31 January 2023: Clinical Research
A Retrospective Study to Evaluate the Association Between the Glasgow Prognostic Score and Atrial Fibrillation, Stroke, and Mortality at 30 Days and at 1 Year After Coronary Artery Bypass Graft Surgery
Esra DönmezDOI: 10.12659/MSM.939283
Med Sci Monit 2023; 29:e939283
Abstract
BACKGROUND: The Glasgow prognostic score (GPS) consists of a combination of serum C-reactive protein and albumin levels as indicators of systematic inflammatory response and nutritional status, respectively. The present retrospective study aimed to evaluate the association between the GPS and atrial fibrillation, stroke, and mortality at 30 days and 1 year after coronary artery bypass graft (CABG) surgery.
MATERIAL AND METHODS: Patients with chronic coronary syndromes who underwent CABG surgery between 2012 and 2019 in a single center were included. Preoperative GPS was calculated. Then, patients were grouped according to postoperative atrial fibrillation (POAF) development. Further, groups were formed to evaluate the relationship between GPS and 30-day and 1-year cardiovascular mortality as well as stroke development.
RESULTS: Patients who developed POAF had higher GPS, higher European System for Cardiac Operative Risk Evaluation (EuroSCORE II) score, advanced age, lower angiotensin converting enzyme inhibitor/angiotensin receptor blocker (ACEI/ARB) use, lower left ventricular ejection fraction, and were more likely to be female and to have a history of carotid artery disease (P<0.05, for all). Additionally, GPS, EuroSCORE II, advanced age, and lower left ventricular ejection fraction were detected as independent risk factors for POAF development. When adverse outcomes were assessed, cardiovascular mortality at 30 days or 1 year, and stroke development at 1 year, were more frequent in patients with POAF. Moreover, POAF development was found to be an independent risk factor for adverse outcomes. Also, GPS was established as an independent risk factor both for 30-day and 1-year cardiovascular mortality (P<0.0001 and P=0.001, respectively).
CONCLUSIONS: GPS is an easy-to-calculate score that has reasonable diagnostic accuracy in determining the risk of POAF and stroke as well as 30-day and 1-year cardiovascular mortality.
Keywords: Atrial Fibrillation, Human Serum Albumin, Des-Leucyl(585)-, Cardiovascular Diseases, C-Reactive Protein (164-173), Prognosis, Humans, Female, Male, angiotensin receptor antagonists, Stroke Volume, Postoperative Complications, Angiotensin-Converting Enzyme Inhibitors, Ventricular Function, Left, Coronary Artery Bypass, Risk Factors, Stroke
Background
Postoperative atrial fibrillation (POAF) is among the most frequent complications of cardiac surgery. The incidence of POAF differs according to the type of surgery. It may develop in 15–40% of patients who undergo coronary artery bypass graft (CABG), while 33–49% of patients develop POAF after valvular surgery [1,2]. The 2 main arrhythmogenic mechanisms are re-entry and triggering activity, including perioperative inflammation, oxidative stress, pain, electrical remodeling, electrolyte disturbance, and ischemia [3–5]. Even though a number of episodes are asymptomatic and self-terminating, POAF is occasionally associated with myocardial infarction, stroke, and death [6]. Additionally, patients who develop POAF have a 4–5-fold increased risk of persistent atrial fibrillation (AF) in the 5 years following surgery [7].
The Glasgow prognostic score (GPS) is composed of C-reactive protein (CRP) and albumin levels, which are broadly used markers in clinical practice. CRP and albumin levels, as indicators of systematic inflammatory response and nutritional status, respectively, have been widely used for predicting oncological outcomes in various malignancies, for 2 decades [8]. In addition, studies have indicated that GPS can be used as a prognostic tool for determining survival after heart failure as well as predicting mortality in acute coronary syndromes [9,10]. Moreover, albumin has an antiplatelet effect by modulating arachidonic acid metabolism and a protective effect conferred by its antioxidant properties [11].
Although the pathophysiology of AF is well-defined, studies evaluating POAF are limited and not validated. Of note, POAF also poses a risk for AF development in the followup period [12]. POAF is thought to be triggered by perioperative inflammation, oxidative stress, pain, electrical remodeling, electrolyte disturbance, and ischemia [3–5]. These aforementioned factors facilitate myocardial vulnerability to AF development in the postoperative period. Arrhythmogenic remodeling due to comorbidities or transient triggering factors related to surgery may initiate POAF development involving pulmonary veins or ‘non-pulmonary’ vein regions. Thus, clinicians are seeking an easy way to calculate an accessible risk score based on everyday parameters for the purpose of predicting the development of POAF. To date, there have been several risk scoring systems like POAF, HATCH (hypertension, age, transient ischemic attack or stroke, chronic obstructive pulmonary disease, and heart failure), CHA2DS2-VASc [congestive heart failure, hypertension, age ≥75 (doubled), diabetes, stroke (doubled), vascular disease, age 65 to 74, and female sex] and COM-AF (age, heart failure, female sex, hypertension, diabetes, previous stroke) to help predict POAF development [13–16]. However, more research is still needed. Since chronic coronary syndrome is associated with chronic inflammation, and CABG surgery causes acute inflammation, inflammatory biomarkers may provide the inflammatory status of the patient and help to identify patients at risk. Our aim was to evaluate whether preoperative GPS can be used to reveal the risk of POAF development in CABG patients and to evaluate the effect of POAF on long-term cardiovascular morbidity and mortality. Therefore, this retrospective study aimed to evaluate the association between the GPS and AF, stroke, and mortality at 30 days and at 1 year after CABG surgery.
