26 October 2022: Clinical Research
Evaluation of Orthodontic Mini-Implant Placement in the Maxillary Anterior Alveolar Region in 15 Patients by Cone Beam Computed Tomography at a Single Center in South India
Arathi Murugesan1BDF, S.P. Saravana Dinesh1BDF, Srirengalakshmi Muthuswamy Pandian1BDE, Lichi Ashwin Solanki1ABC, Abdulrahman Alshehri2CDE, Wael Awadh2BDF, Khalid J. AlzahraniDOI: 10.12659/MSM.937949
Med Sci Monit 2022; 28:e937949
Abstract
BACKGROUND: In this study, we aimed to evaluate orthodontic mini-implant placement in the maxillary anterior alveolar region by cone beam computed tomography (CBCT) in 15 patients at a single center in South India.
MATERIAL AND METHODS: A total of 15 CBCT scans of orthodontic patients after completion of leveling and aligning stage were included. The thickness of labial alveolar bone, labio-palatal bone, and inter-radicular distance between the maxillary central incisors (U1-U1), maxillary central and lateral incisor (U1-U2), and maxillary lateral incisor and canine (U2-U3) at vertical levels 4 mm, 6 mm, and 8 mm above the interdental cementoenamel junction were measured. Descriptive statistics, ANOVA, and Tukey post hoc tests were done to assess the differences among the groups. An independent t test was done to analyze differences by sex.
RESULTS: The thickness of cortical bone in the labial region was higher in the U2-U3 site than in the U1-U1 site, at a height of 4 mm. Also, there was a significant difference between 4 mm and 8 mm heights in the U2-U3 region. No significant difference was noted in bone dimensions among men and women and in the labio-palatal bone thickness among the different sites. The inter-radicular distance was the highest between the U2-U3 site, while it was the lowest in the U1-U2 site.
CONCLUSIONS: The findings from this center showed that when CBCT was used to evaluate orthodontic mini-implant placement in the maxillary anterior alveolar region, the U2-U3 and U1-U1 locations at heights between 6 mm to 8 mm apical to the interdental cementoenamel junction were optimal for placement of the mini-implants.
Keywords: Bone Development, Maxilla, Orthodontics, Corrective, Female, Animals, Dental Implants, Alveolar Process, Orthodontic Anchorage Procedures, Cone-Beam Computed Tomography
Background
The most important factor for successful orthodontic treatment is anchorage control. The introduction of mini-implants/mini-screws as a skeletal anchorage device can provide absolute anchorage during various movements of the tooth, such as anterior retraction, anterior intrusion, molar intrusion, molar distalization, and molar protraction [1–5]. The advantages of mini-implants over other skeletal anchorage devices, such as miniplates, plates, and dental implants, are their small size, ease of placement and removal, decreased discomfort, increased number of placement sites, lack of surgical defects, and immediate loading [6–11].
Mini-implants are commonly inserted in the inter-radicular alveolar bone. Successful placement of the mini-implant requires a thorough knowledge of the root morphology of the adjacent teeth, distance between the radicular bone, thickness of the alveolar bone, and technique of mini-implant placement [3]. Various clinical guidelines have also been proposed regarding the placement of inter-radicular implants, including that the inter-root distance must be greater than 3 mm [12] and that, to avoid any root damage, the path of a mini-implant placement should be angulated [7]. Some authors also suggest that mini-implants can even be inserted in cases in which the inter-radicular distances are less than 3 mm, if the bone thickness along the path of insertion is greater than the length of the threaded portion [13].
Even though inter-radicular implants are most commonly positioned in the posterior alveolus for retraction, they can also be placed in the anterior alveolus for anterior intrusion and molar protraction [14–21]. The prevalence of vertical maxillary excess in the Brazilian population, as well as the Asian population, was reported to be nearly 22% [22], whereas it was nearly 30% in the South Indian population [23]. Vertical maxillary excess and gummy smile of mild to moderate severity are very well camouflaged by the mini-implant-aided anterior intrusion [14–21].
The placement of a mini-implant in the anterior regions could also be used for purposes of molar protraction in cases of congenitally missing teeth. According to the Misch classification of bone density, the anterior part of the maxilla falls into the category of D2 and D3 bone, which is thin and porous [24]. Hence, it is essential to evaluate the thickness of the cortical bone for predicting the long-term stability of mini-implants placed in the anterior region if used for protraction of posterior teeth, which have a greater root surface area than anterior teeth.
Cone beam computed tomography (CBCT) is an accurate radiographic method widely used for evaluating bone morphology [25]. There are many studies using CBCT for assessing bone thickness in the molar, premolar, and mid-palatal areas for mini-implant placement [12,13,26–29]. There is a considerably high prevalence of vertical maxillary excess in the South Indian population, while there are few studies assessing the anterior alveolar bone thickness for orthodontic mini-implant placement. Therefore, the present study was conducted to assess the labial bone thickness, labio-palatal bone thickness, and inter-radicular distance using CBCT and to determine the ideal site for positioning of mini-screws in the upper anterior region in the South Indian population. The variation in bone thickness by sex was also evaluated. Therefore, this study aimed to evaluate orthodontic mini-implant placement in the maxillary anterior alveolar region by CBCT in 15 patients at a single center in South India.
Material and Methods
MEASUREMENTS:
CBCT evaluations were performed using Galileos Viewer Software (Model v 22.8, Denstply Sirona). For making measurements, the maxillary occlusal plane was used as the horizontal reference plane. The thickness of the cortical bone on the labial side (Figure 1), labio-palatal bone thickness (Figure 1), and inter-radicular thickness (Figure 2) were measured between the 3 interdental root areas, specifically, between U1-U1, U1–U2, and U2–U3. Each of the measurements was performed at 3 vertical levels, namely, 4 mm, 6 mm, and 8 mm apical to the interdental CEJ (Figure 3). Labio-palatal bone thickness was measured from the labial side of the labial cortical plate to the palatal side of the palatal cortical plate or the labial wall of the incisive canal in the order of occurrence [25]. Similarly, the inter-radicular distance was also measured in the narrowest interdental region. Measurements were made on both sides and the mean value of the right and left sides for each sample was used for statistical analyses.
