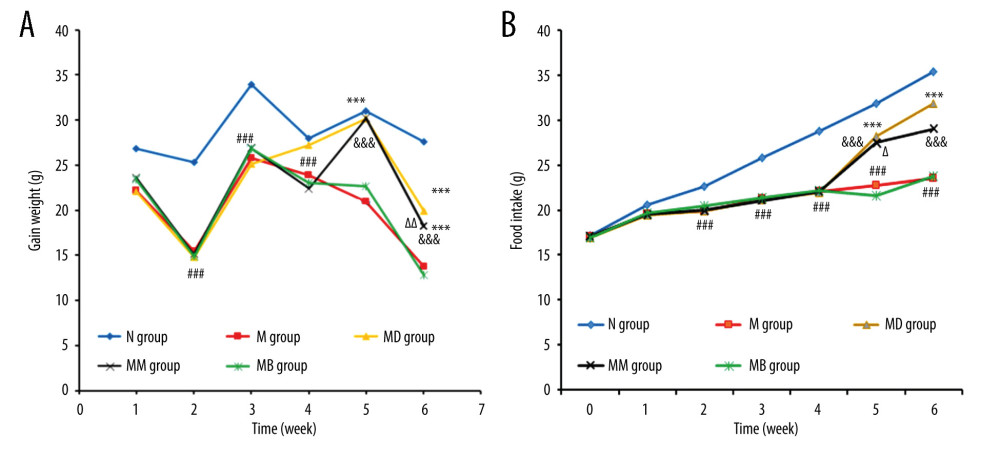 Figure 1. The weight gain (A) and food intake (B) of rats (n=10/group) (mean±SEM). ### P<0.001 vs N group; ** P<0.001 vs M group; Δ P<0.05, ΔΔ P<0.01 and ΔΔΔ P<0.001 vs MD; &&& P<0.001 vs MB group.
Figure 1. The weight gain (A) and food intake (B) of rats (n=10/group) (mean±SEM). ### P<0.001 vs N group; ** P<0.001 vs M group; Δ P<0.05, ΔΔ P<0.01 and ΔΔΔ P<0.001 vs MD; &&& P<0.001 vs MB group. 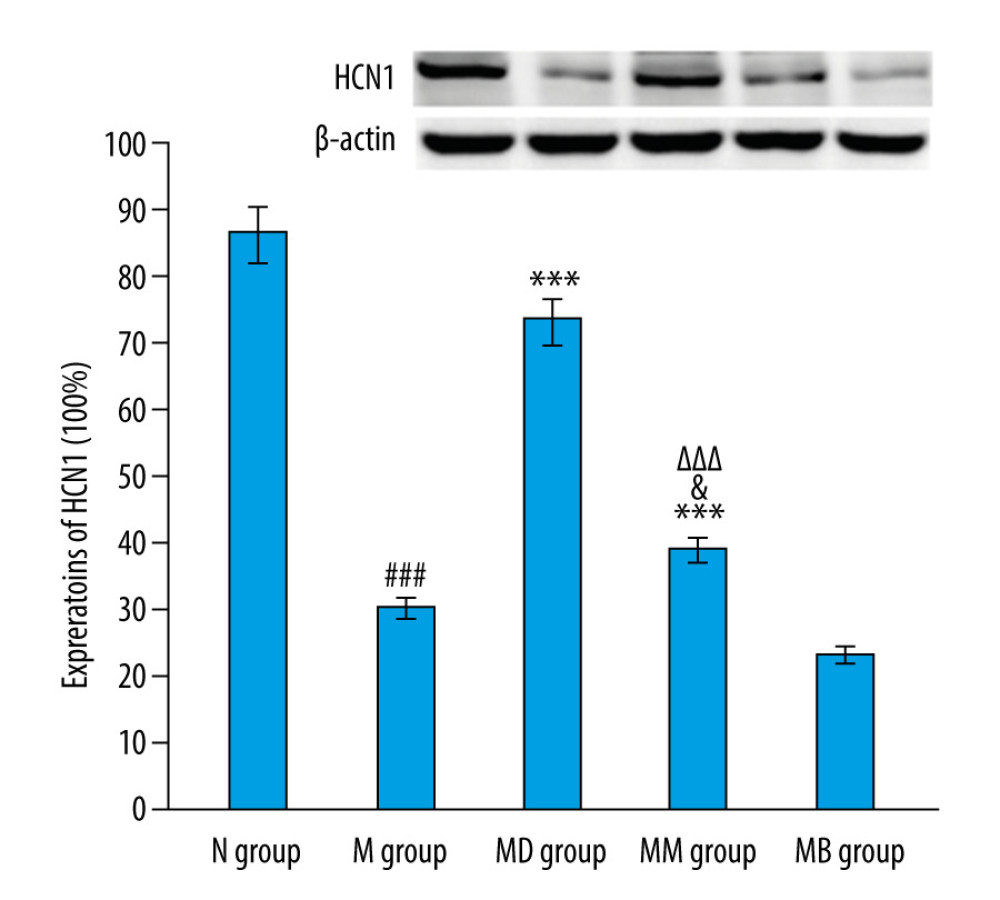 Figure 2. HCN1 expression in the gastric antrum tissues of rats by western blotting (n=4/group). (mean±SEM). ### P<0.001 vs N group;** P<0.01and *** P<0.001 vs M group; ΔΔΔ P<0.001 vs MD group; & P<0.05 vs MB group.
