11 June 2022: Clinical Research
Efficacy of Focused Extracorporeal Shock Wave Therapy in Chronic Low Back Pain: A Prospective Randomized 3-Month Follow-Up Study
Katarzyna Rajfur1ABDEF, Joanna Rajfur1ABDEF, Tomasz Matusz1ABF, Karolina Walewicz1ABD, Robert Dymarek2ABDEFG*, Kuba PtaszkowskiDOI: 10.12659/MSM.936614
Med Sci Monit 2022; 28:e936614
Abstract
BACKGROUND: Extracorporeal shock wave therapy (ESWT) is a modern physiotherapeutic method that is useful for treating musculoskeletal conditions. There are still limited data from well-designed studies evaluating the clinical efficiency of ESWT in low back pain (LBP). Therefore, this study aimed to assess the effectiveness of the focused ESWT (fESWT) in reducing pain and improving the functional status of patients with chronic LBP.
MATERIAL AND METHODS: The study involved 40 patients with L5-S1 discopathy with chronic LBP pain who were randomized into 2 groups: group A (n=20, mean age of 42.3±13.1 years) and group B (n=20, mean age of 45.4±14 years). Group A was an experimental group treated with an fESWT at the lumbar and sacral spine (0.15 mJ/mm², 1000 pulses, 4 Hz). Group B was a control group, treated with a sham fESWT. The treatment protocol in both groups included identical stabilization training (45 minutes, once a day, 5 days a week). Study outcomes included subjective pain with a visual analog scale (VAS) and Laitinen Pain Scale (LPS), and functional status using the Oswestry Disability Index (ODI). Measurements were made before and after treatments, as well as follow-up observations at 1 and 3 months following ESWT. The study was prospectively registered at the ISRCTN registry platform (no. ISRCTN13785224).
RESULTS: There was a significant analgesic effect (VAS and LPS) in both groups; however, it was significantly greater in the experimental group compared to the sham group (P<0.05). A more significant decrease in the perceived pain (VAS and LPS) was observed immediately after the active fESWT therapy. In follow-up observations (after 1 and 3 months), there were no significant between-group differences (P>0.05). Also, there was a significant effect in terms of functional state (ODI) for both groups (P<0.05); however, between-group comparisons revealed no statistically significant differences (P>0.05).
CONCLUSIONS: Focused ESWT with an exercise program can be effective in patients with chronic LBP. ESWT allows reducing pain, although it does not seem to significantly improve a patient’s functional state.
Keywords: chronic pain, Extracorporeal Shockwave Therapy, functional status, Low Back Pain, Physical Therapy Modalities, Randomized controlled trial, Adult, Follow-Up Studies, Humans, Lipopolysaccharides, Middle Aged, Prospective Studies, Treatment Outcome
Background
Extracorporeal shock wave (ESWT) is a modern physiotherapeutic method which is useful for musculoskeletal conditions. Despite some evidence from recent systematic reviews, meta-analyses [1–4], and the Cochrane recommendations [5], there are still inconclusive results on ESWT. Moreover, the literature on ESWT in low back pain (LBP) treatment in the Web of Science Core Collection, PubMed, and MEDLINE databases is limited. There are only 6 randomized clinical trials (RCTs) showing the effect of ESWT on LBP [6–11] that went through methodological quality analysis using the Physiotherapy Evidence Database (PEDro) score (Table 1). Based on objective data, levels of methodological quality of these randomized clinical trials vary from medium to low. Furthermore, most studies did not meet the essential criteria of Evidence-Based Physiotherapy (no Cochrane recommendation and PEDro indexation), suggesting that this topic still requires in-depth investigation. Therefore, in practice, it is not easy to objectively analyze the clinical effectiveness of such procedures, together with precise recommendations regarding doses, treatment parameters, duration of the procedure, and other relevant aspects of the treatment protocol. For example, it is unclear how to evaluate radial vs focused techniques.
The radial method (rESWT) is based on pneumatic technology, using the principle of accelerated cartridge impact by compressed air under high pressure. In this way, the shock wave penetrates the body with a radiated beam, and its energy decreases with the depth of penetration. The pulse lasts a maximum of 5 ms, and the pressure reached by the wave does not exceed 1 MPa [12]. The focused technique (fESWT) is characterized by a stronger stimulus, having a more intense effect on the tissues. Unlike the radial method, the focused technique uses electroacoustic technology. Under the influence of high voltage, an acoustic shock wave is created in the applicator, forming a focused stimulus using a special lens. This stimulus with special coupling attachments is introduced into the patient’s body at an appropriate depth, at the assumed pressure of up to 100 MPa, and the pulse duration up to 0.2 μs [13,14].
In 2020, our research team published clinical data on radial ESWT in treating patients with chronic LBP [15] that had the methodologically highest level (9/10 points) according to PEDro score. Our results showed that the ESWT technique might be especially used in maintaining remission of symptoms and preventing recurrence of disease. Therefore, our team has decided to examine an fESWT, which theoretically might have greater technological possibilities than the radial technique. Thus, the study aimed to assess the effectiveness of focused ESWT in reducing pain intensity and improving functional efficiency in patients with chronic LBP.