STATISTICAL ANALYSIS:
All measurements were examined by a single investigator. Intra-examiner reliability was performed by repeating the measurements in 8 randomly selected samples after 2 weeks, and an intraclass correlation coefficient test revealed 0.96, which indicated excellent intra-examiner reliability. The Shapiro-Wilk test showed normally distributed data. An independent
Results
LABIAL CORTICAL BONE THICKNESS:
The labial cortical bone thickness was highest between U2–U3, at a height of 8 mm (1.16±0.22 mm). The lowest thickness of 0.71±0.12 mm was observed between U1-U1 at 4 mm (Table 1). A statistically significant difference was noted in the thickness of labial cortical (compact) bone between 4 mm and 8 mm in all 3 sites (Table 4). The cortical bone thickness increased as the distance from the CEJ increased apically. A critical distinction was additionally noted in the range of 6 mm and 8 mm in the U2–U3 site. The thickness was more in the U2–U3 site when compared with the U1-U1 site at a height of 4 mm from the CEJ. (Table 5)
LABIO-PALATAL BONE THICKNESS:
A minimum of 8 mm of labio-palatal bone thickness was observed in all the sites assessed (Table 2). There was no critical distinction in the labio-palatal bone thickness between the various sites at different vertical levels (Tables 4, 5).
INTER-RADICULAR DISTANCE:
The inter-radicular distance increased as it moved apically away from the CEJ. A maximum distance of 4.21±0.98 mm was seen between the U2–U3 site at a level of 8 mm and the lowest distance of 2.78±0.88 mm was seen between the U1–U2 site at a level of 4 mm (Table 3). A statistically significant difference in the inter-radicular distance was observed between sites U1-U1 and U1–U2 and between sites U2–U3 and U1–U2 at all 3 vertical levels (Table 5). A significant difference was also noted between 4 mm and 8 mm at sites U1-U1 and U2–U3 (Table 4).
Discussion
The use of mini-implants in the maxillary region is expanding very rapidly [14–21]. Mini-implants are advantageous over the conventional intrusion arches in obtaining true maxillary anterior intrusion with minimal sagittal and vertical anchorage loss of the posteriors [18,19]. The safety and strength of the mini-implants depend upon the thickness of the bone and the proximity of the implant to the vital anatomical structures [30–32]. Bone thickness is known to vary among different races and ethnicities. Therefore, the present study evaluated the thickness of the labial cortical plate, labio-palatal bone, and inter-radicular distance in the maxillary anterior region in the South Indian population. The study sample comprised South Indian participants. A similar study was carried out in other populations, such as with Korean participants. Hence, the establishment of a standard norm for the South Indian population was the aim of this present study. We also evaluated sex variation in bone dimensions. The measurements were performed on CBCT scans taken after the completion of the leveling and aligning stage, as that is the ideal time when the implants are placed for intrusion. This was done to ensure that the teeth tip and torque were expressed almost equally for all patients and also to assess whether the inter-radicular distance obtained after alignment would be adequate for the safe placement of the mini-implants.
The results of the study showed that the sites U2–U3 and U1-U1 at a height of 6 mm to 8 mm were the best for placement of mini-implants, according to the amount of labial cortical thickness, labio-palatal bone thickness, and inter-radicular distance available. Also, there was no considerable difference in bone dimensions between men and women.
Cortical bone thicknesses of 0.02±0.09 to 0.52±0.54 mm, 0.04±0.19 to 0.48±0.59 mm, and 0.1±0.29 to 1.46±0.47 mm were seen in the U1-U1, U1–U2, and U2–U3 sites at levels of 4 mm and 6 mm apical to the CEJ, respectively, in a study by Lee et al in 2009. The thickness of compact bone at a height of 8 mm was more than that observed at 4 mm but less than that seen at 6 mm, which only partly agreed with the results of the present study [13]. In another study conducted in a Korean population by Choi et al [25], the alveolar bone measured 0.70±0.27 mm to 0.90±0.34 mm, 1±0.30 mm to 1.10±0.21 mm, and 1.15±0.27 mm to 1.20±0.13 mm in the U1-U1, U1–U2, and U2–U3 sites at levels of 4 mm to 8 mm apical to the interdental CEJ, respectively. Sadek et al [33] compared the thickness of the buccal compact bone at all inter-radicular sites in the maxilla for different vertical growth patterns and reported an average thickness of 0.8 to 0.9 mm of compact bone in the anterior maxilla in all 3 growth patterns, with no significant differences among the groups; their results were not consistent with the values obtained in the present study. Casetta et al and Ono et al revealed that the thickness and density of the compact bone were lower in the maxillary anterior segment than in the posterior segment. They also stated that a difference in cortical bone thickness by sex was noted in the previous studies, in which they observed men had thicker cortical bone than women [34,35]. However, this variation was significant in the posterior region, which can be attributed to the higher biting force of the men, whereas there was no difference in thickness of bone in the anterior region between men and women. The results of these studies were similar to those we observed in this study.
In the present study, there were no variations noted in the labio-palatal bone thickness between the various sites, with measure values of 7.95±1.99 mm to 9.81±2.34 mm. In the U1-U1 site, the thickness was limited by the presence of the incisive canal. A similar range was observed in the study done by Choi et al [25]; however, they observed that the thickness was significantly high in the U1–U2 site, while it was low in the U1-U1 site.