Figure 2. HCN1 expression in the gastric antrum tissues of rats by western blotting (n=4/group). (mean±SEM). ### P<0.001 vs N group;** P<0.01and *** P<0.001 vs M group; ΔΔΔ P<0.001 vs MD group; & P<0.05 vs MB group. 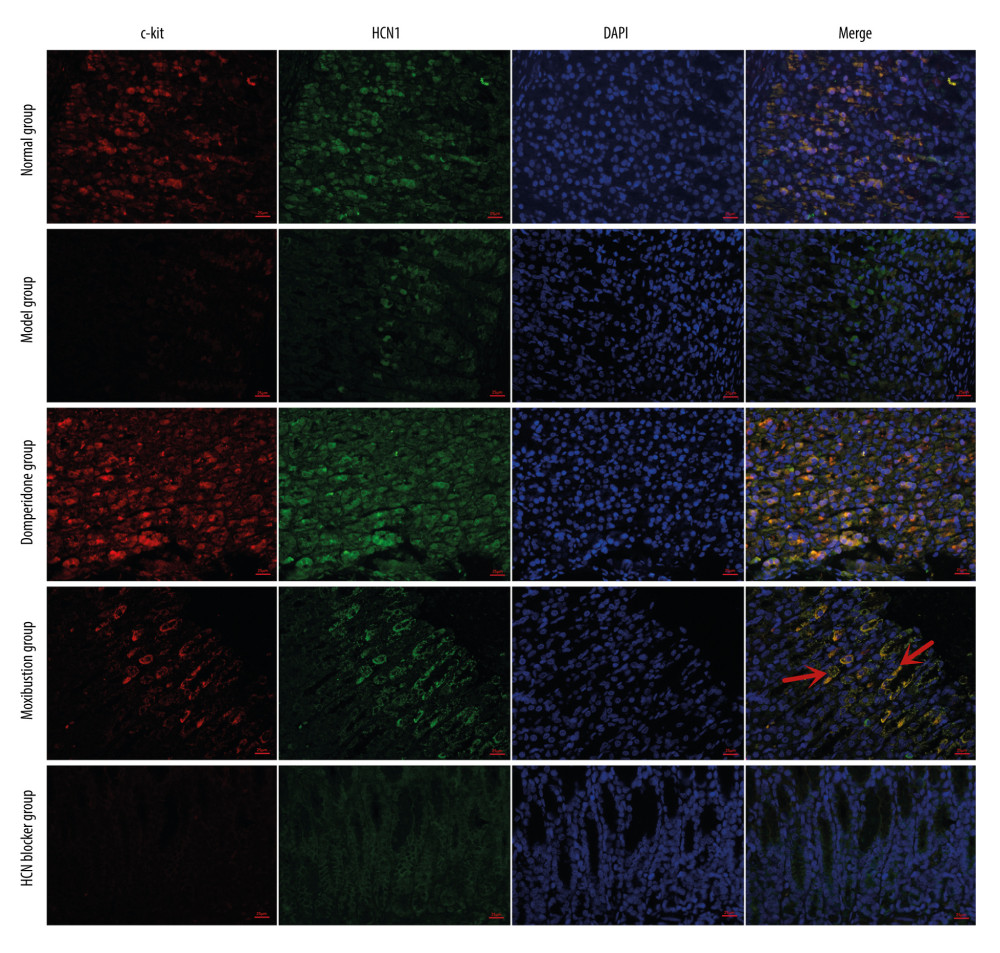 Figure 3. Double immunofluorescence staining of c-kit and HCN1 in gastric tissues. Red, c-kit; Green, HCN1; Blue, DAPI.
