21 September 2022: Clinical Research
Dental Health and Quality of Life in 117 Patients from Kosovo, Aged 6–80 Years, Evaluated Using the Dental Impact on Daily Living (DIDL) Questionnaire and the Oral Health-Related Quality of Life (OHRQoL) Questionnaire
Fehim Haliti1BCDE, Sinan Rusinovci2AD*, Dion Haliti3BCD, Dea Haliti3BCDF, Jonila Rusinovci4BF, Elena Hajdari3BCDF, Tomislav Jukic5CE, David Stubljar6ACEDOI: 10.12659/MSM.938072
Med Sci Monit 2022; 28:e938072
Abstract
BACKGROUND: This study aimed to evaluate the effects of dental health on quality of life (QoL) in 117 patients from Kosova, aged 6-80 years, using the Dental Impact on Daily Living (DL) questionnaire and the Oral Health-Related Quality of Life (OHRQoL) questionnaire.
MATERIAL AND METHODS: We recruited 117 patients, approximately half male and half female, aged 6-80 years. The subjects came for dental appointments and filled out 2 questionnaires: DIDL addressing questions on appearance, comfort, pain, performance and eating restriction, and OHRQoL assessing dental-specific questions for evaluation of satisfaction with oral health, and evaluation of importance they attribute to oral health. Collected data included age, gender, income, education level, and frequency of brushing teeth per day.
RESULTS: The participants were relatively satisfied with their DIDL health (score >0) and also had positive views on OHRQoL (score >0). No participants evaluated the appearance, comfort, eating restrictions, or pain as satisfactory. Comparisons of age, gender, education, income level, and frequency of brushing teeth showed that female participants evaluated their DIDL higher than male participants (P=0.043). Age was correlated with the frequency of teeth brushing per day (rho=-0.450; P<0.001). Gender, age, education level, income level, and frequency of teeth brushing did not influence QoL.
CONCLUSIONS: This small study from Kosovo showed reasonable satisfaction with oral health and its associated QoL. While participants reported good effects of oral health on their QoL, they were least satisfied with comfort and most satisfied with their performance.
Keywords: Oral Health, Oral Hygiene, Quality of Life, Surveys and Questionnaires, Female, Humans, Kosovo, Male, Pain
Background
Assessing oral health and thus quality of life (QoL) is becoming more important. Oral conditions influence the social, economic, and psychological aspect of life and impact the QoL of individuals [1]. In the past, studies have investigated the social impact of dental diseases on people’s daily life [2]. Assessing the QoL related to oral health and dental impact on daily living has led to creation of several questionnaires [3].
The Oral Health Quality of Life (OH-QoL) questionnaire is a self-reported questionnaire that includes social, functional, and psychological items [4]. These items reflect respondents’ self-esteem and satisfaction with and importance of oral health when eating, sleeping, and during social interaction [5,6]. As the responses might be subjective, it is necessary to take into consideration the current emotional state of the patients at the time of the survey, as even patients with severe oral conditions can report good QoL. Furthermore, QoL is by itself multi-faceted, showing variation over time for each individual [7]. For instance, loss of teeth causes a person aesthetic and functional problems and lowers the QoL. Socioeconomic status frequently influences tooth loss, as it is associated to inequalities in healthcare or access to healthcare [8]. Moreover, caries has negative impacts on OH-QoL across all population [9]. For instance, children with caries scored about 50% higher on QoL than children without caries [10].
The Dental Impact on Daily Living (DIDL) survey was created by Leao and Sheiham [11]. It involves questions about appearance, comfort, performance pain, and eating restrictions and gives insight into how a broad spectrum of life compares to clinical status and oral hygiene [3]. DIDL differentiates dimensions on the subjective impact from the responders and also identifies the influence of social class and gender [12]. It was firstly tested in Brazil on 662 people, aged 35–44 years, coming from 2 different social-economic classes, and with different levels of dental caries. The questionnaire was validated as reliable. Levels of oral status were shown to affect people’s daily life. The authors also found that social and psychological dimensions were important and need to be considered when assessing dental needs [12].