In the present study, the inter-radicular distance was high in the U2–U3 site, whereas it was the low in the U1–U2 site. This was expected because the measurements were taken after the completion of leveling and aligning using the MBT bracket prescription. The inter-radicular distance increased as it moved apically from the CEJ in all 3 sites. Choi et al [25] observed a similar trend in the inter-radicular distance when measured on pre-treatment CBCT scans. Analyzing the results obtained for all 3 parameters in the present study, we observed that the sites U1-U1 and U2–U3, at a vertical level of 6 mm and 8 mm with the maximum buccal cortical bone thickness and an average inter-radicular distance of 3 mm, are the ideal sites for anterior mini-implant positioning. Assuming the thickness of the mini-implant to be 1.5 mm and a clearance of 1 mm of bone on either side of the implant, a minimum of 3 mm of inter-radicular distance is essential for the safe placement of implants, as stated by Schnelle et al and Park et al [12,36]. With a labio-palatal bone thickness of 7.95±1.99 mm to 9.81±2.34 mm, mini-implants of lengths 8 mm to 9 mm can be placed safely with or without angulation in the maxillary anterior region. Atalla et al and Sosly et al concluded in their systematic reviews that anterior mini-implants can be efficiently used for maxillary anterior teeth intrusion [37,38]. Alsamak et al [39] concluded in their systematic review that the optimal site of placement of mini-implants in the anterior maxilla is between the canine and first premolar, whereas Fayed et al [40] concluded the optimal site is between the central and lateral incisors. Also, maxillary anterior intrusion with good control over buccal angulation is seen when using 2 mini-implants that are placed between the canine and lateral incisor on right as well as the left side, rather than a single midline implant, as reported by Vela-Hernández [41].
The ideal bone thickness of mini-implants has been discussed by numerous authors, as stated above. Bone thickness is positively correlated to the success rates of mini-implant placement, which in turn affects the outcome of the orthodontic treatment [13]. Hence, it is essential to know the optimal bone thickness at the most common mini-implant placement sites [33].
All the studies that measured bone thickness in the maxillary and mandibular jaw have used only the CBCT technique. CBCT offers the highest possible accuracy in linear measurements of cortical thickness. Tsutsumi et al stated that conventional methods cannot accurately assess bone thickness [42].
The limitations of the present study include a smaller sample size, with only patients with Class I skeletal and average growth patterns being included. At the same time, attempts were made to limit the confounding variables by including only patients with similar growth patterns and an almost equal number of men and women. A shortcoming of using this method for assessing bone thickness would be the variations in the height of the CEJ of adjacent teeth, as that was used as a reference landmark. Along with this, the patients were not classified based on their bone density, which might vary among individuals.
This study provides help in choosing locations for mini-implants in the anterior part of the maxilla. Future studies assessing the same topic in different skeletal growth patterns and larger sample sizes are recommended for validation of the present results. These should discuss the results and how they can be interpreted from the perspective of previous studies and the working hypotheses. The findings and their implications should be discussed in the broadest context possible. Future research directions may also be highlighted.
Conclusions
The findings from this center showed that when CBCT was used to evaluate orthodontic mini-implant placement in the maxillary anterior alveolar region, the U2–U3 and U1-U1 locations at a height of between 6 mm to 8 mm apical to the interdental CEJ were optimal for anterior placement of the mini-implants.
Figures
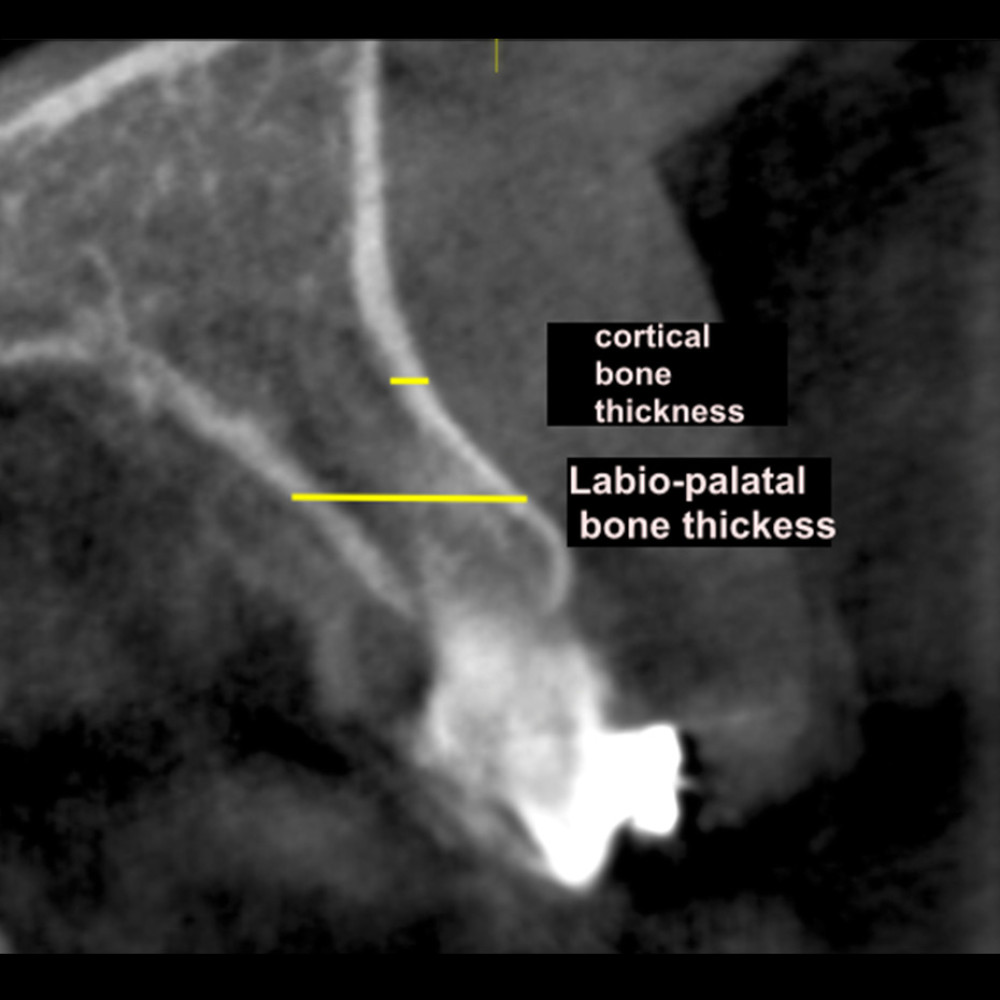 Figure 1. Method of measurement of labial cortical thickness and labio-palatal bone thickness in sagittal view.