Material and Methods
STUDY POPULATION:
This study was approved by the local Human Studies and Research Committee (Number: 2021-75) and patient consent was waived due to the study’s retrospective nature. Patients diagnosed with chronic coronary syndromes who underwent CABG surgery at our institution between May 2012 and December 2019 were included in this retrospective study. Pre-, peri- and postoperative data were retrieved from the hospital database and patients’ files. Demographic, clinical, and laboratory parameters were noted and European System for Cardiac Operative Risk Evaluation (EuroSCORE II) was calculated for each patient. Patients were excluded from the study if they had the following: preoperative AF rhythm or atrial/ventricular arrhythmia, valvular cardiac disease, congenital heart disease, preoperative renal impairment (serum creatinine >2 mg/dl), albuminuria and chronic liver disease, albumin replacement therapy in past 6 months, malignancy, endocrinologic disorders (hypothyroidism, hyperthyroidism), systemic inflammatory diseases, hematologic diseases, low hemoglobin (Hb) levels (≤10 g/dL), left atrial enlargement (>4.5 cm on echocardiography), or previous diagnosis of an autoimmune disease. In addition, those who had undergone emergency operations (eg acute myocardial infarction) were also excluded. Finally, those with unavailable serum CRP or albumin levels were also excluded.
LABORATORY AND CLINICAL EVALUATION:
Preoperative CRP and albumin levels were used for GPS calculation (
An increased CRP level (>10 mg/L) or a low albumin level (<3.5 g/dL) were defined as 1 point each towards the GPS. The patient had a score of 0 if both parameters were normal, 1 if one parameter was abnormal, and 2 if both parameters were abnormal [17]. Patients with GPS=0 were accepted as ‘low GPS’ and those with GPS≥1 were accepted as ‘high GPS’. During the hospital stay, all patients were evaluated with daily 12-lead electrocardiography (ECG) and additional ECGs, which were obtained when the patient reported a symptom or a rhythm abnormality was suspected during telemetry monitoring to identify rhythm abnormalities or AF development. Clinical AF was diagnosed when standard 12-lead ECG recording or a single-lead ECG tracing of ≥30 s showed heart rhythm with no discernible repeating P waves and irregular RR intervals (when atrioventricular conduction was not impaired) [2,18]. POAF was defined as an episode of AF requiring treatment after surgery that developed during hospitalization. Cardiovascular mortality was defined as death due to myocardial or cerebrovascular disease. The development of stroke requiring hospitalization after discharge and 1-year cardiovascular mortality data were obtained by using local hospital and national electronic databases. Patients were grouped according to POAF development, occurrence of 30-day and 1-year cardiovascular mortality, and stroke in the 1-year followup.
STATISTICAL ANALYSIS:
All statistical tests were conducted using the Statistical Package for the Social Sciences 22.0 for Windows (SPSS Inc., Chicago, IL, USA). The Kolmogorov-Smirnov test was used to analyze normality of the data. Continuous data are expressed as mean±standard deviation, and categorical data are expressed as percentages. Chi-square test was used to assess differences in categorical variables between groups. Either the
Results
DEMOGRAPHIC FINDINGS:
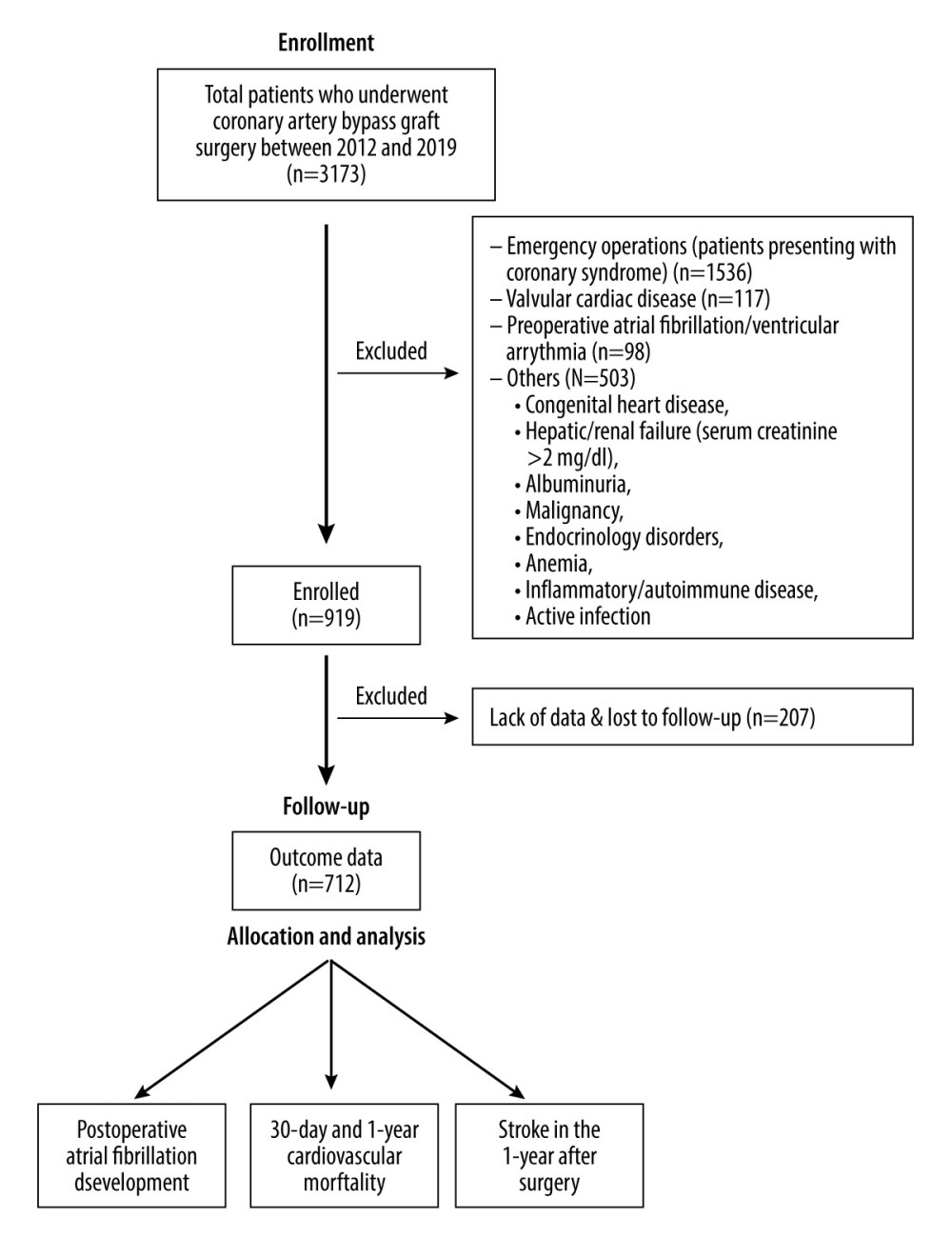