Figure 3. Double immunofluorescence staining of c-kit and HCN1 in gastric tissues. Red, c-kit; Green, HCN1; Blue, DAPI. 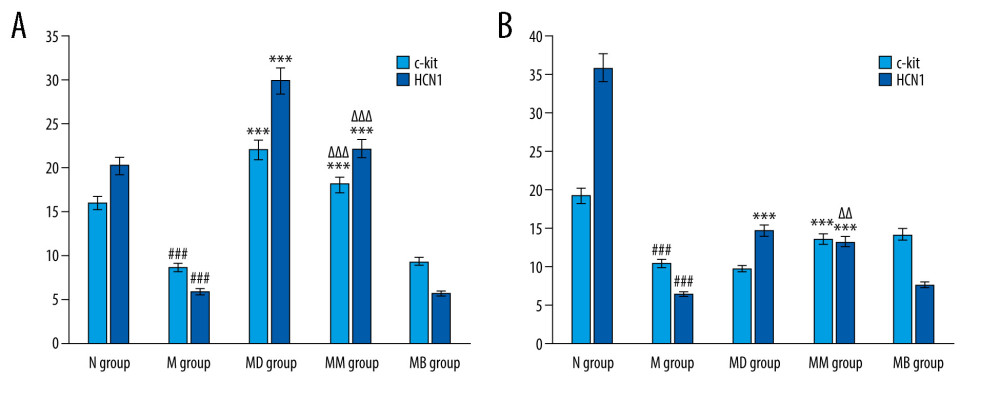 Figure 4. (A) Quantitative analysis of c-kit and HCN1 fluorescence luminance in gastric antrum of FD rats (n=3/group). (mean±SEM). (B) Quantitative analysis of c-kit and HCN1 fluorescence luminance in small intestine of rats (n=3/group). (mean±SEM). ### P<0.001 vs N group; *** P<0.001 vs M group; ΔΔ P<0.01 vs MD group; ΔΔΔ P<0.001 vs MD group.
Figure 4. (A) Quantitative analysis of c-kit and HCN1 fluorescence luminance in gastric antrum of FD rats (n=3/group). (mean±SEM). (B) Quantitative analysis of c-kit and HCN1 fluorescence luminance in small intestine of rats (n=3/group). (mean±SEM). ### P<0.001 vs N group; *** P<0.001 vs M group; ΔΔ P<0.01 vs MD group; ΔΔΔ P<0.001 vs MD group. 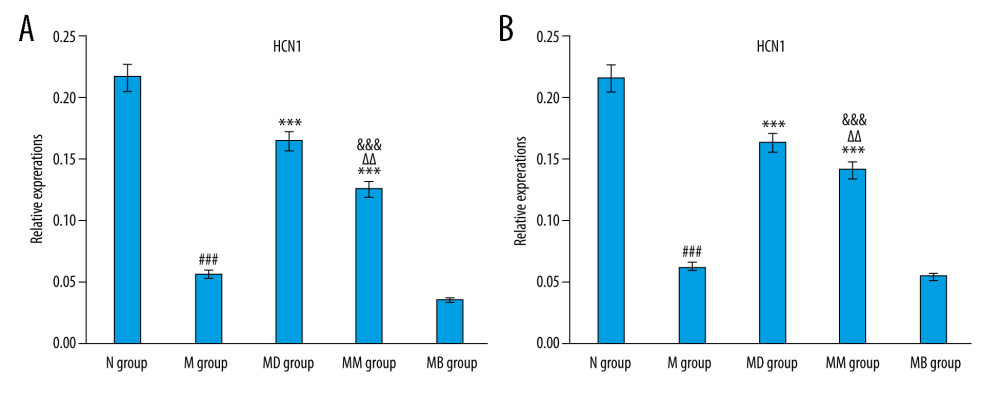 Figure 5. (A) HCN1 expression in the upper segments of small intestine (RT-PCR) of rats (n=4/group) (mean±SEM). (B) HCN1 expression in the satiety center of the hypothalamus of rats (n=4/group) (mean±SEM). ### P<0.001 vs N group; *** P<0.001 vs M group; ΔΔ P<0.01 vs MD group; &&& P<0.001 vs MB group.