Figure 1. Method of measurement of labial cortical thickness and labio-palatal bone thickness in sagittal view. 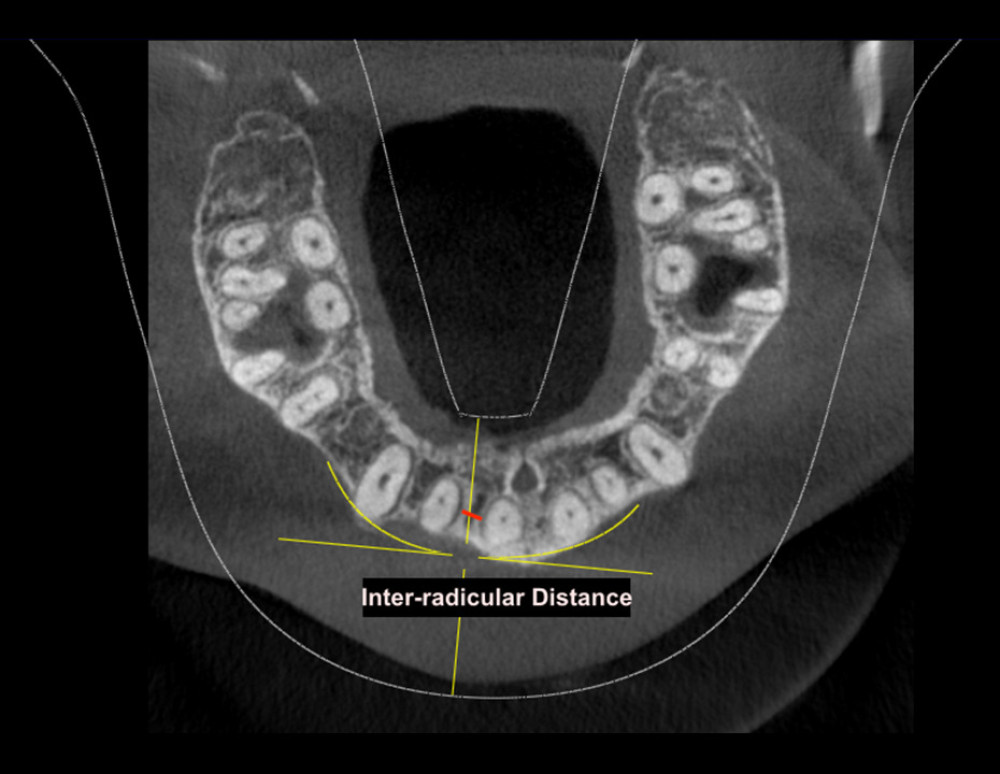 Figure 2. Method of measurement of inter-radicular distance in axial view.
Figure 2. Method of measurement of inter-radicular distance in axial view. 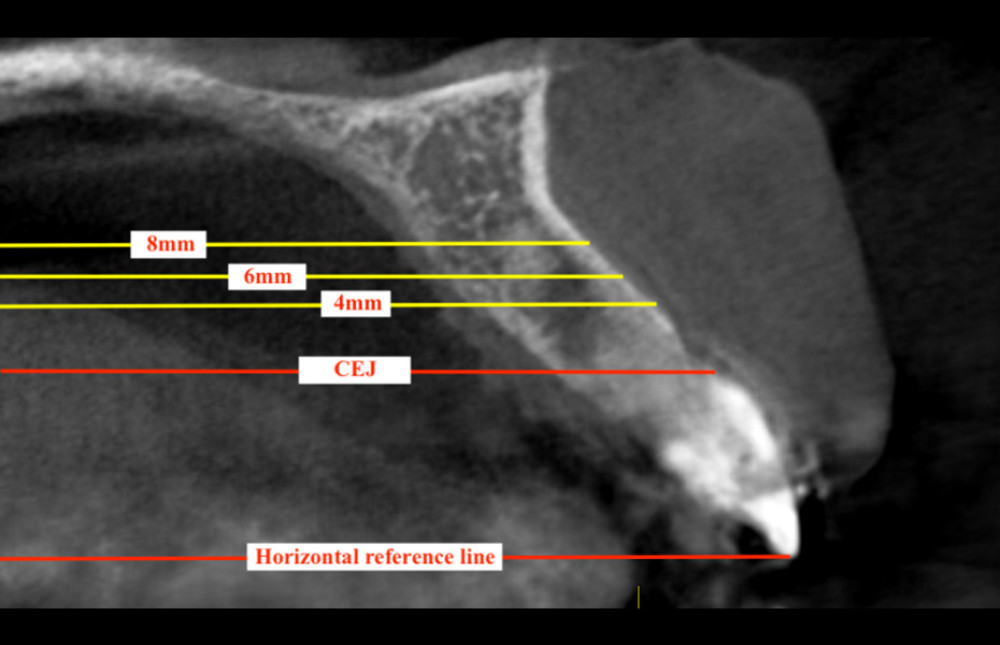 Figure 3. Markings of horizontal reference line and interdental cementoenamel junction. Bone thickness measured at reference lines of 4 mm, 6 mm, and 8 mm above the cementoenamel junction.