A total of 3173 patients who underwent CABG surgery between May 2012 and December 2019 were screened. After exclusion, 712 patients were included in this retrospective single-center study (Figure 1). The mean age of the cohort was 60.3±9.72 years and 75.9% of the patients were male. There were 473 (66.4%) patients in the low-GPS group (GPS=0) and 239 (33.6%) patients in the high-GPS group (GPS≥1). Forty (5.6%) patients died within 30 days and 76 (10.7%) patients died within 1 year after surgery. Stroke occurred in 26 (3.7%) patients during the 1-year followup, excluding early postoperative stroke cases. Table 1 provides an overview of the demographic, laboratory, and clinical data.
POSTOPERATIVE ATRIAL FIBRILLATION:
POAF occurred in 121 (17%) patients at a median of 2 days after the operation. The patients with POAF were older (63.3±8.7 vs 59.6±9.8; P<0.0001) and 84.8% of the patients were female (P=0.05). Also, POAF developed in patients who had a significantly higher prevalence of carotid artery disease (27.3% vs 4.4%; P<0.0001). Furthermore, EuroSCORE II (2.27±1.68 vs 1.89±1.13; P=0.02) was significantly higher while Hb (12.0±1.5 vs 12.5±1.8; P=0.012), Htc (37.8±4.7 vs 39.4±4.8; P=0.001), and left ventricular ejection fraction (49.2±8.7 vs 51.2±8.7; P=0.018) were significantly lower in patients with POAF. In terms of preoperative medications, statins and b-blockers did not differ between groups. However, angiotensin converting enzyme inhibitors/angiotensin receptor blockers (ACEI/ARB) use was less common in the POAF group (38.6% vs 51.2%; P=0.048). Ultimately, POAF developed more frequently in patients with higher GPS. Specifically, within the group of patients who developed POAF, GPS=0 was found in 56 patients (46.3%) and GPS≥1 in 65 patients (53.7%) (P<0.0001). Table 1 provides data regarding the variables and their associations with POAF development.
CARDIOVASCULAR MORTALITY AND STROKE:
The patients’ followup data were analyzed to define factors related to stroke and 30-day and 1-year cardiovascular mortality. When patients were grouped according to 30-day cardiovascular mortality, the following were statistically higher in the 30-day cardiovascular mortality group: advanced age (63.5±11.1 vs 60.1±9.6; P=0.031), EuroSCORE II (3.3±1.3 vs 1.9±1.1; P<0.0001), high GPS (65% vs 31.7%; P<0.0001), history of chronic obstructive pulmonary disease (COPD) (37.5% vs 17.8%; P=0.042), history of carotid artery disease (22.5% vs 7.5%; P=0.004), and POAF (37.5% vs 15.8%; P<0.0001). The parameters that were significantly higher in the 1-year cardiovascular mortality group were similar to those in the 30-day cardiovascular mortality group: advanced age (62.4±10.5 vs 59.9±9.6; P=0.041), EuroSCORE II (3.7±1.5 vs 1.8±1.02; P<0.0001), history of carotid artery disease (26.3% vs 6.1%; P<0.0001), and high GPS (59.2% vs 30.5%; P<0.0001). In addition, stroke (22.4% vs 1.4%; P<0.0001) and POAF development (44.7% vs 13.7%; P<0.0001) were more common in the 1-year cardiovascular mortality group. Tables 2 and 3 provide data regarding the association of the variables with 30-day and 1-year cardiovascular mortality, respectively.
The patients who developed stroke during the 1-year followup period had significantly higher values for the following: EuroSCORE II (3.6±2.2 vs 1.9±1.2; P<0.0001), GPS (76.9% vs 31.9%; P<0.0001), history of cerebrovascular accident (CVA) (42.3% vs 2.1%; P=0.004), and carotid artery disease (92.3% vs 5.2%; P<0.0001). Also, 1-year cardiovascular mortality (65.4% vs 8.6%; P<0.0001) and POAF development (88.5% vs 14.3%; P<0.0001) were higher in the patients who developed stroke (Table 4).