Figure 5. (A) HCN1 expression in the upper segments of small intestine (RT-PCR) of rats (n=4/group) (mean±SEM). (B) HCN1 expression in the satiety center of the hypothalamus of rats (n=4/group) (mean±SEM). ### P<0.001 vs N group; *** P<0.001 vs M group; ΔΔ P<0.01 vs MD group; &&& P<0.001 vs MB group. 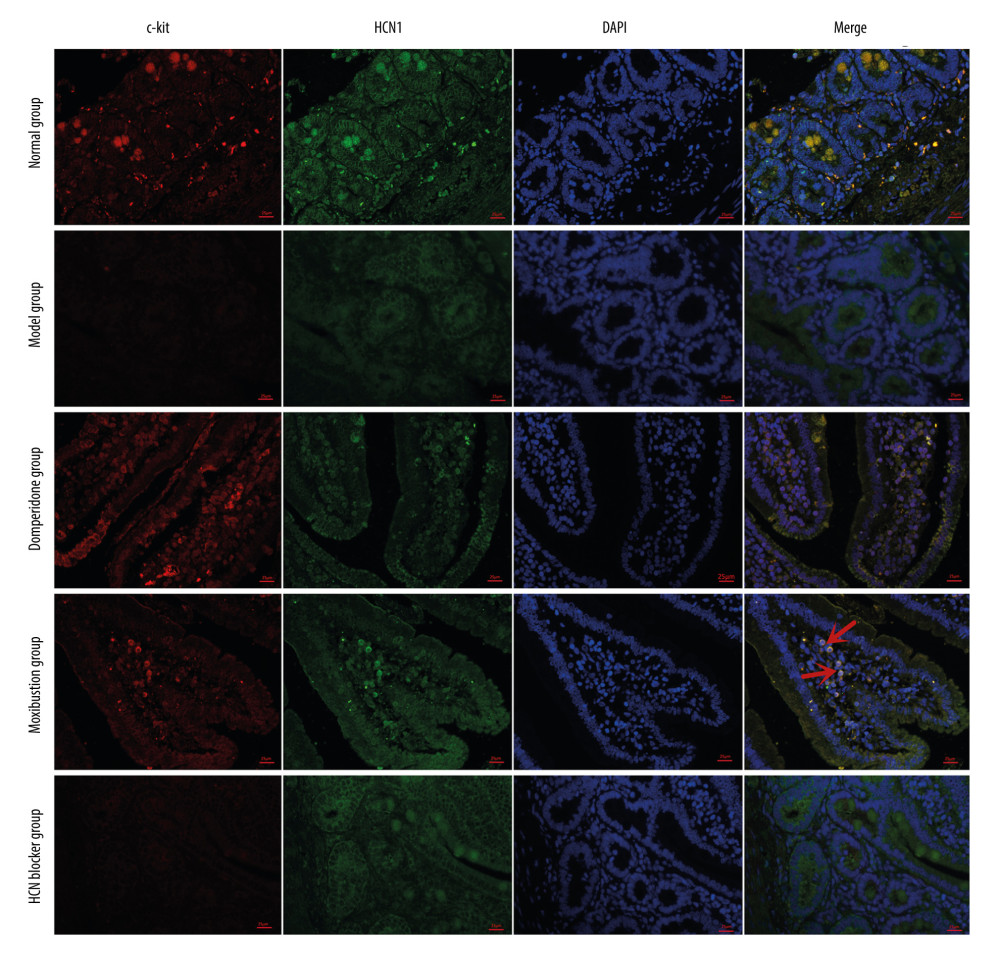 Figure 6. Double immunofluorescence staining of c-kit and HCN1 in upper small intestinal tissues. Red, c-kit; Green, HCN1; Blue, DAPI.
