10 March 2023: Clinical Research
Balloon Dilation Eustachian Tuboplasty Combined with Tympanotomy Tube Insertion for Treatment of Refractory Otitis Media with Effusion: A Randomized, Prospective, Controlled Trial Comparing Local Anesthesia Combined Sedation Versus General Anesthesia
Bingyi Dai1ABCDE, Xiao Yin1BF, Danni GuoDOI: 10.12659/MSM.938879
Med Sci Monit 2023; 29:e938879
Abstract
BACKGROUND: Balloon dilation eustachian tuboplasty (BET) is used to treat eustachian dysfunction but its therapeutic effect and cost-effectiveness when combined with tympanotomy tube insertion (TBI) on refractory otitis media with effusion under local anesthesia with sedation compared to traditional general anesthesia are not well understood.
MATERIAL AND METHODS: Forty patients with refractory secretory otitis media who received BET+TBI were enrolled in this study and randomized into the local anesthesia with sedation group (n=20) and general anesthesia group (n=20). Tympanometry (TMM), 7-item eustachian tube dysfunction questionnaire (ETDQ-7) results, intraoperative anesthesia accidents, and operation costs were compared between the groups.
RESULTS: Patients in the local anesthesia with sedation group exhibited intraoperative awareness and pain. Differences in TMM, ETDQ-7 results, and postoperative VAS scores between the groups were comparable (P>0.05). Notably, operative time and treatment costs in the local anesthesia group were lower compared with general anesthesia group.
CONCLUSIONS: The treatment effects and safety of local anesthesia and general anesthesia under BET combined with TBI for treatment of refractory otitis media with effusion are comparable. However, further studies should aim at reducing pain and discomfort.
Keywords: Otitis Media with Effusion, Anesthesia, Local, Eustachian Tube, Humans, Treatment Outcome, Dilatation, Prospective Studies, Anesthesia, General, Ear Diseases, Pain
Background
Refractory otitis media with effusion (ROME) is a common disorder in ENT clinics. It is characterized by aural fullness and hearing loss, and it often leads to tympanic atelectasis and adhesive otitis media. In adults, it has a low prevalence (approximately 0.55–1%) [1]. Most ROME cases in adults are due to eustachian tube dysfunction (ETD) [2]. Traditional treatment options for ROME include medicines such as antibiotics, nasal steroids, and decongestants, physical training such as Valsalva maneuver, or surgical processes such as tympanic paracentesis (TP) or placement of a grommet to treat ETD [3]. However, these therapeutic approaches are not effective.
Balloon eustachian tuboplasty (BET) under general anesthesia is a therapeutic option with promising short-term results for ETD. It is a minimally invasive, simple, and safe approach [4–8]. Good treatment outcomes for ROME using BET and tympanostomy tube insertion (TBI) have been reported. BET+TBI was initially performed under general anesthesia [4]. However, there has been increased interest in performing the procedure in office settings under local anesthesia, and the feasibility of such an approach has been reported in recent years with varying local anesthesia protocols. However, there is a need to improve the technique [9,10]. In some areas, BET and TBI are still mainly performed under general anesthesia. Catalano et al first established the feasibility of BET under local anesthesia in 2012 [11]. Performing BET under local anesthesia with monitored anesthesia care (MAC) instead of general anesthesia confers the advantages of improved patient safety, faster patient recovery, and reduced treatment costs [12].
This study aimed to compare the clinical effects, safety, and cost-effectiveness of BET combined with TBI on ROME under local anesthesia with MAC vs general anesthesia.