Material and Methods
STUDY DESIGN:
The research was carried out in the Clinical Research Laboratory of the Institute of Health Sciences of the University of Opole. The study was conducted in cooperation with the Department of Physiotherapy of the Wrocław Medical University in Poland. The local and independent Bioethics Committee of the University of Opole approved the study protocol (no. KB/90/FI/2018). The study was prospectively registered at the International Standard Randomized Controlled Trial Number (ISRCTN) registry database (no. ISRCTN13785224). Each participant provided their written informed consent prior to the study. The studies were conducted in accordance with the Helsinki Declaration and Good Clinical Practice guidelines.
RANDOMIZATION AND BLINDING:
Patients were selected for this randomized and single-blinded project by an internist, radiologist, neurologist, neurosurgeon, orthopedist, and physiotherapist. After a positive qualifying procedure, participants were randomly assigned to real or sham ESWT treatments using a computer random number generator (
PARTICIPANTS:
Patients with L5-S1 discopathy, chronic pain, and no spinal surgical intervention were qualified. The participants were of legal age and had current magnetic resonance imaging (MRI) scans confirming the LBP syndrome – type 3 changes in section L5-S1 according to Modic classification (MC), which describes vertebral endplate lesions.
The exclusion criteria were: discopathy beyond the L5-S1 (MC type 1 and 2), no pain and reduced mobility in the lumbosacral segment, other spinal conditions (fractures, tumors, spondylolisthesis, rheumatic diseases, cauda equina syndrome), pregnancy or ovulation, neurological deficits, implanted cardiac pacemaker, blood coagulation disorders, metal implants within the application site, sensory disturbances, mental disorders, cancer, skin lesions within the treatment site, viral and bacterial infections, painkillers, and anti-inflammatory drugs.
The study involved 40 patients with L5-S1 discopathy of the spine with chronic pain lasting at least 12 weeks. Patients were randomized into 2 groups: group A (n=20) with a mean age of 42.3±13.1 years and group B (n=20) with a mean age of 45.4±14 years. The groups were homogeneous regarding demographic characteristics (Table 2) and initial pain and functional status assessments. Following the Consolidated Standards of Reporting Trials (CONSORT) guidelines for registered randomized clinical trials, the patient flow over the entire period of the study is shown in Figure 1. In both groups, all participants completed treatment. All patients were assessed 1 month later and 3 months after the end of the study. It should be noted that 1 person in group A (business trip at the time of taking the measurements) and 2 people in group B (taking painkillers) were excluded from the statistical analysis.
TREATMENT:
Group A was an experimental group treated with an fESWT shockwave using the Duolith SD1 Tower device (Storz Medical, Switzerland; Figures 2, 3). Each procedure was performed using the contact method at the lumbar and sacral spine level in the area of greatest pain indicated by the patient (Figure 4). The following parameters were used for the therapy: energy flux density 0.15 mJ/mm2 (1000 pulses), frequency 4 Hz. An ultrasound gel was used as a coupling substance between the applicator and the patient’s skin to reduce tissue resistance. Treatments were performed twice a week (Monday and Thursday) for 5 weeks (10 treatments in total). The therapy was conducted under ultrasound guidance.
Group B was a control group, treated with a sham fESWT. Stimulation took place using a special polyethylene insert mounted on the top of the applicator, which absorbed energy and limited its spread in the tissue. The treatment procedure was identical to condition A in terms of the audible signals and the technical parameters used in the actual procedure.
The treatment protocol in both groups included identical stabilization training (45 minutes, once a day, 5 days a week, Monday to Friday) with myofascial relaxation of the extensors of the spine, activation of the lumbo-sacro-pelvic complex and deep muscles, stimulation of proper breathing, and dynamic postural exercises.
MEASUREMENT:
Therapeutic progress was assessed by analyzing subjective pain sensations using a visual analog scale (VAS), on which the patient-rated the symptoms on a numerical scale from 0 to 10 (0 indicated no pain, 10 indicated the strongest pain).
The Laitinen Pain Scale (LPS) was also used, which measures 4 criteria of pain: its intensity, frequency of its occurrence, use of painkillers, and limitation of motor activity. Patients assigned points from 0 to 4 (0 – no pain, 4 – severe pain) to each of the determined indicators.
Functional fitness was assessed using the Oswestry Disability Index (ODI), which consists of 10 sections, with 8 related to activities of daily living and 2 related to pain concerns; responses are graded from 0 to 5, and the total ODI score is presented on a scoring system of 0–50 or a percentage system of 0–100% indicating the degree of disability.
Tests and questionnaires were administered in both groups at the beginning, after treatment, and during follow-up visits after 1 and 3 months. During this time, the patients were not receiving any other treatment.
SAMPLE SIZE:
The sample size was based on group differences in primary outcomes (means and standard deviations of pain experience), estimated at 26 participants (13 in each group). A 20% loss to follow-up was allowed for in calculations. The decreasing sample size also applied to historical information from our unit because 45% of patients offered conservative management (physical therapy agents) for LBP opted for ESWT within 6 months.