Figure 6. Double immunofluorescence staining of c-kit and HCN1 in upper small intestinal tissues. Red, c-kit; Green, HCN1; Blue, DAPI. 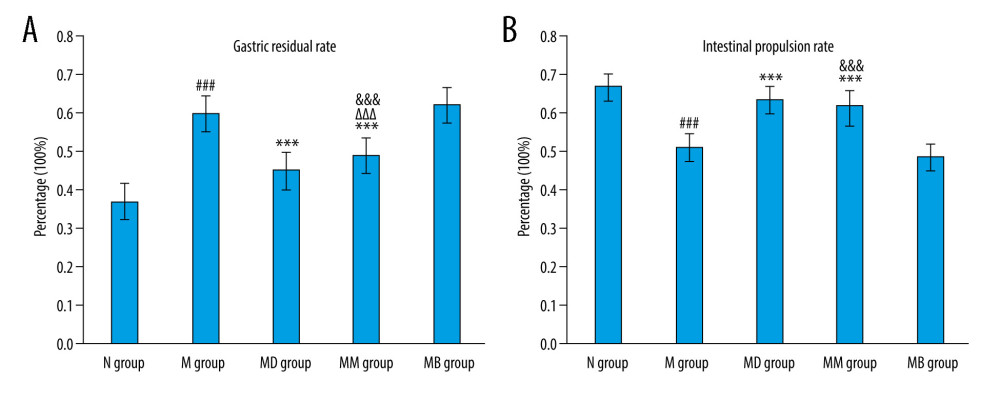 Figure 7. GRR (A) and IPR (B) of rats (n=10/group) (mean±SEM). ### P<0.001 vs N group; *** P<0.001 vs M group; ΔΔΔ P<0.001 vs MD group; &&& P<0.001 vs MB group.
Figure 7. GRR (A) and IPR (B) of rats (n=10/group) (mean±SEM). ### P<0.001 vs N group; *** P<0.001 vs M group; ΔΔΔ P<0.001 vs MD group; &&& P<0.001 vs MB group. References
1. Ford AC, Mahadeva S, Carbone MF, Functional dyspepsia: Lancet, 2020; 396; 1689-702
2. Black CJ, Drossman DA, Talley NJ, Functional gastrointestinal disorders: Advances in understanding and management: Lancet, 2020; 396; 1664-74
3. Stanghellini V, Chan FK, Hasler WL, Gastroduodenal disorders: Gastroenterology, 2016; 150; 1380-92
4. Talley NJ, Ford AC, Functional dyspepsia: N Engl J Med, 2016; 374; 896
5. Mani J, Madani S, Thomas R, Economic impact and prognostic factors of functional dyspepsia in children: J Pediatr Gastroenterol Nutr, 2020; 70; e65-70
6. Talley NJ, What causes functional gastrointestinal disorders? A proposed disease model: Am J Gastroenterol, 2020; 115; 41-48
7. Wauters L, Talley NJ, Walker MM, Novel concepts in the pathophysiology and treatment of functional dyspepsia: Gut, 2020; 69; 591-600
8. Ford AC, Moayyedi P, Black CJ, Systematic review and network meta-analysis: Efficacy of drugs for functional dyspepsia: Aliment Pharmacol Ther, 2021; 53; 8-21
9. Pasricha PJ, Grover M, Yates KP, Functional dyspepsia and gastroparesis in tertiary care are interchangeable syndromes with common clinical and pathologic features: Gastroenterology, 2021; 160; 2006-17
10. Wang C, Fang X, Inflammation and overlap of irritable bowel syndrome and functional dyspepsia: J Neurogastroenterol Motil, 2021; 27; 153-64
11. Rahman MM, Ghoshal UC, Kibria MG, Functional dyspepsia, peptic ulcer, and helicobacter pylori infection in a rural community of South Asia: An endoscopy-assisted household survey: Clin Transl Gastroenterol, 2021; 12; e00334
12. Wauters L, Ceulemans M, Frings D, Proton pump inhibitors reduce duodenal eosinophilia, mast cells, and permeability in patients with functional dyspepsia: Gastroenterology, 2021; 160; 1521-31e9
13. Kao KL, Sung FC, Huang HC, Functional dyspepsia in depression: A population-based cohort study: Eur J Clin Invest, 2021; 51; e13506
14. Cordner ZA, Li Q, Liu L, Vagal gut-brain signaling mediates amygdaloid plasticity, affect, and pain in a functional dyspepsia model: JCI Insight, 2021; 6; e144046
15. Duncanson K, Burns G, Pryor J, Mechanisms of food-induced symptom induction and dietary management in functional dyspepsia: Nutrients, 2021; 13; 1109
16. Nakamura F, Kuribayashi S, Tanaka F, Impact of improvement of sleep disturbance on symptoms and quality of life in patients with functional dyspepsia: BMC Gastroenterol, 2021; 21; 78
17. Beh KH, Chuah KH, Rappek N, Mahadeva S, The association of body mass index with functional dyspepsia is independent of psychological morbidity: A cross-sectional study: PLoS One, 2021; 16; e0245511