Material and Methods
STUDY PARTICIPANTS:
This was a randomized, prospective, controlled trial. In total, 40 adults (age range=18–56 years) – 23 males (28 ears, including 5 binaural cases and 18 monaural cases) and 17 females (20 ears, including 3 binaural cases and 14 monaural cases) – were enrolled from December 2020 to November 2021 at the Affiliated Hospital of Jiangnan University. Patients with ROME diagnosed at least 6 months earlier were randomized based on computer software-assigned numbers allocated into 2 groups: the BET+TBI under local anesthesia group (Study group, 20 patients with 25 ears, including 5 binaural cases) and the BET+TBI under general anesthesia group (Control group, 20 patients with 23 ears, including 3 binaural cases). Eustachian tube dysfunction was diagnosed with tympanometry (TMM), the 7-item eustachian tube dysfunction questionnaire (ETDQ-7), and visual analog scale (VAS) with a 0–10 scale (0, no discomfort; 10, worst possible discomfort) [13]. Differences in gender, age, and disease duration since diagnosis between the groups were insignificant. This study was approved by the Ethics Review Board of the Affiliated Hospital of Jiangnan University (Ethics Approval Number: 2020023). All patients provided a signed informed consent form before enrollment.
INCLUSION AND EXCLUSION CRITERIA:
The inclusion criteria for this study were:
The exclusion criteria were:
OPERATION PROCEDURES:
For surgical procedures under local anesthesia with MAC, all patients were administered 15 mg/kg (1 g maximum) paracetamol according to their body weight before the procedure. The upper-limb venous access was opened and intravenously perfused with dexmetomidine at 1 μg/kg/h during the procedure for sedation. For patients experiencing unbearable pain, 5 ml of Dezocine was intravenously injected. For nasal nerve block, the nasal cavity was filled with cotton sheet supplemented with 3 ml of 0.1% adrenaline and 20 ml 1% tetracaine for about 15 to 20 min. The filling sites were the middle nasal meatus, olfactory sulcus, meatus nasi communis, nasopharynx, inferior nasal meatus, and nasal septum mucosa, among others. For local anesthesia and lubrication, 1 ml of lidocaine-prilocaine cream was applied to the eustachian tube lumen under endoscopy for 5 min. The endoscope was inserted into the ipsilateral nostril with the balloon dilatation catheter. If the nose was too narrow for both the endoscope and balloon dilatation catheter to pass, a 45° angulated endoscope was inserted in the contralateral nostril to visualize the eustachian tube orifice. Surgical techniques for BET+TBI were performed as previously described [14]. A balloon catheter (Carefree, Guangzhou Manxiang Medical Equipment Co., Ltd., China) was inserted into the ET with endoscopic assistance (0- or 30-degree view angle). The balloon was inflated with sterile water with a pressure of 10 bars for 2 min. After termination of inflation, the deflated balloon catheter was removed and the catheter tip was positioned correctly. After the procedures, the pharyngeal ostium of the eustachian tube was observed to be smooth and the openings enlarged without breakage (Figure 3). Then, the patients were instructed to turn the head to one side and, while keeping the affected ear up, perform the Valsalva maneuver. If entire tympanic atelectasis was restored when assessed by optic endoscopy, BET was proven effective and the patient would then undergo the TBI procedure (Figure 4). For general anesthesia, TBI was performed before BET and without the Valsalva maneuver.
QUESTIONNAIRE:
Once patients returned to the ward after the operation, they were asked to complete a questionnaire evaluating their operation experiences. The questionnaires were administered when patients felt comfortable. All patients were followed up at 1, 3, 6, and 12 months after the operation to observe the ventilation and tympanic membrane. ETDQ-7 results and VAS scores were recorded at each follow-up.
STATISTICAL ANALYSIS:
All analyses were performed using SPSS 22.0 software. The
Results
All patients successfully completed the BET+TBI procedure without any intraoperative anesthesia accidents, such as cardiopulmonary receptor reflex or marked fluctuations in blood oxygen levels, heart rate, or blood pressure. No difference in bleeding or abnormal patency of the eustachian tube or any other complications were observed between the groups. BET+TBI under local anesthesia with MAC was associated with higher discomfort compared with the general anesthesia group (mean VAS score=5.2±0.6 vs 0,
Three months after surgery, ETDQ-7 scores and R-values of TMM were significantly improved in both groups compared with preoperative scores (
The average total duration of the operation under local anesthesia was 49±17.26 min, whereas the total duration of anesthesia and operation in the general anesthesia group was 125.7±17.36 min, which significantly shortened the operation time (
Discussion
Since Catalano et al successfully performed BET under local anesthesia in 2012, this procedure has gradually become popular, but general anesthesia is still being used in many places [11]. In this study, we found that BET can be safely performed with MAC at a pressure of 10 to 12 atm and a dilatation time of 2 min. Our results are consistent with those reported by Veera et al, who reported that BET under MAC can be safely and effectively performed [15].