STATISTICAL ANALYSIS:
Statistical analysis was performed using the Statistica 13 program (TIBCO, Inc., USA). Arithmetic means, medians, standard deviations, quartiles, and the range of variability (extreme values) were calculated for measurable variables. For qualitative variables, the frequencies were calculated (the results were given as percentages). Quantitative variables were subjected to the Shapiro-Wilk test to determine the normality of distribution. Comparisons between groups were made using the chi-square test (χ2). Within-group comparisons for measurement conditions 1, 2, 3, and 4 were performed by Friedman’s analysis of variance and a post hoc test (Dunn’s test). Finally, the comparison between the experimental and placebo groups was assessed using the Mann-Whitney U test. The level for statistical significance was α=0.05.
Results
Table 3 presents comparisons of pain (VAS) in both groups. There was a significant effect in both groups (
Comparing pain between the groups (using the VAS scale showed differences immediately after treatment and 1 month after the end of treatment (Figure 5). For the ESWT group, there was a significantly greater improvement in VAS scores compared to the sham group (
Table 4 shows the comparisons of perceived pain according to LPS in 4 measurements between the experimental and control groups. The mean pain scores changed significantly in both groups (main effect:
Patients from the experimental group differed from the control group immediately after treatment, indicating remission of pain (
Table 5 shows the between-group comparisons of functional assessments taken with the ODI under 4 measurement conditions. There was a significant effect for both groups (significant effect:
Discussion
STUDY LIMITATIONS:
Future research should use other objective measurement methods (eg, stabilometric platform, surface electromyography) and include more participants over a longer period. Also, it is important to establish uniform treatment parameters that can be verified by other researchers. In subsequent studies, the questionnaire assessment of disability should be extended.
Conclusions
Focused ESWT in conjunction with an exercise program can be effective in patients with chronic LBP, both short- and long-term. In addition, focused ESWT allows reducing pain, although it does not seem to improve a patient’s functional state significantly. Thus, ESWT cannot be a key enrichment method for a standard rehabilitation program at this stage. Therefore, further clinical trials should be conducted, especially regarding patient functional evaluation after applying focused ESWT.
Figures
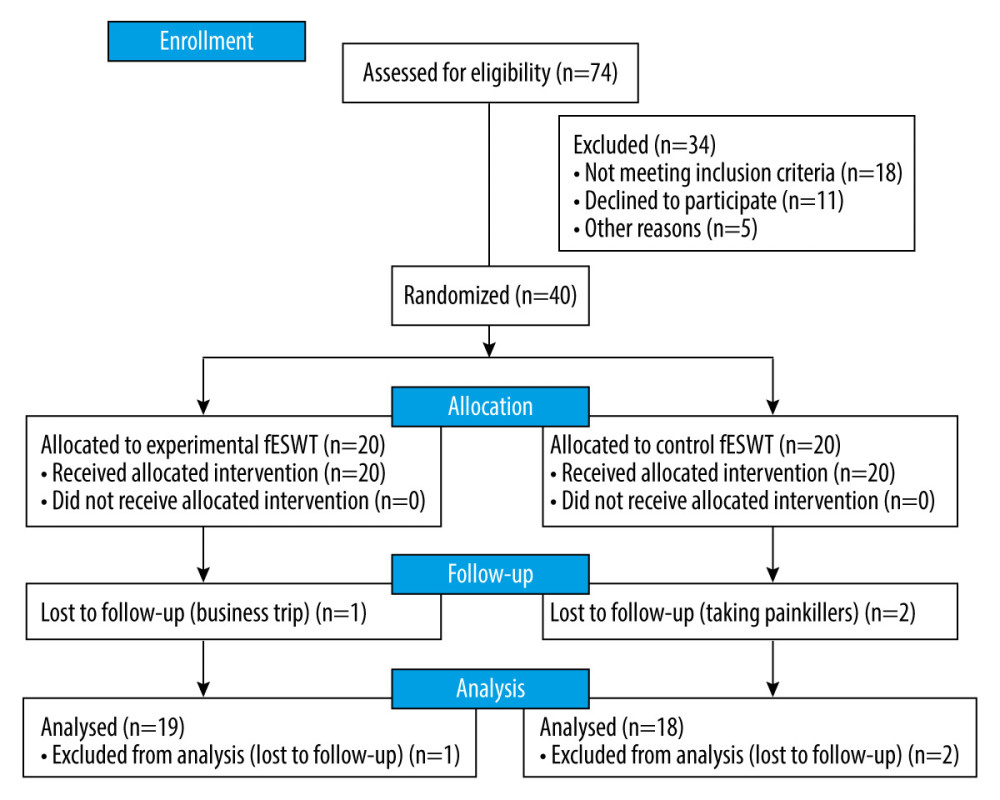 Figure 1. CONSORT flow chart of study participants. fESWT – focused extracorporeal shock wave.
Figure 1. CONSORT flow chart of study participants. fESWT – focused extracorporeal shock wave.  Figure 2. Duolith SD1 Tower device for high-energy fESWT.
Figure 2. Duolith SD1 Tower device for high-energy fESWT.  Figure 3. fESWT applicator used in this study.
Figure 3. fESWT applicator used in this study.  Figure 4. Treatment session using the fESWT applicator.