18. Varghese C, Carson DA, Bhat S, Clinical associations of functional dyspepsia with gastric dysrhythmia on electrogastrography: A comprehensive systematic review and meta-analysis: Neurogastroenterol Motil, 2021 [Online ahead of print]
19. Agrusa AS, Allegra AB, Kunkel DC, Coleman TP, Robust methods to detect abnormal initiation in the gastric slow wave from cutaneous recordings: Annu Int Conf IEEE Eng Med Biol Soc, 2020; 2020; 225-31
20. Benzoni P, Bertoli G, Giannetti F, The funny current: Even funnier than 40 years ago. Uncanonical expression and roles of HCN/f channels all over the body: Prog Biophys Mol Biol, 2021 [Online ahead of print]
21. Shahi PK, Choi S, Zuo DC, The possible roles of hyperpolarization-activated cyclic nucleotide channels in regulating pacemaker activity in colonic interstitial cells of Cajal: J Gastroenterol, 2014; 49; 1001-10
22. Si X, Huang L, Gong Y, Role of calcium in activation of hyperpolarization-activated cyclic nucleotide-gated channels caused by cholecystokinin octapeptide in interstitial cells of cajal: Digestion, 2012; 85; 266-75
23. Wang SZFourth Military Medical University, Effect of HCN1 on the pace generation of the gastrointestinal tract: Surgery, 2009(12)
24. Chun X, Chao Z, Ming QDistribution and characteristics of HCN1 in gastrointestinal tract: Journal of Shanxi Medical University, 2012; 43; 564-66 [in Chinese]
25. Zhong W, Darmani NA: Front Pharmacol, 2021; 12; 647021
26. Schlaeger JM, Stoffel CL, Bussell JL, Moxibustion for cephalic version of breech presentation: J Midwifery Womens Health, 2018; 63; 309-22
27. Stein DJ, Massage acupuncture, moxibustion, and other forms of complementary and alternative medicine in inflammatory bowel disease: Gastroenterol Clin North Am, 2017; 46; 875-80
28. Choe S, Cai M, Jerng UM, Lee JH, The efficacy and underlying mechanism of moxibustion in preventing cognitive impairment: A systematic review of animal studies: Exp Neurobiol, 2018; 27; 1-15
29. He QD, Huang MS, Zhang LB, Effect of moxibustion on intestinal microbiome in acute gastric ulcer rats: Evid Based Complement Alternat Med, 2019; 2019; 6184205
30. Qi Q, Liu YN, Jin XM, Moxibustion treatment modulates the gut microbiota and immune function in a dextran sulphate sodium-induced colitis rat model: World J Gastroenterol, 2018; 24; 3130-44
31. Tabosa A, Yamamura Y, Forno ER, Mello LE, A comparative study of the effects of electroacupuncture and moxibustion in the gastrointestinal motility of the rat: Dig Dis Sci, 2004; 49; 602-10
32. Wei D, Zhao N, Xie L, Electroacupuncture and moxibustion improved anxiety behavior in DSS-induced colitis mice: Gastroenterol Res Pract, 2019; 2019; 2345890
33. Yang X, Wang W, Zhang Y, Moxibustion improves ovary function by suppressing apoptosis events and upregulating antioxidant defenses in natural aging ovary: Life Sci, 2019; 229; 166-72
34. Ho R, Chung V, Wong C, Acupuncture and related therapies used as add-on or alternative to prokinetics for functional dyspepsia: Overview of systematic reviews and network meta-analysis: Sci Rep, 2017; 7; 10320
35. Zhang J, Liu Y, Huang X, Efficacy comparison of different acupuncture treatments for functional dyspepsia: A systematic review with network meta-analysis: Evid Based Complement Alternat Med, 2020; 2020; 3872919