In this study, patients underwent surgery under local anesthesia while still awake, and reported mild nervousness and discomfort. However, since they were awake, they could communicate their discomfort for timely interventions during the operation. In this study, 19 patients in the local anesthesia with MAC group reported that the procedure provided adequate pain relief, whereas 1 patient reported the operation was uncomfortable during a retrospective review of the procedure. Further, all patients in the local anesthesia with MAC group reported complete relief from all discomfort within 1–2 h after the procedure. However, the experience of pain or discomfort during the operation in the local anesthesia group compared with the general anesthesia group suggests the need to improve our anesthetic techniques when performing eustachian tube and lumen procedures. Due to being awake during the operation, pain and discomfort could be generated from mucosal sensory, mechanical, or stretch receptors within the lumen of the cartilaginous eustachian tube (ET) or middle ear. This neuronal reflex arc also has the potential to trigger vasovagal responses [16]. Therefore, to reduce pain, Joonas et al suggested the rate of inflation not exceed 1 atm/s [17].
Compared with the general anesthesia group, postoperative VAS scores were slightly lower in the local anesthesia group. Under local anesthesia with MAC, the intraoperation procedures were tolerable, whereas the postoperative pain gradually increased after the analgesic effects subsided. Therefore, VAS scores after surgery were slightly but not significantly different between the 2 groups (
Regarding the order of BET and TBI during the procedure, some operators believe that TBI should be performed before BET [19]. The reasoning behind this view is that removing the effusion or secretion in the tympanic cavity may balance the pressure between the external and middle ear. The middle ear could be in a negative pressure state caused by ETD, and if BET is performed first, the pressure in the middle ear cavity will change sharply when the balloon catheter is expanded in the eustachian tube lumen. However, whether performing TBI first followed by BET will affect the inner ear is still not clear. In this study, BET was performed first, followed by TBI, in the local anesthesia group. During the dilation process, the patient was clearly conscious and instructed to perform the Valsalva maneuver, which could indicate the patency of the eustachian tube.
Treatment costs are an important consideration in modern health practice. Surgery under local anesthesia with MAC, rather than general anesthesia, usually saves costs [20]. In this feasibility study, local anesthesia was performed in the operation room for monitoring. The anesthesiologist was on stand-by and constantly monitored the patients prepared for sedation. From the beginning of local anesthesia to the end of the operation, the average time consumed was about 49±17.26 min. Patients in the local anesthesia group experienced inapparent adverse reactions; therefore, anesthesia should be done in the preparation room before the patients enter the operating room. This will reduce the anesthesiologist’s time in the operating room by about 20 min, thereby reducing treatment costs [21]. Based on our findings, we believe that patients under the current local anesthetic scheme experienced some pain and discomfort, and some of them required intravenous drugs to relieve pain. Therefore, we do not recommend surgery without an intravenous approach.
The number of patients in this preliminary study was limited. While the local anesthesia group had no significant adverse reactions, we cannot rule out intraoperative pain and possible vagus reactions due to significant changes in heart rate or blood pressure. A patient was reported for the first time to experience bradycardia (heart rate of 30 beats per min) during BET under local anesthesia at the University of Helsinki hospital, which was relieved by intravenous atropine administration [12]. Therefore, we recommend proper intraoperative monitoring and intravenous access for BET under local anesthesia until more patients are safely treated and anesthetic procedures are improved. In addition, the high VAS score in the local anesthesia group indicated that some patients could still sense pain during the operation, suggesting that local anesthesia and operation approaches need further improvements.