Figure 4. Treatment session using the fESWT applicator. 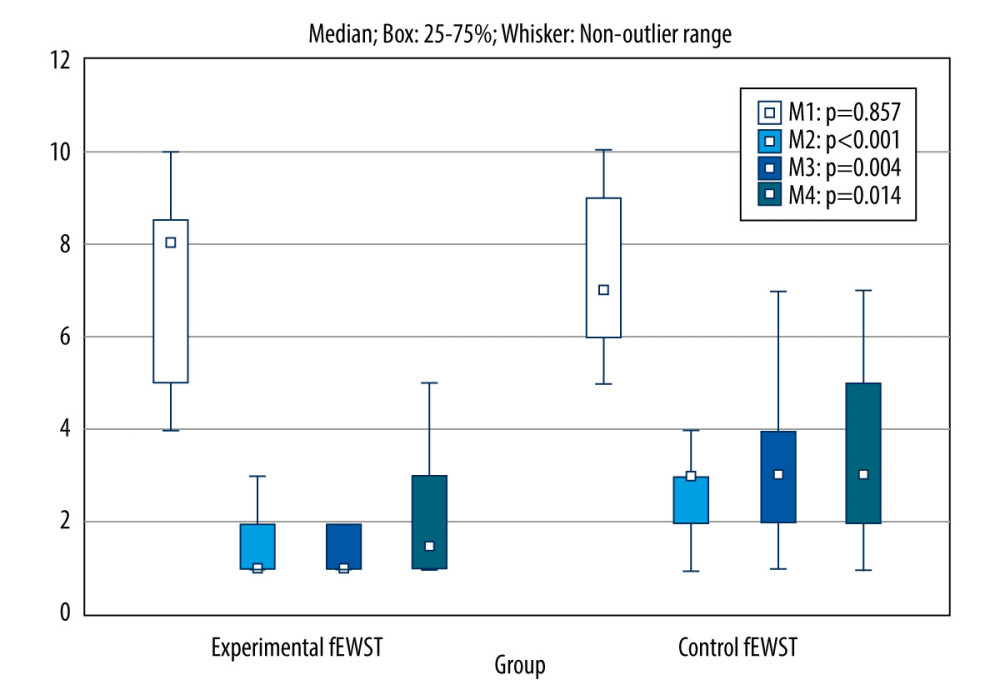 Figure 5. Comparison of VAS scores obtained in 4 measurements between the experimental and control group. fESWT – focused extracorporeal shock wave; M1 – before, M2 – after, M3 – after 1 month, M4 – after 3 months.
Figure 5. Comparison of VAS scores obtained in 4 measurements between the experimental and control group. fESWT – focused extracorporeal shock wave; M1 – before, M2 – after, M3 – after 1 month, M4 – after 3 months. 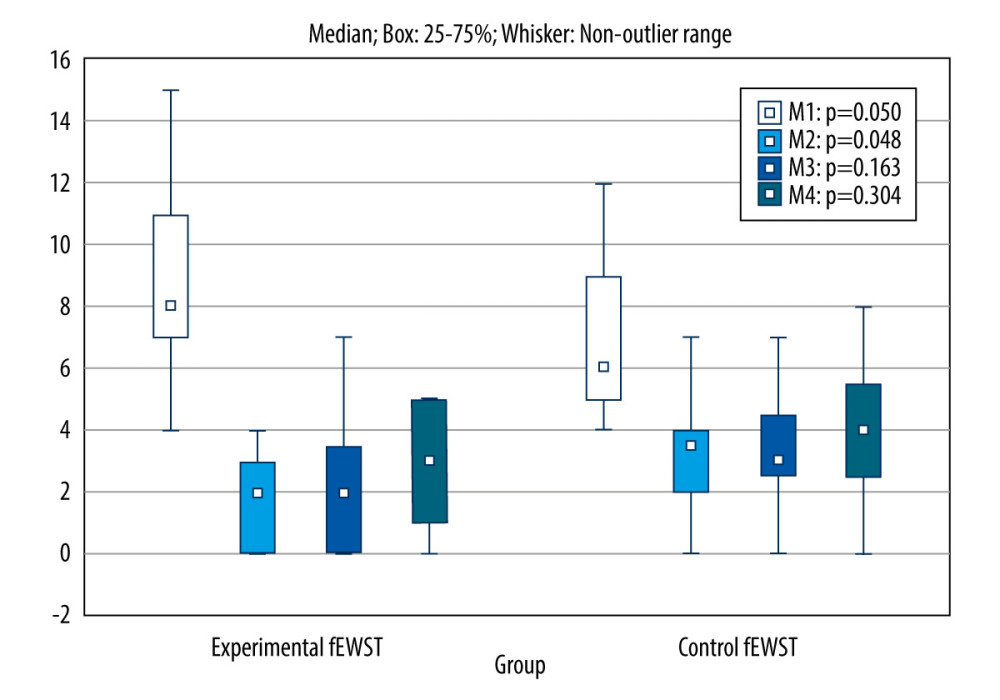 Figure 6. Comparison of LPS scores obtained in 4 measurements between the experimental and control group. fESWT – focused extracorporeal shock wave; M1 – before, M2 – after, M3 – after 1 month, M4 – after 3 months.