Figure 3. Markings of horizontal reference line and interdental cementoenamel junction. Bone thickness measured at reference lines of 4 mm, 6 mm, and 8 mm above the cementoenamel junction. Tables
Table 1. Descriptive statistics for labial cortical bone thickness.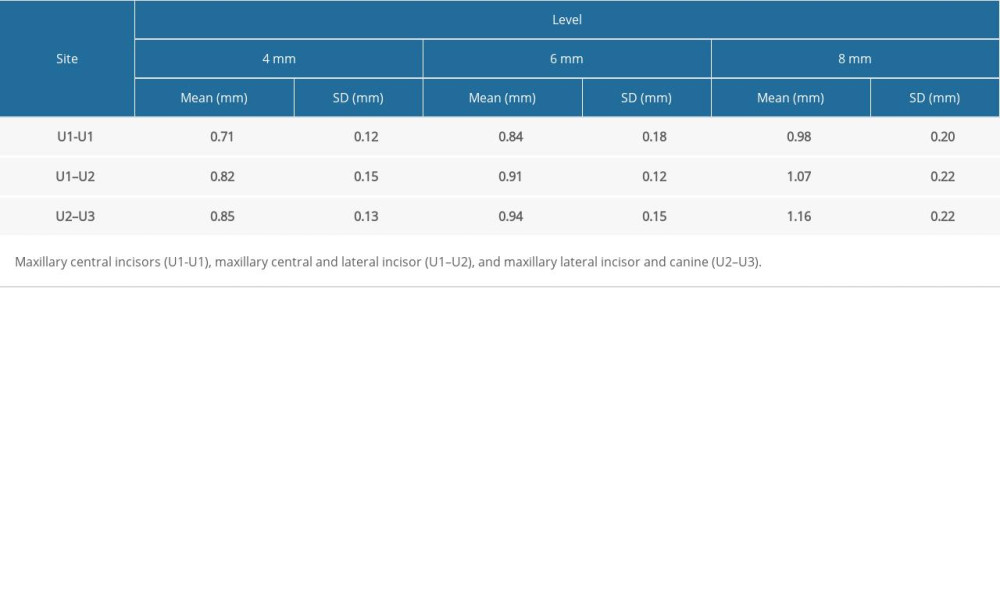 Table 2. Descriptive statistics for labio-palatal bone thickness.
Table 2. Descriptive statistics for labio-palatal bone thickness.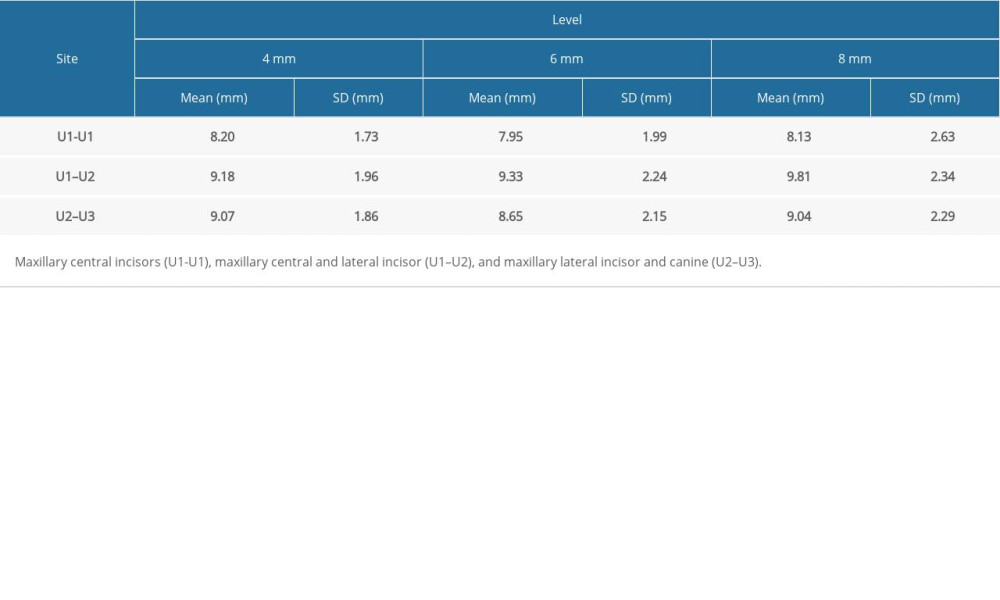 Table 3. Descriptive statistics for inter-radicular distance.
Table 3. Descriptive statistics for inter-radicular distance.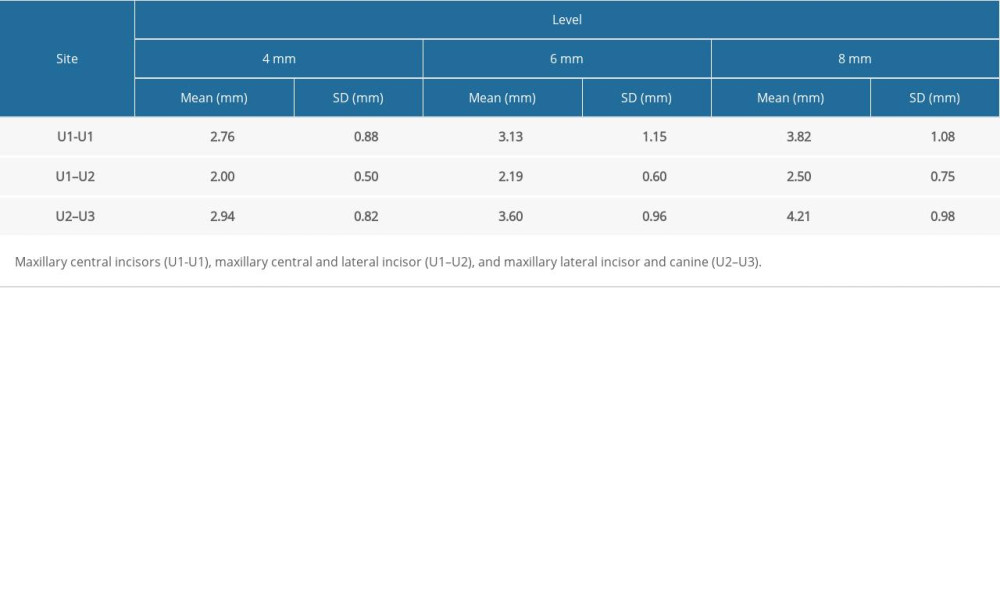 Table 4. Significance value obtained from ANOVA and Tukey post hoc tests comparing the mean difference of cortical thickness, labio-palatal bone thickness, and inter-radicular distance between 4 mm, 6 mm, and 8 mm.