Conclusions
BET+TBI under local anesthesia with MAC for treatment of refractory otitis media with effusion is feasible and safe. However, under the current program, patients still feel slight pain and discomfort, indicating the need to improve it. Clinically, BET is a potentially effective therapeutic approach, but further investigations are needed to improve pain control and vagal reactions.
Figures
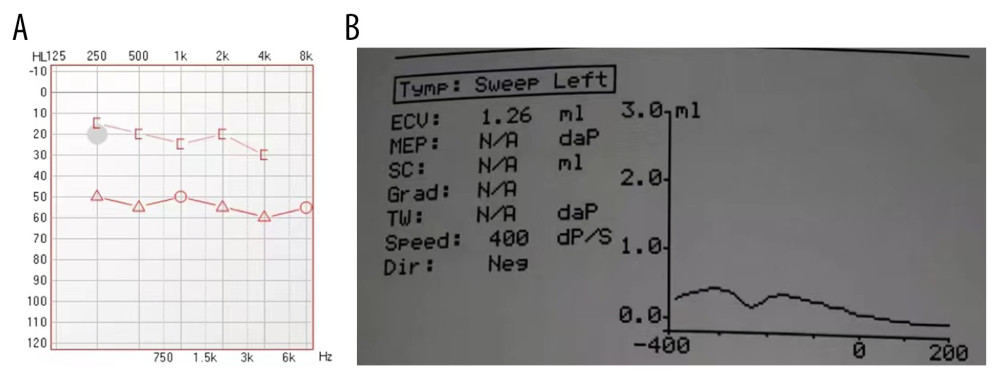 Figure 1. Acoustic impedance measurement. (A) Pure tone audiogram suggests conductive hearing loss, air-bone gap is approximately 30 DB. (B) Acoustic immittance showed a type B tympanogram.
Figure 1. Acoustic impedance measurement. (A) Pure tone audiogram suggests conductive hearing loss, air-bone gap is approximately 30 DB. (B) Acoustic immittance showed a type B tympanogram. 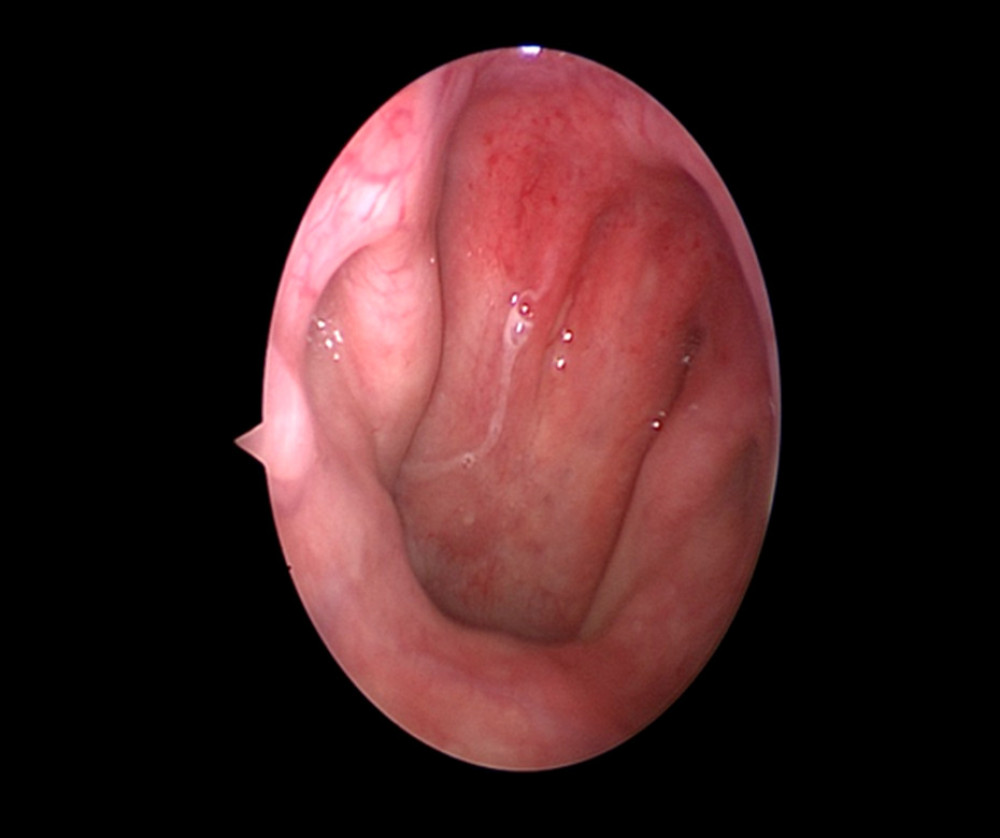 Figure 2. Nasal endoscopy of the right pharyngeal mucosa showing mild edema, and no new organisms in the nasopharynx.