Figure 6. Comparison of LPS scores obtained in 4 measurements between the experimental and control group. fESWT – focused extracorporeal shock wave; M1 – before, M2 – after, M3 – after 1 month, M4 – after 3 months. 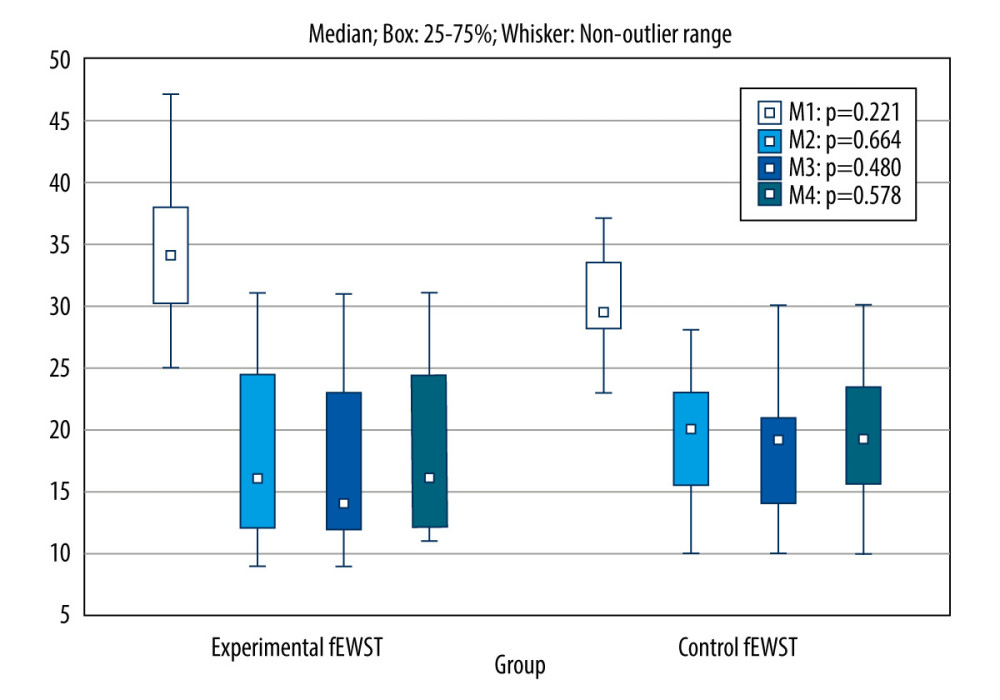 Figure 7. Comparison of ODI scores obtained in 4 measurements between the experimental and control group. fESWT – focused extracorporeal shock wave; M1 – before, M2 – after, M3 – after 1 month, M4 – after 3 months.
Figure 7. Comparison of ODI scores obtained in 4 measurements between the experimental and control group. fESWT – focused extracorporeal shock wave; M1 – before, M2 – after, M3 – after 1 month, M4 – after 3 months. References
1. Korakakis V, Whiteley R, Tzavara A, Malliaropoulos N, The effectiveness of extracorporeal shockwave therapy in common lower limb conditions: A systematic review including quantification of patient-rated pain reduction: Br J Sports Med, 2018; 52; 387-407
2. Zhang Q, Fu C, Huang L, Efficacy of extracorporeal shockwave therapy on pain and function in myofascial pain syndrome of the trapezius: A systematic review and meta-analysis: Arch Phys Med Rehabil, 2020; 101; 1437-46
3. Ma H, Zhang W, Shi J, The efficacy and safety of extracorporeal shockwave therapy in knee osteoarthritis: A systematic review and meta-analysis: Int J Surg Lond Engl, 2020; 75; 24-34
4. Tengku Yusof TNB, Seow D, Vig KS, The musculoskeletal applications of extracorporeal shockwave therapy for foot and ankle disorders: A systematic review and meta-analysis: J Am Podiatr Med Assoc, 2021; 18-191
5. Surace SJ, Deitch J, Johnston RV, Buchbinder R, Shock wave therapy for rotator cuff disease with or without calcification: Cochrane Database Syst Rev, 2020; 3; CD008962
6. Taheri P, Khosrawi S, Ramezani M, Extracorporeal shock wave therapy combined with oral medication and exercise for chronic low back pain: A randomized controlled trial: Arch Phys Med Rehabil, 2021; 102; 1294-99
7. Walewicz K, Taradaj J, Rajfur K, The effectiveness of radial extracorporeal shock wave therapy in patients with chronic low back pain: A prospective, randomized, single-blinded pilot study: Clin Interv Aging, 2019; 14; 1859-69
8. Moon YE, Seok H, Kim SH, Extracorporeal shock wave therapy for sacroiliac joint pain: A prospective, randomized, sham-controlled short-term trial: J Back Musculoskelet Rehabil, 2017; 30; 779-84
9. Schneider R, Effectiveness of myofascial trigger point therapy in chronic back pain patients is considerably increased when combined with a new, integrated, low-frequency shock wave vibrotherapy (Cellconnect Impulse): A two-armed, measurement repeated, randomized, controlled pragmatic trial: J Back Musculoskelet Rehabil, 2018; 31; 57-64
10. Notarnicola A, Maccagnano G, Gallone MF, Extracorporeal shockwave therapy versus exercise program in patients with low back pain: Short-term results of a randomised controlled trial: J Biol Regul Homeost Agents, 2018; 32; 385-89