Table 4. Significance value obtained from ANOVA and Tukey post hoc tests comparing the mean difference of cortical thickness, labio-palatal bone thickness, and inter-radicular distance between 4 mm, 6 mm, and 8 mm.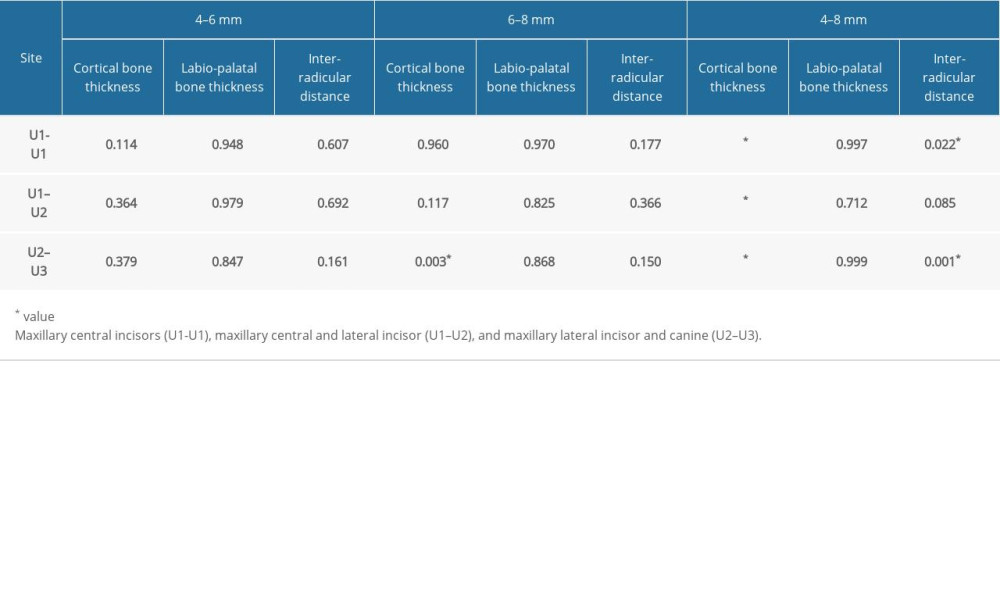 Table 5. Significance value obtained from ANOVA and Tukey post hoc tests comparing the mean difference of cortical thickness, labio-palatal bone thickness, and inter-radicular distance between the sites.
Table 5. Significance value obtained from ANOVA and Tukey post hoc tests comparing the mean difference of cortical thickness, labio-palatal bone thickness, and inter-radicular distance between the sites.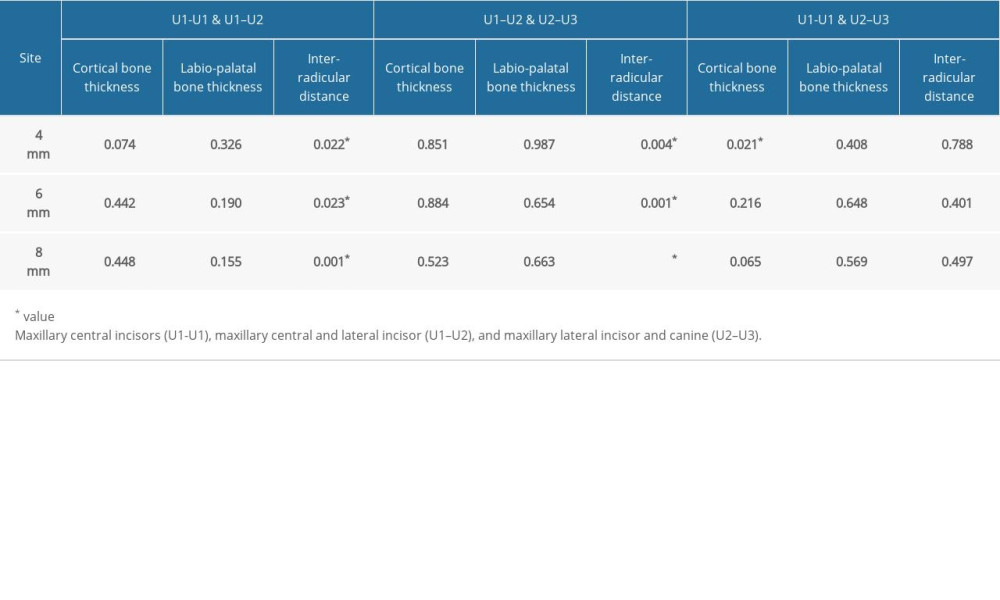
References
1. Paik C-H, Woo YJBR, Treatment of an adult patient with vertical maxillary excess using miniscrew fixation: J Clin Orthod, 2003; 37; 423-28
2. Park Y-C, Lee S-Y, Kim D-H, Jee S-H, Intrusion of posterior teeth using mini-screw implants: Am J Orthod Dentofac Orthop, 2003; 123; 690-94
3. Lin JCY, Liou EJW, A new bone screw for orthodontic anchorage: J Clin Orthod, 2003; 37; 676-81
4. Kuroda S, Katayama AT-YT, Severe anterior open-bite case treated using titanium screw anchorage: Angle Orthod, 2004; 74; 558-67
5. Park HS, Bae SM, Kyung HMSJ, Simultaneous incisor retraction and distal molar movement with microimplant anchorage: World J Orthod, 2004; 5; 164-71
6. Costa A, Raffainl MMB, Miniscrews as orthodontic anchorage: A preliminary report: Int J Adult Orthod Orthognath Surg, 1998; 13; 201-9
7. Park HS, Kwon OWSJ, Microscrew implant anchorage sliding mechanics: World J Orthod, 2005; 6; 265-74
8. Kitai N, Yasuda Y, Takada K, A stent fabricated on a selectively colored stereolithographic model for placement of orthodontic mini-implants: Int J Adult Orthod Orthognath Surg, 2002; 17; 264-66
9. Ohmae M, Saito S, Morohashi T, A clinical and histological evaluation of titanium mini-implants as anchors for orthodontic intrusion in the beagle dog: Am J Orthod Dentofac Orthop, 2001; 119; 489-97
10. Kanoni R, Mini-implant for orthodontic anchorage: J Clin Orthod, 1997; 31; 763-67
11. Lee CYS, Immediate load protocol for anterior maxilla with cortical bone from mandibular ramus: Implant Dent, 2006; 15; 153-59
12. Schnelle MA, Beck FM, Jaynes RMHS, A radiographic evaluation of the availability of bone for placement of miniscrews: Angle Orthod, 2004; 74; 832-37
13. Lee K-J, Joo E, Kim K-D, Computed tomographic analysis of tooth-bearing alveolar bone for orthodontic miniscrew placement: Am J Orthod Dentofac Orthop, 2009; 135; 486-94
14. Ohnishi H, Yagi T, Yasuda YTK, A mini-implant for orthodontic anchorage in a deep overbite case: Angle Orthod, 2005; 75; 444-52
15. Deguchi T, Murakami T, Kuroda S, Comparison of the intrusion effects on the maxillary incisors between implant anchorage and J-hook headgear: Am J Orthod Dentofac Orthop, 2008; 133; 654-60
16. Lin JCY, Liou EJWBS, Simultaneous reduction in vertical dimension and gummy smile using miniscrew anchorage: J Clin Orthod, 2010; 44; 157-70
17. Saxena R, Kumar PS, Upadhyay M, Naik V, A clinical evaluation of orthodontic mini-implants as intraoral anchorage for the intrusion of maxillary anterior teeth: World J Orthod, 2010; 11; 346-51
18. Polat-Özsoy Ö, Arman-Özçırpıcı A, Veziroğlu F, Çetinşahin A, Comparison of the intrusive effects of miniscrews and utility arches: Am J Orthod Dentofac Orthop, 2011; 139; 526-32
19. Şenışık NE, Türkkahraman H, Treatment effects of intrusion arches and mini-implant systems in deepbite patients: Am J Orthod Dentofac Orthop, 2012; 141; 723-33
20. Kaku M, Kojima S, Sumi H, Gummy smile and facial profile correction using miniscrew anchorage: Angle Orthod, 2012; 82; 170-77
21. Kaku M, Kojima S, Sumi HK, Gummy smile and facial profile correction using miniscrew anchorage: Angle Orthod, 2012; 82; 758