LOGISTIC REGRESSION ANALYSIS:
To further evaluate individual risk factors for POAF development, 30-day and 1-year cardiovascular mortality, and stroke development, univariate logistic regression analyses were performed. The variables that were statistically significant in univariate logistic regression analyses were additionally evaluated by multivariate logistic regression analysis to define independent risk factors for outcomes. In multivariate logistic regression analyses, GPS [
Furthermore, high GPS [
Last but not least, EuroSCORE II [
Discussion
POAF is considered an important complication following CABG, and it is crucial to predict its occurrence as it has both short- and long-term consequences. The results of our study indicated that high GPS, high EuroSCORE II, advanced age, female gender, history of carotid artery disease, lower ACEI/ARB use, and lower left ventricular ejection fraction were seen in patients who developed POAF. In addition, high GPS, EuroSCORE II, advanced age, and lower left ventricular ejection fraction were shown to be independent risk factors associated with POAF development. With regard to adverse events, cardiovascular mortality either within 30 days or 1 year, and stroke development within 1 year following the surgery were more frequent in patients who developed POAF. Moreover, POAF development was found to be an independent risk factor for adverse outcomes, and GPS was established as an independent risk factor both for 30-day and 1-year cardiovascular mortality, even in patients with chronic coronary syndromes.
The most common type of arrhythmia after CABG is POAF, which may be observed in up to 40% of patients [19]. A history of AF, older age, obesity, presence of valvular and rheumatic heart disease, impaired left ventricular systolic function, left atrial enlargement, previous myocardial infarction, hypertension (HT), diabetes mellitus (DM), COPD, presence of metabolic syndrome, coronary ischemia, and hypoxemia are known risk factors for POAF [20]. Preoperative conditions such as clinical presentation and comorbidities, related surgery, and perioperative complications are the facilitator factors that make the myocardium vulnerable to AF development in the postoperative period. Re-entery and triggered activity are known to be the 2 main arrhythmogenic mechanisms. Arrhythmogenic remodeling due to comorbidities or transient triggering factors related to the surgery may initiate POAF development involving pulmonary veins or ‘non-pulmonary’ vein regions. Including all these parameters to obtain a risk score to predict the development of POAF would be extremely time consuming. On the other hand, the role of inflammation and related biomarkers have already been studied and inflammation has been established as a pathological mechanism for AF development [21,22]. Our study’s analysis of serum CRP, a marker of acute inflammation, showed that increased age, female sex, reduced ejection fraction, and lower preoperative hemoglobin and hematocrit levels were associated with POAF development in concordance with previously stated risk factors.
CRP is an acute-phase reactant and a well-known marker of systemic inflammation. Not only surgery, but also most of the coronary artery disease risk factors, as well as coronary artery disease itself, may cause increased CRP levels. The association between higher baseline CRP level and POAF was revealed in a meta-analysis which considered high CRP as a positive predictor [22]. Similarly, in our study, CRP levels were higher in the patients who developed POAF.
Serum albumin levels represent nutritional status, but they are also known as a negative acute-phase reactant (decreasing levels with increasing inflammation). Moreover, as stated before, albumin exerts antiplatelet effects through modulation of arachidonic acid metabolism and a protective effect through antioxidant properties [11]. The relationship between hypoalbuminemia and acute coronary syndromes, cardiovascular ischemic disease, and stroke was reported previously [23,24]. In contrast to the consensus in the literature, there were no significant differences in albumin levels between groups in our study. However, it should be noted that the exclusion of patients with acute or chronic inflammatory conditions and those with disorders related to the loss of or impaired production of albumin may be the reasons for similar albumin levels in our study.
GPS consists of CRP and albumin concentrations and is among the validated inflammatory risk scores for cancer patients [8]. Moreover, it has been studied in different cardiac disorders and shown to be a prognostic tool for determining survival after heart failure as well as cardiovascular mortality in acute coronary syndromes [9,10]. Concerning the influence of CRP and albumin on POAF development, higher GPS values were found to be associated with POAF development. Our results emphasize the importance and utility of this scoring system (GPS), rather than biomarkers individually (CRP and albumin), for the anticipation of POAF development in patients who have undergone CABG surgery with a diagnosis of chronic coronary syndrome. High GPS was displayed as an independent risk factor for POAF development; moreover, it was an independent predictor of 30-day and 1-year cardiovascular mortality. Furthermore, high GPS was significantly related to stroke development in the POAF group during the 1-year followup period, although it was not found to be an independent predictor.
POAF is an important phenomenon related to myocardial infarction, stroke, and even death [6]. Besides, patients with POAF have increased risk of persistent AF in the first 5 years after CABG [7]; thus, it is crucial to define patients who are at high risk. We demonstrated the relation between POAF and 30-day and 1-year cardiovascular mortality, as well as stroke development in the 1-year followup period. POAF was also found to be an independent risk factor for cardiovascular mortality and stroke development within 1 year after surgery. Since high GPS was found to be an independent predictor of POAF development and 30-day and 1-year mortality, effective responses to preoperative conditions, including inflammation and nutritional status of the patient, may improve outcomes by decreasing POAF development.
There are several limitations of our study. Firstly, although the cohort was large, the study population remained low, mostly due to strict exclusion criteria (patients with disease that might have altered serum CRP and/or albumin levels). Moreover, all pitfalls of retrospective studies are relevant to our study. Further, information on preoperative medications (b-blockers, statins, ACEI/ARB), such as doses and length of treatment, might have influenced the results. Baseline CRP and albumin levels were used in the study whereas monitoring the changes in serum levels throughout the course of hospitalization may reveal additive knowledge. Also, our data is limited to in-hospital detection of POAF, whereas a longer duration would give better diagnostic ability. The patients were revascularized with arterial (mostly left internal mammalian artery) and venous (saphenous vein) conduits in our center. Thus, a comparison could not be made in terms of the graft effect on POAF development. Future studies comparing complete arterial revascularization CABG with CABG including venous conduits may give additional valuable information. Last but not least, this study was not designed to evaluate short- or long-term treatment of POAF. However, the guideline-directed anti-arrhythmic and anticoagulant therapy, either for short- or long-term periods, is essential to reduce mortality and morbidity.