Another reliable measure is the Oral Health-Related Quality of Life (OHRQoL) questionnaire, which was developed by Cornell University and can be used as a whole or as the part of the questionnaire including 4 domains: self-rated oral health, objectively-assessed oral health, nutrition, and QoL [13]. OHRQoL can measure treatment needs and efficacy of care. Scores show the relationship between oral health and general health and demonstrate that improving the patient’s QoL goes beyond just treatments [14]. Many instruments have been developed to measure QoL, but OHRQoL is one of the most largely investigated and widely used [14].
Patient-reported outcomes (PROs) are fundamental evidence-based data not only in dentistry, but in the whole medical community, and are essential to increase research and understandings of what is important during the treatment and in oral healthcare. The increasing importance of oral health led to investigating the relationship between oral health and QoL. Therefore, this study aimed to evaluate the effects of dental health on quality of life in 117 patients from Kosovo, aged 6–80 years, using the DIDL questionnaire and the OHRQoL questionnaire.
Material and Methods
STUDY DESIGN:
Our Institutional Ethics Committee approved the study on 19/05/2022 with protocol number 247. Adult participants and children and their parents were informed about the study and asked to participate. They gave written consent agreement for inclusion into the study. Those who accepted filled out the questionnaires or were interviewed by the interviewer. Participation in the surveys was voluntary, the data and the results were used only for research purposes. The questionnaires were anonymous.
The study was carried out among patients coming for dental appointments in 2022 to the Department of Dentistry of University Dentistry Clinical Centre of Kosovo due to various minor dental problems and were asked to participate. A total of 117 patients, aged from 6 to 80 years, participated in this research.
ROLL-OUT OF QUESTIONNAIRE SURVEY:
The interviewer recorded the answers from respondents. The questionnaires and the scale were shown to the respondents before interviewing people. Two already-established questionnaires were used in the study.
The first questionnaire comprised 36 questions measuring oral health from the Dental Impact on Daily Living (DIDL) instrument and was originally developed by Leao and Sheiham [11]. The questions included 5 different dimensions:
The scores were evaluated according to the response on the impact as +1=positive, 0=neutral, −=negative. The scores of each dimension were summarized and divided by the number of questions within each dimension. Thus, an average score of respective dimensions was obtained. Each dimension was then weighted by importance. In our case, we decided that dimension should be equally weighted, meaning that each dimension was weighted as 0.20. A final DIDL total score ranged from 10 to −10 and was calculated according to the equation=(0.2×Appearance dimension score) + (0.2×Pain dimension score) + (0.2×Comfort dimension score) + (0.2×Performance dimension score) + (0.2× Eating Restriction dimension score). The DIDL responses were then grouped into 3 response categories: (i) not at all satisfied (scores <0), (ii) relatively satisfied (scores 0–7), and (iii) very much satisfied (scores >7).
The second questionnaire used was Oral Health Quality of Life (OH-QoL), created by Cornell et al [13]. We used only a part of the questionnaire for assessing dental-specific questions for evaluation of satisfaction with oral health, and evaluation of importance attributed to oral health and functional status. Thus, 2 dimensions were assessed: Importance as not at all important (0), somewhat important (+1), or very important (+2), while Satisfaction was coded as unhappy (−2), somewhat unhappy (−1), somewhat happy (+1), or happy (+2). The total score is the mean value of the answered OH-QoL items; thus, yielding an interval level measure that ranges from a −4 to +4.
STATISTICAL ANALYSIS:
Statistical analyses were performed using SPSS version 21 (IBM, New York, USA). The one-way analysis of variance (one-way ANOVA) or
Results
A total of 117 patients who came for dental appointment participated in the study. Basic characteristic of all participants and their total scores of DIDL and OH-QoL are presented in Table 1. Participants were relatively young, with a mean age of approximately 29 years. There were approximately the same proportion of male and female participants, with a wide range of educational levels. Income levels were distributed into 3 groups, as was the frequency of brushing the teeth per day.
On average the participants were relatively satisfied with their dental impact on daily living health (DIDL score more than 0) and also had positive views on oral health-related quality of life (score above 0).
Analysis of responses from DIDL showed that most participants were relatively satisfied with all 5 dimensions (Table 2), but some were unsatisfied. No participants evaluated the appearance, comfort, eating restrictions, and pain as satisfactory.