22. Bansal AK, Sharma M, Kumar P, Long face syndrome: A literature review: J Dent Heal Oral Disord Ther, 2015; 2; 1-2
23. Kumar N, Prevalence of vertical maxillary excess – an institution based retrospective study: Int J Dent Oral Sci, 2021; 3108-12
24. Misch CE, Dietsh-Misch F, Hoar J, A bone quality-based implant system: First year of prosthetic loading: J Oral Implantol, 1999; 25; 185-97
25. Choi JH, Yu HS, Lee KJ, Park YC, Three-dimensional evaluation of maxillary anterior alveolar bone for optimal placement of miniscrew implants: Korean J Orthod, 2014; 44; 54
26. Gahleitner A, Podesser B, Schick S, Dental CT and orthodontic implants: Imaging technique and assessment of available bone volume in the hard palate: Eur J Radiol, 2004; 51; 257-62
27. Deguchi T, Nasu M, Murakami K, Quantitative evaluation of cortical bone thickness with computed tomographic scanning for orthodontic implants: Am J Orthod Dentofac Orthop, 2006; 129; 721e7-e12
28. Kim J-H, Park Y-C, Evaluation of mandibular cortical bone thickness for placement of temporary anchorage devices (TADs): Korean J Orthod, 2012; 42; 110
29. Farnsworth D, Rossouw PE, Ceen RF, Buschang PH, Cortical bone thickness at common miniscrew implant placement sites: Am J Orthod Dentofac Orthop, 2011; 139; 495-503
30. Chen Y, Kyung HM, Zhao WT, Yu WJ, Critical factors for the success of orthodontic mini-implants: A systematic review: Am J Orthod Dentofac Orthop, 2009; 135; 284-91
31. Yang L, Li F, Cao M, Quantitative evaluation of maxillary interradicular bone with cone-beam computed tomography for bicortical placement of orthodontic mini-implants: Am J Orthod Dentofac Orthop, 2015; 147; 725-37
32. Poggio PM, Incorvati C, Velo SCA, “Safe Zones”: A guide for miniscrew positioning in the maxillary and mandibular arch: Angle Orthod”, 2006; 76; 191-97
33. Sadek MM, Sabet NE, Hassan IT, Three-dimensional mapping of cortical bone thickness in subjects with different vertical facial dimensions: Prog Orthod, 2016; 17; 32
34. Cassetta M, Sofan A, Altieri F, Barbato E, Evaluation of alveolar cortical bone thickness and density for orthodontic mini-implant placement: J Clin Exp Dent, 2013; 5; e245-52
35. Ono A, Motoyoshi M, Shimizu N, Cortical bone thickness in the buccal posterior region for orthodontic mini-implants: Int J Oral Maxillofac Surg, 2008; 37; 334-40
36. Park H-S, Jeong S-H, Kwon O-W, Factors affecting the clinical success of screw implants used as orthodontic anchorage: Am J Orthod Dentofac Orthop, 2006; 130; 18-25
37. Atalla AI, AboulFotouh MH, Fahim FHFM, Effectiveness of orthodontic mini-screw implants in adult deep bite patients during incisor intrusion: A systematic review: Contemp Clin Dent, 2019; 10; 372-81
38. Sosly R, Mohammed H, Rizk MZ, Effectiveness of miniscrew-supported maxillary incisor intrusion in deep-bite correction: A systematic review and meta-analysis: Angle Orthod, 2020; 90; 291-304
39. Alsamak S, Psomiadis S, Gkantidis N, Positional guidelines for orthodontic mini-implant placement in the anterior alveolar region: A systematic review: Int J Oral Maxillofac Implants, 2013; 28(2); 470-79
40. Fayed MM, Pazera P, Katsaros C, Optimal sites for orthodontic mini-implant placement assessed by cone beam computed tomography: Angle Orthod, 2010; 80(5); 939-51
41. Vela-Hernández A, Gutiérrez-Zubeldia L, López-García R, One versus two anterior miniscrews for correcting upper incisor overbite and angulation: A retrospective comparative study: Prog Orthod, 2020; 21; 34
42. Tsutsumi K, Chikui T, Okamura KYK, Accuracy of linear measurement and the measurement limits of thin objects with cone beam computed tomography: Effects of measurement directions and of phantom locations in the fields of view: Int J Oral Maxillofac Implants, 2011; 26; 91-100
Figures
 Figure 1. Method of measurement of labial cortical thickness and labio-palatal bone thickness in sagittal view.