Conclusions
GPS is an easy-to-use and rapidly measured score with widely available tools for calculation. In addition, it has reasonable diagnostic accuracy in determining POAF and stroke development as well as 30-day and 1-year cardiovascular mortality. Since POAF is related to mortality and stroke, GPS may help to predict patients who are at risk with minimal effort. Further prospective studies with larger patient cohorts and longer followup periods are needed to improve the clinical utility of GPS.
Tables
Table 1. Comparison of demographic and laboratory parameters and outcomes of groups with regard to postoperative atrial fibrillation development.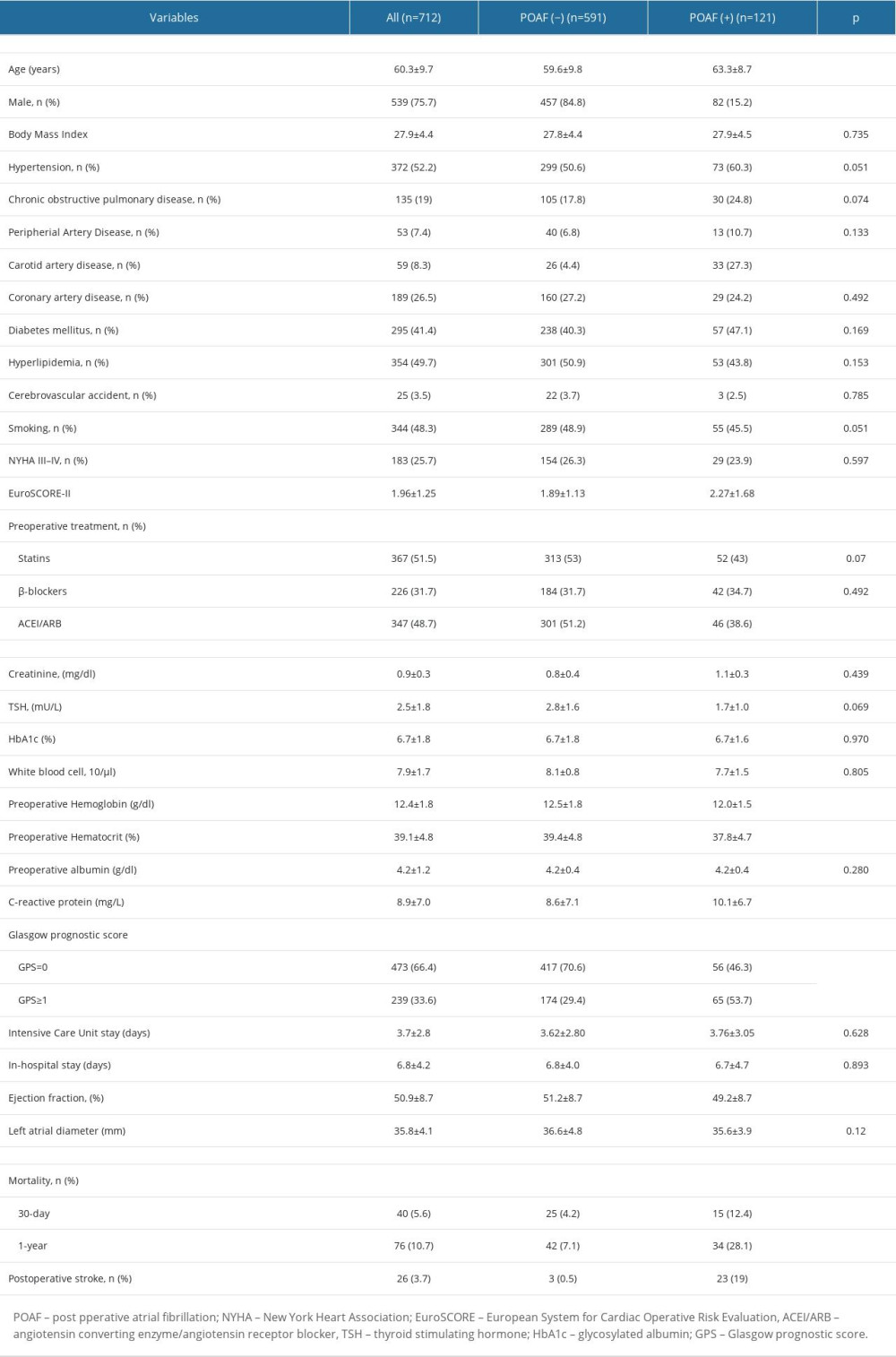 Table 2. Comparison of demographic, laboratory, and clinical parameters with respect to 30-day cardiovascular mortality.