Comparisons of independent variables (age, gender, education level, income level, frequency of brushing teeth) that can influence oral health and quality of life as dependable variables showed that only gender was significantly different when comparing total scores of DIDL. Female participants evaluated their DIDL higher that male participants (Table 3).
Linear regression predictions confirmed the impact of gender on DIDL scores, but other independent variables (age, education level, income level, and frequency of brushing teeth) were not significantly associated with scores of DIDL or OH-QoL (Tables 4, 5).
Pearson’s correlation analysis showed some statistical correlations. Age was correlated with the frequency of brushing per day (rho=−0.450;
Discussion
The increasing importance of oral health and inclusion of PROs in assessment of treatment success led us to investigate the relationship between oral health and QoL. Therefore, the aim of the current study was to evaluate the effects of dental health on QoL in patients from Kosovo, using the DIDL and the OHRQoL questionnaires. To the best of our knowledge, this is the first such study in Kosovo, and thus is a first attempt to provide the insights into how people perceive their oral health and how these influence their QoL. In terms of satisfaction, more than half of the participants were relatively satisfied with their dental impact on daily living and health. Similar results were obtained by Kumar et al [3], showing that the great majority of patients were also relatively satisfied with all dimensions and overall obtained by DIDL, also according to the total score. Oral health is known to affect QoL. The impact of oral health is based on the perception of an individual [1]. There might be also an impact of social class. For instance, in the current study, income level was correlated with education level and the frequency of brushing per day. Those who were highly educated and had higher income level brushed their teeth more frequently per day (rho=0.221;
The outcomes of oral diseases influence the wellbeing and QoL of individuals. Therefore, OH-QoL assesses self-perception of how oral health influences life quality and wellbeing [16]. Numerous questionnaires have been developed to measure OH-QoL. Studies show that OH-QoL is very much associated with age, gender, and socioeconomic factors [17]. People perceive their teeth to be important for their appearance and self-esteem [18,19]. This increase of interest in and importance of oral health led to investigating the self-evaluation of oral health, quality of life, and exploring the possible correlation between these 2 parameters in our population from Kosovo. The aim of DIDL is to obtain scores for 5 different dimensions and to finalize it with 1 total score. The total score gives a view of the individual, and generates personal importance for dimensions. Some feel more importance of appearance and other respondents might feel more importance of comfort. Therefore, the dimensions are directly associated with the perception of QoL, and its impact can vary from respondent to respondent. However, in our study the dimensions were weighted with the same power of 0.2 for the data to be more comparable within the respective dimensions. Moreover, DIDL includes many questions and therefore provides high-reliability data [11]. Thus, in conjunction it was an ideal questionnaire to be used in our analysis. The second questionnaire was OHRQoL, which assesses subjective wellbeing with respect to person’s oral health and functional status on QoL within 2 dimensions – importance and satisfaction. Wellbeing is subjective, and functional status is objectively measured. OHRQoL has high consistency and validity, and self-assessment of importance and satisfaction dimensions may also explain some clinical situations, such as patient dissatisfaction with dental care, and patient compliance with oral hygiene and treatment [20]. All these questionnaires were developed to measure the impact of oral health on QoL and could potentially be valuable tools for assessment and promotion of oral health initiatives [21].
According to the analysis, patients who came for dental appointment were relatively young, with a mean age of approximately 29 years, with approximately the same proportion of male and female participants, defining a good sample from the general population from Kosovo. Most of the study participants had secondary and university education. Apparently, also according to Okunseri et al [16], there is difficult enrolling participants with primary education only who are willing to participate in such oral health surveys. The reasons for the high numbers of secondary or university-educated participants could be that people with higher education are more informed about oral health and therefore are more likely to and more frequently seek dental treatments. But in our study, we did not investigate the reasons for their appointment, so we cannot conclude that from our analysis. Additionally, highly educated persons are also better able to afford dental services, have better access to dental care, and have better oral health habits when compared to less educated people. This evidence also confirms the relatively satisfied results of our participants with their dental impact on daily living health (DIDL score more than 0) and a positive view on OHRQoL (score above 0). Accurate analysis of responses from DIDL showed that most participants confirmed that they were relatively satisfied with all 5 dimensions. Moreover, correlation was found with education level (rho=0.221;
Studies found that females are commonly more concerned about dental appearance than males [12,23–25]. The same was demonstrated in our case. Independent variable such as age, gender, education level, income level, and frequency of brushing teeth can influence oral health and consequently the quality of life, but only gender was statistically significant when comparing total scores of DIDL. Female participants evaluated their DIDL higher than male participants, meaning they had higher satisfaction with their QoL and they spend more energy on oral health. Previous studies found no significant difference related to dimensions within DIDL, which agrees with our study. However, Leao and Sheiham found slightly more dissatisfaction in females (2.4%) than in males (0.8%) [12].