36. Ye Y, Wang XR, Zheng Y, Choosing an animal model for the study of functional dyspepsia: Can J Gastroenterol Hepatol, 2018; 2018; 1531958
37. Zhang XX, Min XC, Xu XL, ZD7288, a selective hyperpolarization-activated cyclic nucleotide-gated channel blocker, inhibits hippocampal synaptic plasticity: Neural Regen Res, 2016; 11; 779-86
38. Su YS, Xin JJ, Yang ZK, Effects of different local moxibustion-like stimuli at Zusanli (ST36) and Zhongwan (CV12) on gastric motility and its underlying receptor mechanism: Evid Based Complement Alternat Med, 2015; 2015; 486963
39. Koloski N, Holtmann G, Talley NJ, Is there a causal link between psychological disorders and functional gastrointestinal disorders: Expert Rev Gastroenterol Hepatol, 2020; 14; 1047-59
40. Lee CH, MacKinnon R, Voltage sensor movements during hyperpolarization in the HCN channel: Cell, 2019; 179; 1582-9e7
41. Wang ZJ, Blanco I, Hayoz S, Brelidze TI, The HCN domain is required for HCN channel cell-surface expression and couples voltage- and cAMP-dependent gating mechanisms: J Biol Chem, 2020; 295; 8164-73
42. Brandalise F, Kalmbach BE, Mehta P, Fragile X mental retardation protein bidirectionally controls dendritic ih in a cell type-specific manner between mouse hippocampus and prefrontal cortex: J Neurosci, 2020; 40; 5327-40
43. Kharouf Q, Phillips AM, Bleakley LE, The hyperpolarization-activated cyclic nucleotide-gated 4 channel as a potential anti-seizure drug target: Br J Pharmacol, 2020; 177; 3712-29
44. Sciamanna G, Ponterio G, Vanni V, Optogenetic activation of striatopallidal neurons reveals altered HCN gating in DYT1 dystonia: Cell Rep, 2020; 31; 107644
45. Yang L, Liu X, Yao K, HCN channel antagonist ZD7288 ameliorates neuropathic pain and associated depression: Brain Res, 2019; 1717; 204-13
46. Yuan L, Luo L, Ma X, Chronic morphine induces cyclic adenosine monophosphate formation and hyperpolarization-activated cyclic nucleotide-gated channel expression in the spinal cord of mice: Neuropharmacology, 2020; 176; 108222
47. Rivolta I, Binda A, Masi A, DiFrancesco JC, Cardiac and neuronal HCN channelopathies: Pflugers Arch, 2020; 472; 931-51
48. Liu Q, Long Z, Dong X, Cyclophosphamide-induced HCN1 channel upregulation in interstitial Cajal-like cells leads to bladder hyperactivity in mice: Exp Mol Med, 2017; 49; e319
49. Xu J, Lin X, Cheng KK, Metabolic response in rats following electroacupuncture or moxibustion stimulation: Evid Based Complement Alternat Med, 2019; 2019; 6947471
50. Akhunzada HA, Rehman H, Tariq N, Enteric fever: Diagnostic dilemma encountered in domperidone-induced neuroleptic malignant syndrome: Cureus, 2021; 13; e15385
Figures
 Figure 1. The weight gain (A) and food intake (B) of rats (n=10/group) (mean±SEM). ### P<0.001 vs N group; ** P<0.001 vs M group; Δ P<0.05, ΔΔ P<0.01 and ΔΔΔ P<0.001 vs MD; &&& P<0.001 vs MB group.
Figure 1. The weight gain (A) and food intake (B) of rats (n=10/group) (mean±SEM). ### P<0.001 vs N group; ** P<0.001 vs M group; Δ P<0.05, ΔΔ P<0.01 and ΔΔΔ P<0.001 vs MD; &&& P<0.001 vs MB group. Figure 2. HCN1 expression in the gastric antrum tissues of rats by western blotting (n=4/group). (mean±SEM). ### P<0.001 vs N group;** P<0.01and *** P<0.001 vs M group; ΔΔΔ P<0.001 vs MD group; & P<0.05 vs MB group.