11. Han H, Lee D, Lee S, The effects of extracorporeal shock wave therapy on pain, disability, and depression of chronic low back pain patients: J Phys Ther Sci, 2015; 27; 397-99
12. Foldager CB, Kearney C, Spector M, Clinical application of extracorporeal shock wave therapy in orthopedics: Focused versus unfocused shock waves: Ultrasound Med Biol, 2012; 38; 1673-80
13. van der Worp H, van den Akker-Scheek I, van Schie H, Zwerver J, ESWT for tendinopathy: Technology and clinical implications: Knee Surg Sports Traumatol Arthrosc, 2013; 21; 1451-58
14. Opara J, Taradaj J, Walewicz K, The current state of knowledge on the clinical and methodological aspects of extracorporeal shock waves therapy in the management of post-stroke spasticity-overview of 20 years of experiences: J Clin Med, 2021; 10; E261
15. Walewicz K, Taradaj J, Dobrzyński M, Effect of radial extracorporeal shock wave therapy on pain intensity, functional efficiency, and postural control parameters in patients with chronic low back pain: A randomized clinical trial: J Clin Med, 2020; 9; 568
Figures
 Figure 1. CONSORT flow chart of study participants. fESWT – focused extracorporeal shock wave.
Figure 1. CONSORT flow chart of study participants. fESWT – focused extracorporeal shock wave. Figure 2. Duolith SD1 Tower device for high-energy fESWT.
Figure 2. Duolith SD1 Tower device for high-energy fESWT. Figure 3. fESWT applicator used in this study.
Figure 3. fESWT applicator used in this study. Figure 4. Treatment session using the fESWT applicator.
Figure 4. Treatment session using the fESWT applicator. Figure 5. Comparison of VAS scores obtained in 4 measurements between the experimental and control group. fESWT – focused extracorporeal shock wave; M1 – before, M2 – after, M3 – after 1 month, M4 – after 3 months.
Figure 5. Comparison of VAS scores obtained in 4 measurements between the experimental and control group. fESWT – focused extracorporeal shock wave; M1 – before, M2 – after, M3 – after 1 month, M4 – after 3 months. Figure 6. Comparison of LPS scores obtained in 4 measurements between the experimental and control group. fESWT – focused extracorporeal shock wave; M1 – before, M2 – after, M3 – after 1 month, M4 – after 3 months.
Figure 6. Comparison of LPS scores obtained in 4 measurements between the experimental and control group. fESWT – focused extracorporeal shock wave; M1 – before, M2 – after, M3 – after 1 month, M4 – after 3 months. Figure 7. Comparison of ODI scores obtained in 4 measurements between the experimental and control group. fESWT – focused extracorporeal shock wave; M1 – before, M2 – after, M3 – after 1 month, M4 – after 3 months.
Figure 7. Comparison of ODI scores obtained in 4 measurements between the experimental and control group. fESWT – focused extracorporeal shock wave; M1 – before, M2 – after, M3 – after 1 month, M4 – after 3 months. Tables
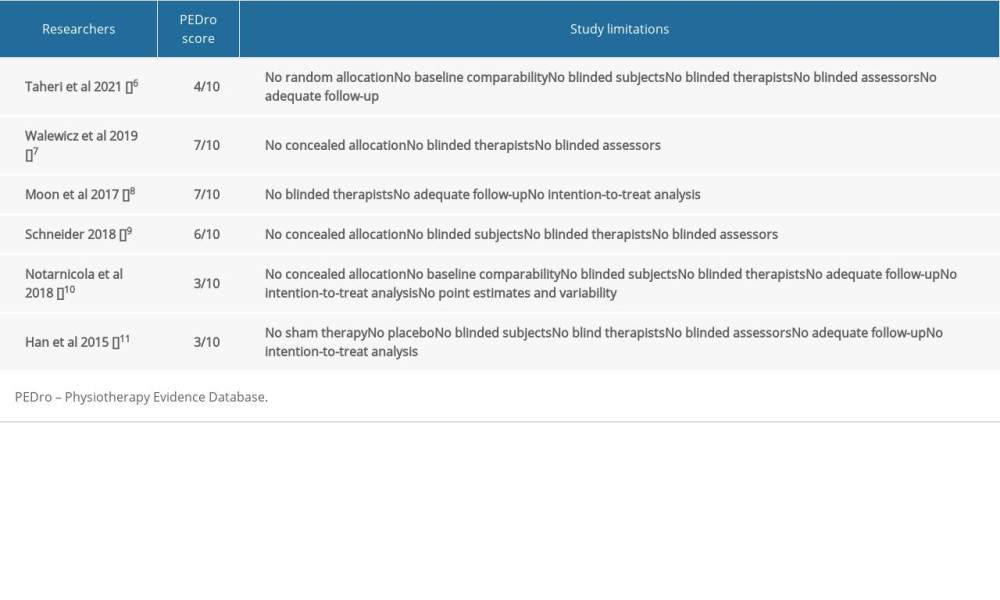 Table 1. A randomized clinical trial addressing the treatment of LBP using ESWT.