The same scenario was noted with use of the OHRQoL questionnaire, where participants were also satisfied with their oral health and QoL. However, we found a negative correlation between DIDL score and OHRQoL score (rho=−0.232;
Although we did not find any statistical correlation between the oral hygiene (more frequent brushing of the teeth) and QoL, we saw a negative association with DIDL and OHRQoL scores after performing linear regression. Oral hygiene had no correlations with the dimensions of Appearance, Pain, or Performance, but it showed a correlation with the dimension of Comfort using the DIDL questionnaire. Therefore, we might conclude that oral hygiene did not influence their daily living. Other studies went even further than ours, and included patients with oral problems such as caries and periodontal disease. Few studies have confirmed a correlation in adults, but some found correlations with gingival problems and OHRQoL in children [26]. This shows the perception and importance of oral health in their life. In these analyses dental caries had a positive correlation with all dimensions except for comfort, which showed a negative one, which agrees with previous reports where caries was correlated with all domains [1,12]. Unfortunately, our analysis did not identify the conditions of the participants, but this might be interesting to address in the future. For instance, the dimension Comfort asks about bleeding and gums and might show a negative correlation, meaning that presence of a periodontal problem decreases the Comfort score.
Most participants in the current study perceived that their oral health had an effect, mostly a good effect, on their QoL. If people generally visit a dentist only if there is a dental condition requiring treatment, so those visiting a dentist would definitely have lower scores then those who do not visit a dentist. Those who do not visit a dentist consider themselves not in need of oral health care and perceive their oral health to be better. Therefore, this study had some limitations that influence the interpretation and generalization of results. The sample was relatively small and was from a single center, and our findings may not be representative of the whole population. Questionnaires as such and PROs obtain certain levels of subjectivity and bias. Questionnaires have limitations as they are self-reported and reflect the perception of participants, not reality. The subjective nature of the use of questionnaires alone and the wide range of ages, including children, are major limitations. DIDL and OHRQoL are reliable questionnaires, but were not developed for children, so our study did not use a questionnaire that was specifically designed for children. Moreover, we did not investigate participants’ reasons for visiting a dentist, as this depends upon a perceived need for treatment and might also impact the QoL and perception of oral health status. Another limitation is that we only included patients with dental conditions and not patients who came for regular dental checkups and prevention, who perceive their oral health differently and this may have affected scores of self-reports and oral health status.
Conclusions
This small study from Kosovo showed reasonable satisfaction with oral health and its association with quality of life. To the best of our knowledge, this report is the first attempt to assess how people perceive their oral health and how these influence their QoL in Kosovo. This study identified that our population is relatively satisfied with their oral health-related QoL. While participants reported good effects of oral health on their QoL, they were least satisfied with Comfort and most satisfied with Performance.