Table 2. Comparison of demographic, laboratory, and clinical parameters with respect to 30-day cardiovascular mortality.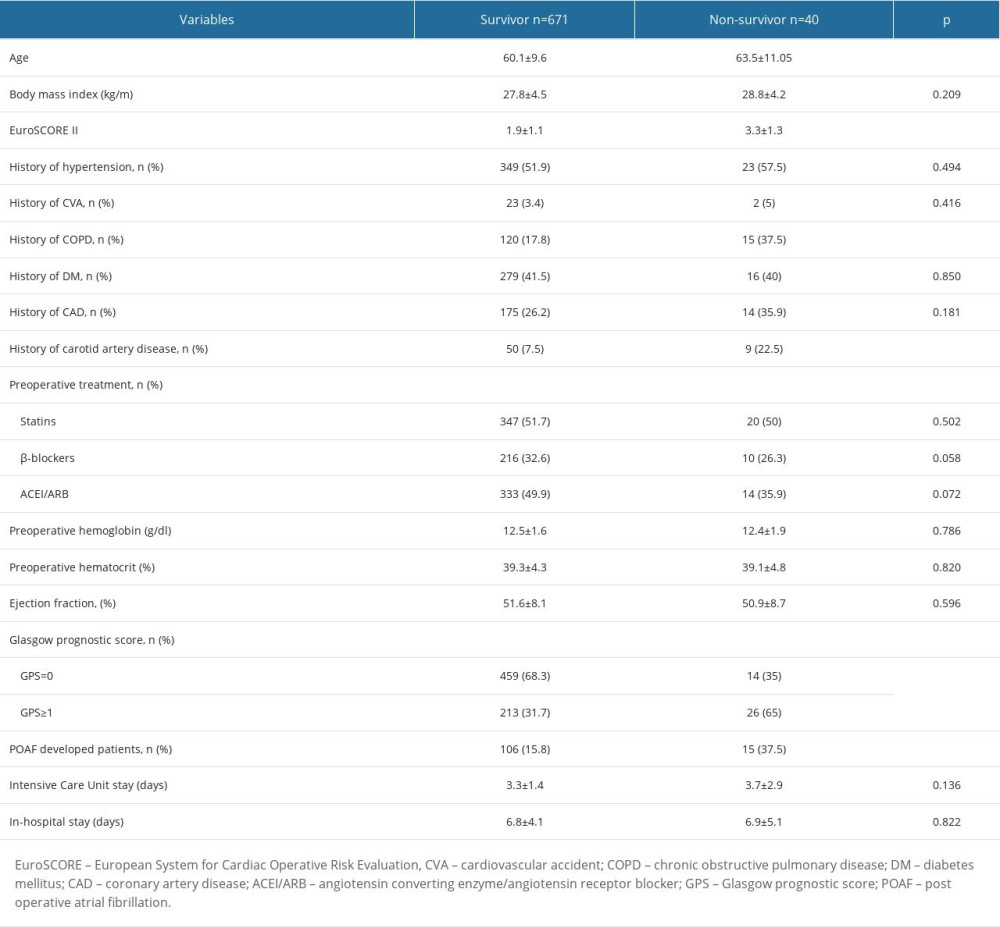 Table 3. Comparison of demographic, laboratory, and clinical parameters with respect to 1-year cardiovascular mortality.
Table 3. Comparison of demographic, laboratory, and clinical parameters with respect to 1-year cardiovascular mortality.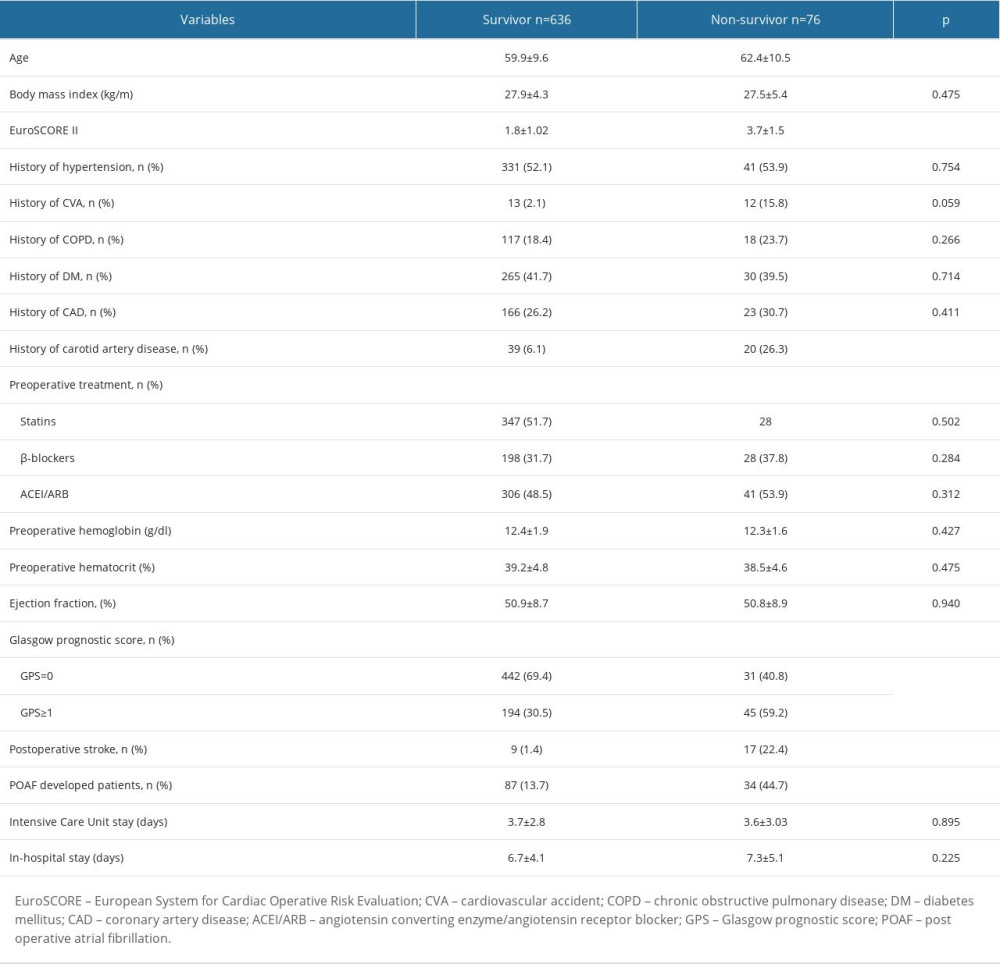 Table 4. Comparison of demographic, laboratory, and clinical parameters with respect to stroke development in the 1-year followup period.