Figure 2. HCN1 expression in the gastric antrum tissues of rats by western blotting (n=4/group). (mean±SEM). ### P<0.001 vs N group;** P<0.01and *** P<0.001 vs M group; ΔΔΔ P<0.001 vs MD group; & P<0.05 vs MB group. Figure 3. Double immunofluorescence staining of c-kit and HCN1 in gastric tissues. Red, c-kit; Green, HCN1; Blue, DAPI.
Figure 3. Double immunofluorescence staining of c-kit and HCN1 in gastric tissues. Red, c-kit; Green, HCN1; Blue, DAPI. Figure 4. (A) Quantitative analysis of c-kit and HCN1 fluorescence luminance in gastric antrum of FD rats (n=3/group). (mean±SEM). (B) Quantitative analysis of c-kit and HCN1 fluorescence luminance in small intestine of rats (n=3/group). (mean±SEM). ### P<0.001 vs N group; *** P<0.001 vs M group; ΔΔ P<0.01 vs MD group; ΔΔΔ P<0.001 vs MD group.
Figure 4. (A) Quantitative analysis of c-kit and HCN1 fluorescence luminance in gastric antrum of FD rats (n=3/group). (mean±SEM). (B) Quantitative analysis of c-kit and HCN1 fluorescence luminance in small intestine of rats (n=3/group). (mean±SEM). ### P<0.001 vs N group; *** P<0.001 vs M group; ΔΔ P<0.01 vs MD group; ΔΔΔ P<0.001 vs MD group. Figure 5. (A) HCN1 expression in the upper segments of small intestine (RT-PCR) of rats (n=4/group) (mean±SEM). (B) HCN1 expression in the satiety center of the hypothalamus of rats (n=4/group) (mean±SEM). ### P<0.001 vs N group; *** P<0.001 vs M group; ΔΔ P<0.01 vs MD group; &&& P<0.001 vs MB group.
Figure 5. (A) HCN1 expression in the upper segments of small intestine (RT-PCR) of rats (n=4/group) (mean±SEM). (B) HCN1 expression in the satiety center of the hypothalamus of rats (n=4/group) (mean±SEM). ### P<0.001 vs N group; *** P<0.001 vs M group; ΔΔ P<0.01 vs MD group; &&& P<0.001 vs MB group. Figure 6. Double immunofluorescence staining of c-kit and HCN1 in upper small intestinal tissues. Red, c-kit; Green, HCN1; Blue, DAPI.
Figure 6. Double immunofluorescence staining of c-kit and HCN1 in upper small intestinal tissues. Red, c-kit; Green, HCN1; Blue, DAPI. Figure 7. GRR (A) and IPR (B) of rats (n=10/group) (mean±SEM). ### P<0.001 vs N group; *** P<0.001 vs M group; ΔΔΔ P<0.001 vs MD group; &&& P<0.001 vs MB group.
Figure 7. GRR (A) and IPR (B) of rats (n=10/group) (mean±SEM). ### P<0.001 vs N group; *** P<0.001 vs M group; ΔΔΔ P<0.001 vs MD group; &&& P<0.001 vs MB group. In Press
15 Apr 2024 : Laboratory Research
The Role of Copper-Induced M2 Macrophage Polarization in Protecting Cartilage Matrix in OsteoarthritisMed Sci Monit In Press; DOI: 10.12659/MSM.943738
07 Mar 2024 : Clinical Research
Knowledge of and Attitudes Toward Clinical Trials: A Questionnaire-Based Study of 179 Male Third- and Fourt...Med Sci Monit In Press; DOI: 10.12659/MSM.943468
08 Mar 2024 : Animal Research
Modification of Experimental Model of Necrotizing Enterocolitis (NEC) in Rat Pups by Single Exposure to Hyp...Med Sci Monit In Press; DOI: 10.12659/MSM.943443
18 Apr 2024 : Clinical Research
Comparative Analysis of Open and Closed Sphincterotomy for the Treatment of Chronic Anal Fissure: Safety an...Med Sci Monit In Press; DOI: 10.12659/MSM.944127
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952