Tables
Table 1. Basic characteristics of enrolled participants.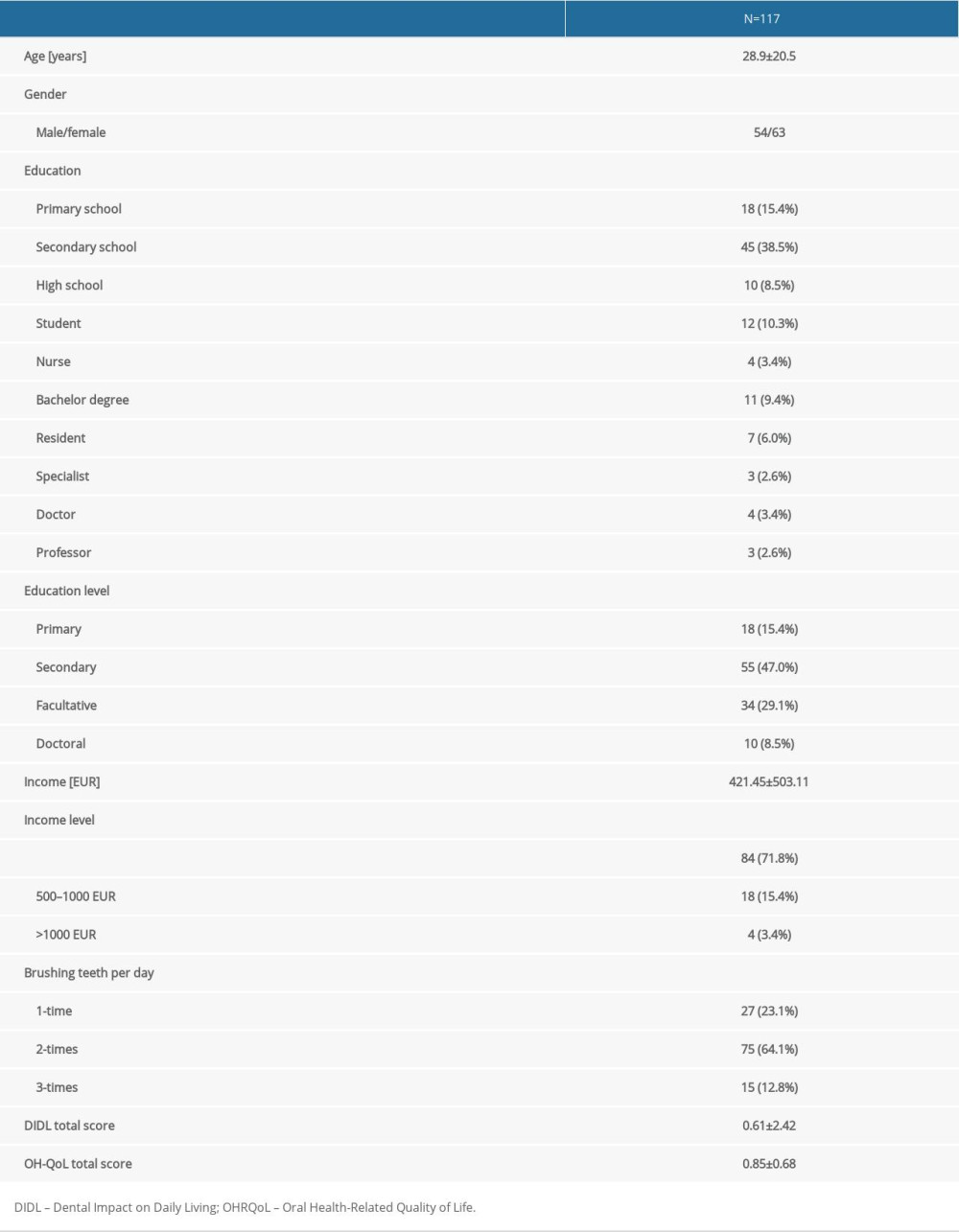 Table 2. Results of DIDL questionnaire for measuring the dental impact on daily living health.