Table 4. Comparison of demographic, laboratory, and clinical parameters with respect to stroke development in the 1-year followup period.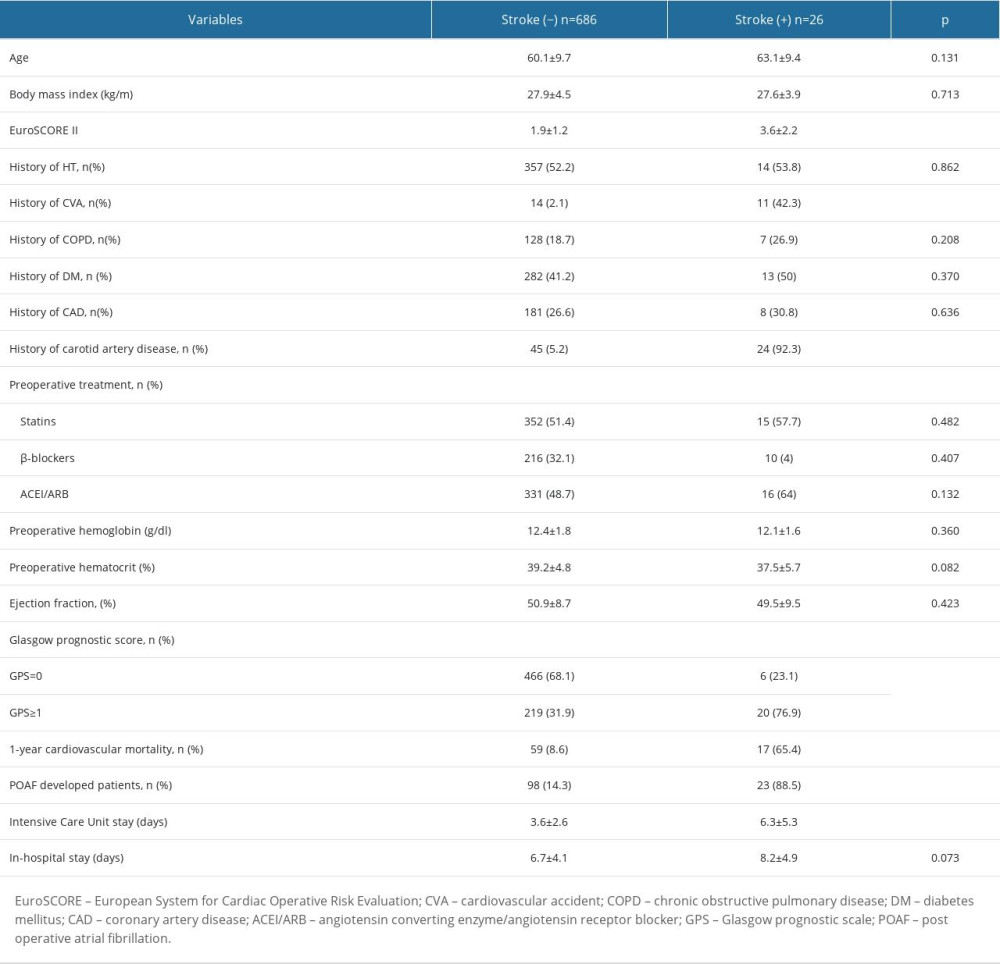
References
1. Gillinov AM, Bagiella E, Moskowitz AJ, Rate control versus rhythm control for atrial fibrillation after cardiac surgery: N Engl J Med, 2016; 374(20); 1911-21
2. Hindricks G, Potpara T, Dagres N, 2020 ESC Guidelines for the diagnosis and management of atrial fibrillation developed in collaboration with the European Association for Cardio-Thoracic Surgery (EACTS):The Task Force for the diagnosis and management of atrial fibrillation of the European Society of Cardiology (ESC) Developed with the special contribution of the European Heart Rhythm Association (EHRA) of the ESC: Eur Heart J, 2021; 42(5); 373-498
3. Mostafa A, El-Haddad MA, Shenoy M, Tuliani T, Atrial fibrillation post cardiac bypass surgery: Avicenna J Med, 2012; 2(3); 65-70
4. Oral H, Post-operative atrial fibrillation and oxidative stress:A novel causal mechanism or another biochemical epiphenomenon?: J Am Coll Cardiol, 2008; 51(1); 75-76
5. Greenberg JW, Lancaster TS, Schuessler RB, Melby SJ, Postoperative atrial fibrillation following cardiac surgery:A persistent complication: Eur J Cardiothorac Surg, 2017; 52(4); 665-72
6. Sahin I, Ozkaynak B, Karabulut A, Impact of coronary collateral circulation and severity of coronary artery disease in the development of postoperative atrial fibrillation: Interact Cardiovasc Thorac Surg, 2014; 19(3); 394-97
7. Konstantino Y, Zelnik Yovel D, Friger MD, Postoperative atrial fibrillation following coronary artery bypass graft surgery predicts long-term atrial fibrillation and stroke: Isr Med Assoc J, 2016; 18(12); 744-48
8. Roxburgh CS, McMillan DC, Role of systemic inflammatory response in predicting survival in patients with primary operable cancer: Future Oncol, 2010; 6(1); 149-63
9. Jia Y, Li D, Cao Y, Inflammation-based Glasgow prognostic score in patients with acute ST-segment elevation myocardial infarction:A prospective cohort study: Medicine (Baltimore), 2018; 97(50); e13615
10. Cho A, Arfsten H, Goliasch G, The inflammation-based modified Glasgow prognostic score is associated with survival in stable heart failure patients: ESC Heart Fail, 2020; 7(2); 654-62
11. Purdon AD, Rao AK, Interaction of albumin, arachidonic acid and prostanoids in platelets: Prostaglandins Leukot Essent Fatty Acids, 1989; 35(4); 213-18
12. Thoren E, Wernroth ML, Christersson C, Compared with matched controls, patients with postoperative atrial fibrillation (POAF) have increased long-term AF after CABG, and POAF is further associated with increased ischemic stroke, heart failure and mortality even after adjustment for AF: Clin Res Cardiol, 2020; 109(10); 1232-42
13. Mariscalco G, Biancari F, Zanobini M, Bedside tool for predicting the risk of postoperative atrial fibrillation after cardiac surgery:The POAF score: J Am Heart Assoc, 2014; 3(2); e000752
14. de Vos CB, Pisters R, Nieuwlaat R, Progression from paroxysmal to persistent atrial fibrillation clinical correlates and prognosis: J Am Coll Cardiol, 2010; 55(8); 725-31
15. Chua SK, Shyu KG, Lu MJ, Clinical utility of CHADS2 and CHA2DS2-VASc scoring systems for predicting postoperative atrial fibrillation after cardiac surgery: J Thorac Cardiovasc Surg, 2013; 146(4); 919-26e1
16. Burgos LM, Ramirez AG, Seoane L, New combined risk score to predict atrial fibrillation after cardiac surgery:COM-AF: Ann Card Anaesth, 2021; 24(4); 458-63
17. Forrest LM, McMillan DC, McArdle CS, Evaluation of cumulative prognostic scores based on the systemic inflammatory response in patients with inoperable non-small-cell lung cancer: Br J Cancer, 2003; 89(6); 1028-30
18. Steinberg JS, O’Connell H, Li S, Ziegler PD, Thirty-second gold standard definition of atrial fibrillation and its relationship with subsequent arrhythmia patterns:Analysis of a large prospective device database: Circ Arrhythm Electrophysiol, 2018; 11(7); e006274