Table 1. A randomized clinical trial addressing the treatment of LBP using ESWT.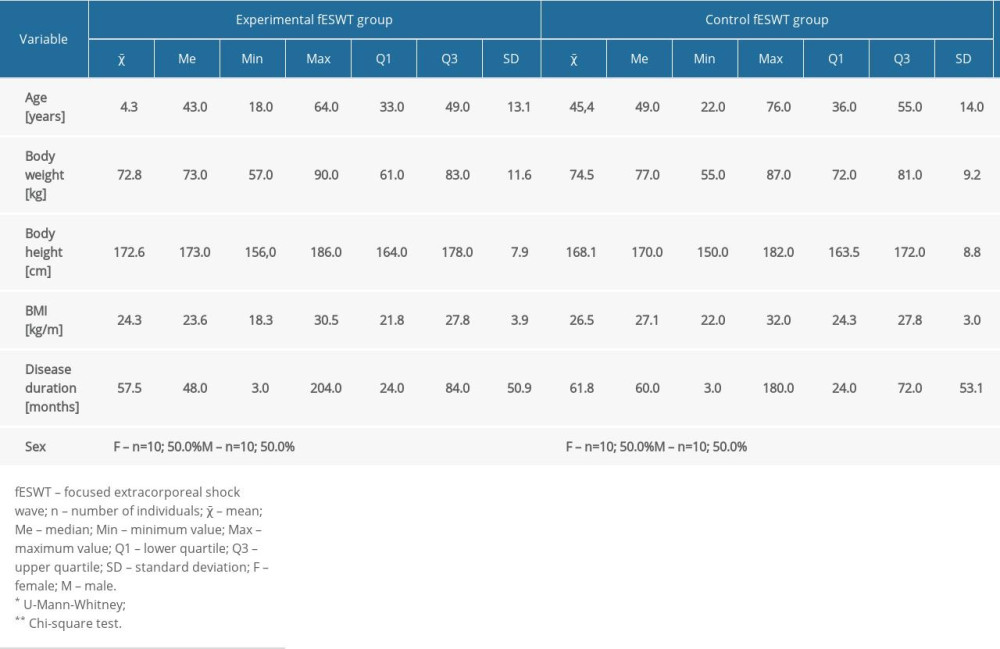 Table 2. Characteristics of the study groups.
Table 2. Characteristics of the study groups.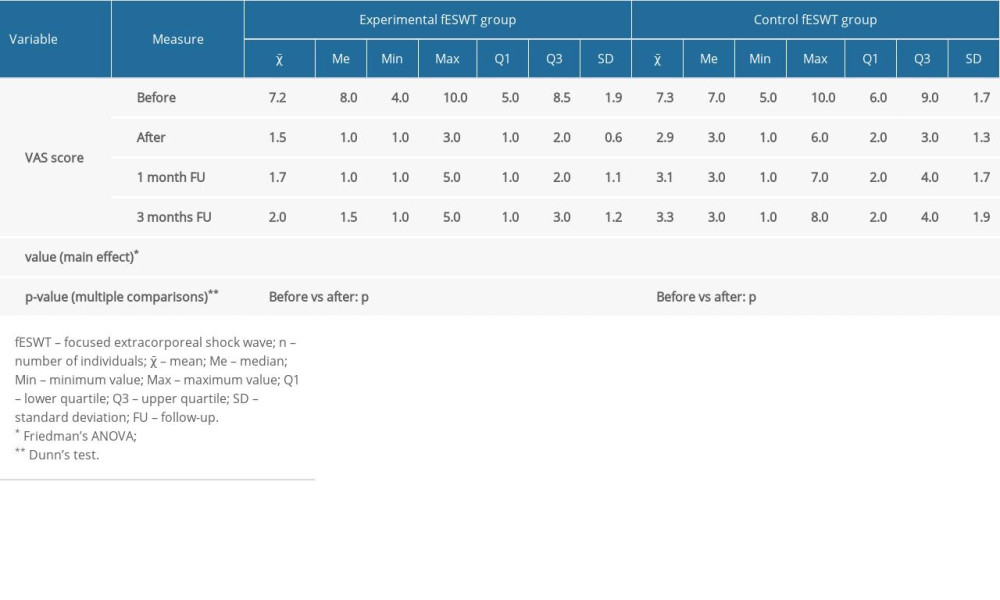 Table 3. VAS scores in both groups.