Table 2. Results of DIDL questionnaire for measuring the dental impact on daily living health.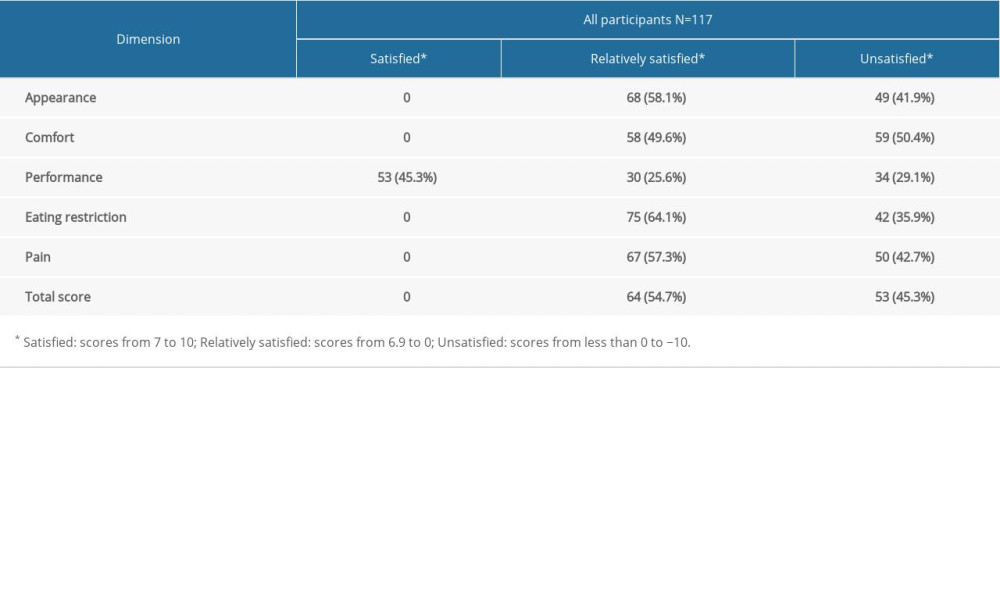 Table 3. Comparison of independent variables and related total score of DIDL and OH-QoL questionnaires.
Table 3. Comparison of independent variables and related total score of DIDL and OH-QoL questionnaires.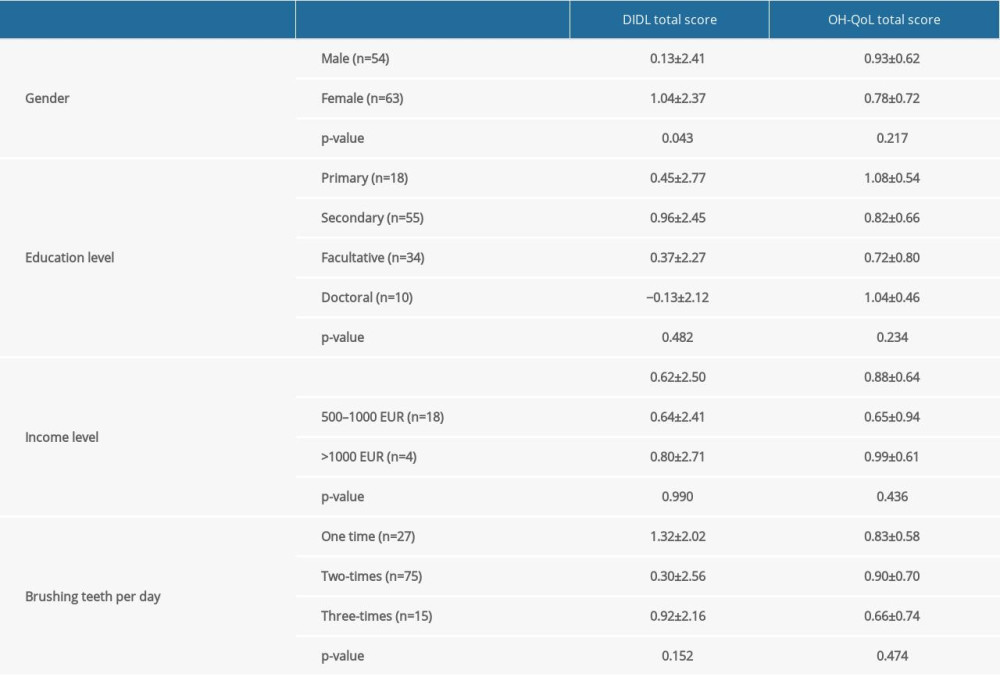 Table 4. Linear regression calculation for prediction of total score of DIDL.