19. Yang E, Spragg D, Schulman S, Rate versus rhythm control in heart failure patients with post-operative atrial fibrillation after cardiac surgery: J Card Fail, 2021; 27(8); 915-19
20. Yamashita K, Hu N, Ranjan R, Clinical risk factors for postoperative atrial fibrillation among patients after cardiac surgery: Thorac Cardiovasc Surg, 2019; 67(2); 107-16
21. Li XY, Hou HT, Chen HX, Preoperative plasma biomarkers associated with atrial fibrillation after coronary artery bypass surgery: J Thorac Cardiovasc Surg, 2021; 162(3); 851-63e3
22. Weymann A, Popov AF, Sabashnikov A, Baseline and postoperative levels of C-reactive protein and interleukins as inflammatory predictors of atrial fibrillation following cardiac surgery:A systematic review and meta-analysis: Kardiol Pol, 2018; 76(2); 440-51
23. Zhu L, Chen M, Lin X, Serum albumin level for prediction of all-cause mortality in acute coronary syndrome patients: A meta-analysis: Biosci Rep, 2020; 40(1); BSR20190881
24. Xia M, Zhang C, Gu J, Impact of serum albumin levels on long-term all-cause, cardiovascular, and cardiac mortality in patients with first-onset acute myocardial infarction: Clin Chim Acta, 2018; 477; 89-93
Tables
 Table 1. Comparison of demographic and laboratory parameters and outcomes of groups with regard to postoperative atrial fibrillation development.
Table 1. Comparison of demographic and laboratory parameters and outcomes of groups with regard to postoperative atrial fibrillation development. Table 2. Comparison of demographic, laboratory, and clinical parameters with respect to 30-day cardiovascular mortality.
Table 2. Comparison of demographic, laboratory, and clinical parameters with respect to 30-day cardiovascular mortality. Table 3. Comparison of demographic, laboratory, and clinical parameters with respect to 1-year cardiovascular mortality.
Table 3. Comparison of demographic, laboratory, and clinical parameters with respect to 1-year cardiovascular mortality. Table 4. Comparison of demographic, laboratory, and clinical parameters with respect to stroke development in the 1-year followup period.
Table 4. Comparison of demographic, laboratory, and clinical parameters with respect to stroke development in the 1-year followup period. Table 1. Comparison of demographic and laboratory parameters and outcomes of groups with regard to postoperative atrial fibrillation development.
Table 1. Comparison of demographic and laboratory parameters and outcomes of groups with regard to postoperative atrial fibrillation development. Table 2. Comparison of demographic, laboratory, and clinical parameters with respect to 30-day cardiovascular mortality.
Table 2. Comparison of demographic, laboratory, and clinical parameters with respect to 30-day cardiovascular mortality. Table 3. Comparison of demographic, laboratory, and clinical parameters with respect to 1-year cardiovascular mortality.
Table 3. Comparison of demographic, laboratory, and clinical parameters with respect to 1-year cardiovascular mortality. Table 4. Comparison of demographic, laboratory, and clinical parameters with respect to stroke development in the 1-year followup period.
Table 4. Comparison of demographic, laboratory, and clinical parameters with respect to stroke development in the 1-year followup period. In Press
08 Mar 2024 : Clinical Research
Evaluation of Foot Structure in Preschool Children Based on Body MassMed Sci Monit In Press; DOI: 10.12659/MSM.943765
15 Apr 2024 : Laboratory Research
The Role of Copper-Induced M2 Macrophage Polarization in Protecting Cartilage Matrix in OsteoarthritisMed Sci Monit In Press; DOI: 10.12659/MSM.943738
07 Mar 2024 : Clinical Research
Knowledge of and Attitudes Toward Clinical Trials: A Questionnaire-Based Study of 179 Male Third- and Fourt...Med Sci Monit In Press; DOI: 10.12659/MSM.943468
08 Mar 2024 : Animal Research
Modification of Experimental Model of Necrotizing Enterocolitis (NEC) in Rat Pups by Single Exposure to Hyp...Med Sci Monit In Press; DOI: 10.12659/MSM.943443
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952