Table 3. VAS scores in both groups.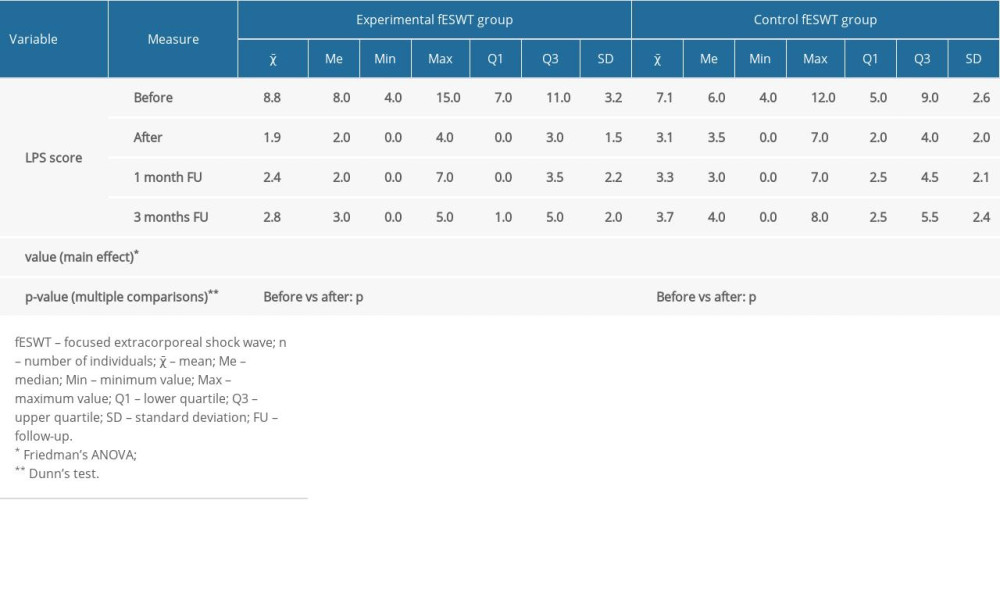 Table 4. LPS scores in both groups.
Table 4. LPS scores in both groups.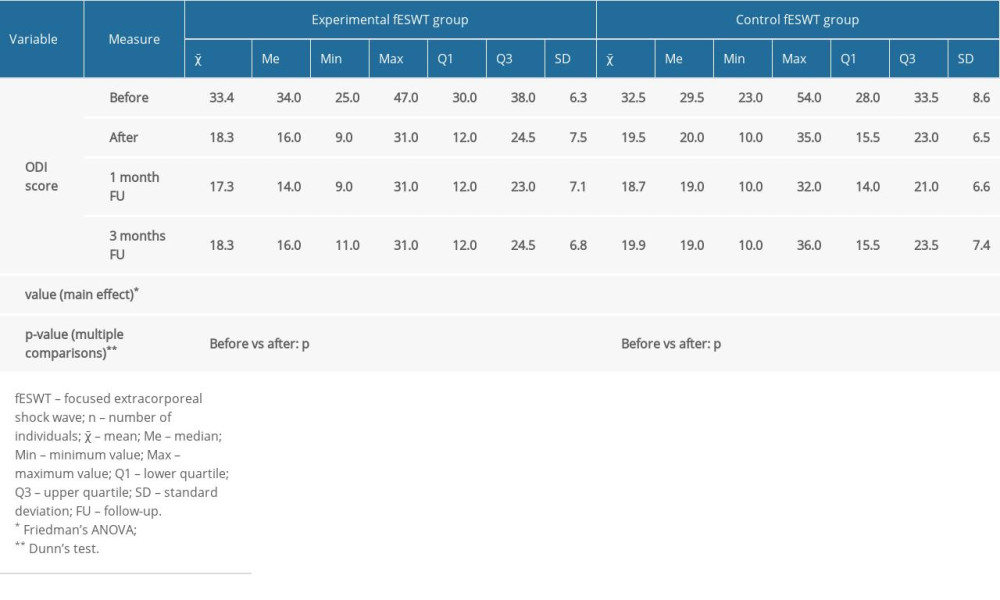 Table 5. ODI scores in both groups.
Table 5. ODI scores in both groups. Table 1. A randomized clinical trial addressing the treatment of LBP using ESWT.
Table 1. A randomized clinical trial addressing the treatment of LBP using ESWT. Table 2. Characteristics of the study groups.
Table 2. Characteristics of the study groups. Table 3. VAS scores in both groups.
Table 3. VAS scores in both groups. Table 4. LPS scores in both groups.
Table 4. LPS scores in both groups. Table 5. ODI scores in both groups.
Table 5. ODI scores in both groups. In Press
05 Mar 2024 : Clinical Research
Role of Critical Shoulder Angle in Degenerative Type Rotator Cuff Tears: A Turkish Cohort StudyMed Sci Monit In Press; DOI: 10.12659/MSM.943703
06 Mar 2024 : Clinical Research
Comparison of Outcomes between Single-Level and Double-Level Corpectomy in Thoracolumbar Reconstruction: A ...Med Sci Monit In Press; DOI: 10.12659/MSM.943797
21 Mar 2024 : Meta-Analysis
Economic Evaluation of COVID-19 Screening Tests and Surveillance Strategies in Low-Income, Middle-Income, a...Med Sci Monit In Press; DOI: 10.12659/MSM.943863
10 Apr 2024 : Clinical Research
Predicting Acute Cardiovascular Complications in COVID-19: Insights from a Specialized Cardiac Referral Dep...Med Sci Monit In Press; DOI: 10.12659/MSM.942612
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952