Table 4. Linear regression calculation for prediction of total score of DIDL.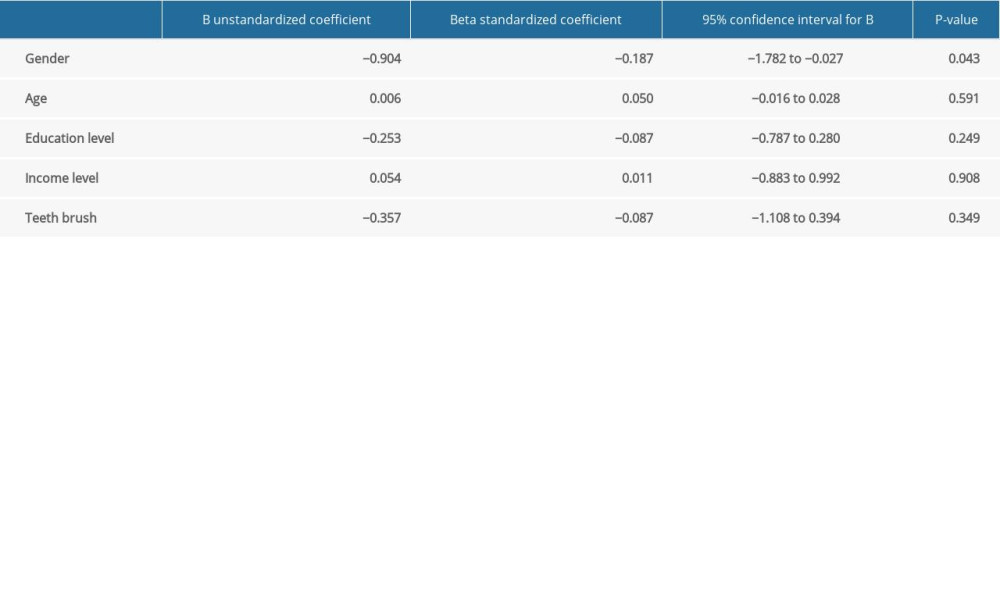 Table 5. Linear regression calculation for prediction of total score of OH-QoL.
Table 5. Linear regression calculation for prediction of total score of OH-QoL.
References
1. Ganesh R, John J, A correlation between dental caries and dental impact on daily living: A cross sectional study: Indian J Oral Sci, 2013; 4; 70
2. Bulgareli JV, de Faria ET, Cortellazzi KL, Factors influencing the impact of oral health on the daily activities of adolescents, adults and older adults: Rev Saude Publica, 2018; 52; 44
3. Deepan Kumar CV, Mohamed S, Janakiram C, Joseph J, Validation of dental impact on daily living questionnaire among tribal population of India: Contemp Clin Dent, 2015; 6(Suppl 1); S235-41
4. Bettie NF, Ramachandiran H, Anand V, Tools for evaluating oral health and quality of life: J Pharm Bioallied Sci, 2015; 7(Suppl 2); S414-19
5. De Ataíde Mariz AL, Araújo SL, Negrinho LA, Impact of dental treatment on self-esteem and oral health selfperception of children and adolescents victims of sexual abuse: Braz Dent Sci, 2018; 21(2); 185
6. Dumitrescu AL, Dogaru BC, Dogaru CD, Self-control and self-confidence:Ttheir relationship to self-rated oral health status and behaviours: Oral Health Prevent Dent, 2009; 7(2); 155-62
7. Koistinen S, Olai L, Ståhlnacke K, Fält A, Ehrenberg A, Oral health-related quality of life and associated factors among older people in short-term care: Int J Dent Hyg, 2020; 18(2); 163-72
8. Sixoub JL, How to make a link between Oral Health-Related Quality of Life and dentin hypersensitivity in the dental office?: Clin Oral Investig, 2013; 7(Suppl 1); S41-44
9. Sheiham A, Alexander D, Cohen L, Global Oral Health Inequalities: Task Group-Implementation and delivery of oral health strategies: Adv Dent Res, 2011; 23(2); 259-67
10. Lee GH, McGrath C, Yiu CK, King NM, A comparison of a generic and oral health-specific measure in assessing the impact of early childhood caries on quality of life: Community Dent Oral Epidemiol, 2010; 38(4); 333-39
11. Leao A, Sheiham A: Dental impact on daily living Measuring Oral Health-Related Quality of Life, 1997, Chapel Hill, University of North Carolina Dental Ecology
12. Leao A, Sheiham A, Relation between clinical dental status and subjective impacts on daily living: J Dent Res, 1995; 74(7); 1408-13
13. Frisch MB, Cornell J, Villanueva M, Retzlaff PJ, Clinical validation of the quality of life inventory: A measure of life satisfaction for use in treatment planning and outcome assessment: Psychological Assessment, 1992; 4(1); 92-101
14. Sischo L, Broder HL, Oral health-related quality of life: What, why, how, and future implications: J Dent Res, 2011; 90(11); 1264-70
15. Reissmann DR, Methodological considerations when measuring oral health-related quality of life: Oral Rehabil, 2021; 48(3); 233-45
16. Okunseri C, Chattopadhyay A, Lugo RI, McGrath C, Pilot survey of oral health-related quality of life: A cross-sectional study of adults in Benin City, Edo State, Nigeria: BMC Oral Health, 2005; 5; 7
17. Malicka B, Skośkiewicz-Malinowska K, Kaczmarek U, The impact of socioeconomic status, general health and oral health on Health-Related Quality of Life, Oral Health-Related Quality of Life and mental health among Polish older adults: BMC Geriatr, 2022; 22; 2