Figure 1. Method of measurement of labial cortical thickness and labio-palatal bone thickness in sagittal view. Figure 2. Method of measurement of inter-radicular distance in axial view.
Figure 2. Method of measurement of inter-radicular distance in axial view. Figure 3. Markings of horizontal reference line and interdental cementoenamel junction. Bone thickness measured at reference lines of 4 mm, 6 mm, and 8 mm above the cementoenamel junction.
Figure 3. Markings of horizontal reference line and interdental cementoenamel junction. Bone thickness measured at reference lines of 4 mm, 6 mm, and 8 mm above the cementoenamel junction. Tables
 Table 1. Descriptive statistics for labial cortical bone thickness.
Table 1. Descriptive statistics for labial cortical bone thickness. Table 2. Descriptive statistics for labio-palatal bone thickness.
Table 2. Descriptive statistics for labio-palatal bone thickness. Table 3. Descriptive statistics for inter-radicular distance.
Table 3. Descriptive statistics for inter-radicular distance. Table 4. Significance value obtained from ANOVA and Tukey post hoc tests comparing the mean difference of cortical thickness, labio-palatal bone thickness, and inter-radicular distance between 4 mm, 6 mm, and 8 mm.
Table 4. Significance value obtained from ANOVA and Tukey post hoc tests comparing the mean difference of cortical thickness, labio-palatal bone thickness, and inter-radicular distance between 4 mm, 6 mm, and 8 mm. Table 5. Significance value obtained from ANOVA and Tukey post hoc tests comparing the mean difference of cortical thickness, labio-palatal bone thickness, and inter-radicular distance between the sites.
Table 5. Significance value obtained from ANOVA and Tukey post hoc tests comparing the mean difference of cortical thickness, labio-palatal bone thickness, and inter-radicular distance between the sites. Table 1. Descriptive statistics for labial cortical bone thickness.
Table 1. Descriptive statistics for labial cortical bone thickness. Table 2. Descriptive statistics for labio-palatal bone thickness.
Table 2. Descriptive statistics for labio-palatal bone thickness. Table 3. Descriptive statistics for inter-radicular distance.
Table 3. Descriptive statistics for inter-radicular distance. Table 4. Significance value obtained from ANOVA and Tukey post hoc tests comparing the mean difference of cortical thickness, labio-palatal bone thickness, and inter-radicular distance between 4 mm, 6 mm, and 8 mm.
Table 4. Significance value obtained from ANOVA and Tukey post hoc tests comparing the mean difference of cortical thickness, labio-palatal bone thickness, and inter-radicular distance between 4 mm, 6 mm, and 8 mm. Table 5. Significance value obtained from ANOVA and Tukey post hoc tests comparing the mean difference of cortical thickness, labio-palatal bone thickness, and inter-radicular distance between the sites.
Table 5. Significance value obtained from ANOVA and Tukey post hoc tests comparing the mean difference of cortical thickness, labio-palatal bone thickness, and inter-radicular distance between the sites. In Press
05 Mar 2024 : Clinical Research
Role of Critical Shoulder Angle in Degenerative Type Rotator Cuff Tears: A Turkish Cohort StudyMed Sci Monit In Press; DOI: 10.12659/MSM.943703
06 Mar 2024 : Clinical Research
Comparison of Outcomes between Single-Level and Double-Level Corpectomy in Thoracolumbar Reconstruction: A ...Med Sci Monit In Press; DOI: 10.12659/MSM.943797
21 Mar 2024 : Meta-Analysis
Economic Evaluation of COVID-19 Screening Tests and Surveillance Strategies in Low-Income, Middle-Income, a...Med Sci Monit In Press; DOI: 10.12659/MSM.943863
10 Apr 2024 : Clinical Research
Predicting Acute Cardiovascular Complications in COVID-19: Insights from a Specialized Cardiac Referral Dep...Med Sci Monit In Press; DOI: 10.12659/MSM.942612
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952