18. Newton JT, Subramanian SS, Westland S, The impact of tooth colour on the perceptions of age and social judgements: J Dent, 2021; 112(2021); 103771
19. Isiekwe GI, Aikins EA, Self-perception of dental appearance and aesthetics in a student population: Inter Orthodon, 2019; 17(2); 506-12
20. Cornell JE, Saunders MJ, Paunovich ED: Oral health quality of life inventory (OH-QoL) Measuring Oral Health-Related Quality of Life, 1997, Chapel Hill, University of North Carolina Dental Ecology
21. Sancho FM, Tsakos G, Brealey D, Development of a tool to assess oral health-related quality of life in patients hospitalised in critical care: Qual Life Res, 2020; 29; 559-68
22. Hajek A, Kretzler B, König HH, Factors Associated with dental service use based on the andersen model: A systematic review: Int J Environ Res Public Health, 2021; 18(5); 2491
23. Ellakany P, Fouda SM, Alghamdi M, Bakhurji E, Factors affecting dental self-confidence and satisfaction with dental appearance among adolescents in Saudi Arabia: A cross sectional study: BMC Oral Health, 2021; 21; 149
24. Su S, Lipsky MS, Licari FW, Hung M, Comparing oral health behaviours of men and women in the United States: J Dent, 2022; 122(2022); 104157
25. Hamasha AAH, Alshehri A, Alshubaiki A, Gender-specific oral health beliefs and behaviors among adult patients attending King Abdulaziz Medical City in Riyadh: Saudi Dent J, 2018; 30(3); 226-31
26. Gherunpong S, Tsakos G, Sheiham A, The prevalence and severity of oral impacts on daily performances in Thai primary school children: Health Qual Life Outcomes, 2004; 2; 57
Tables
 Table 1. Basic characteristics of enrolled participants.
Table 1. Basic characteristics of enrolled participants. Table 2. Results of DIDL questionnaire for measuring the dental impact on daily living health.
Table 2. Results of DIDL questionnaire for measuring the dental impact on daily living health. Table 3. Comparison of independent variables and related total score of DIDL and OH-QoL questionnaires.
Table 3. Comparison of independent variables and related total score of DIDL and OH-QoL questionnaires. Table 4. Linear regression calculation for prediction of total score of DIDL.
Table 4. Linear regression calculation for prediction of total score of DIDL. Table 5. Linear regression calculation for prediction of total score of OH-QoL.
Table 5. Linear regression calculation for prediction of total score of OH-QoL. In Press
12 Mar 2024 : Clinical Research
Metabolomic Alterations in Methotrexate Treatment of Moderate-to-Severe PsoriasisMed Sci Monit In Press; DOI: 10.12659/MSM.943360
14 Mar 2024 : Clinical Research
Renal Dysfunction Increases Risk of Adverse Cardiovascular Events in 5-Year Follow-Up Study of Intermediate...Med Sci Monit In Press; DOI: 10.12659/MSM.943956
15 Mar 2024 : Clinical Research
Impact of One-Lung Ventilation on Oxygenation and Ventilation Time in Thoracoscopic Heart Surgery: A Compar...Med Sci Monit In Press; DOI: 10.12659/MSM.943089
14 Mar 2024 : Clinical Research
Differential DHA and EPA Levels in Women with Preterm and Term Births: A Tertiary Hospital Study in IndonesiaMed Sci Monit In Press; DOI: 10.12659/MSM.943895
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952