Figure 2. Nasal endoscopy of the right pharyngeal mucosa showing mild edema, and no new organisms in the nasopharynx. 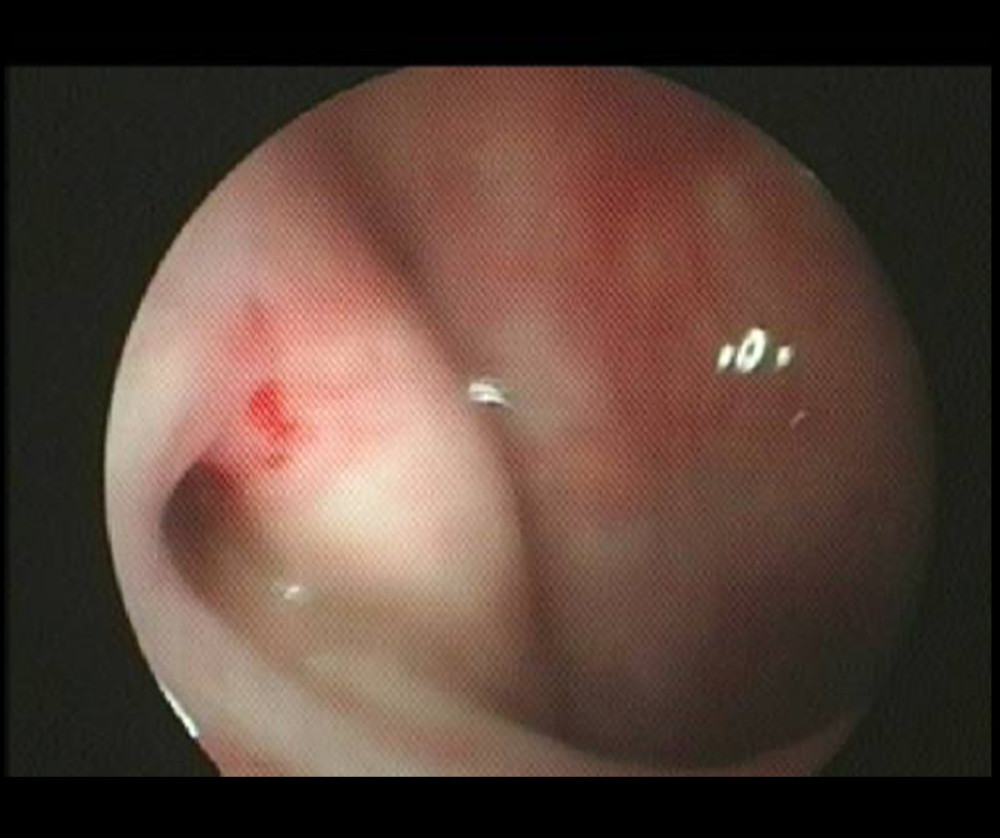 Figure 3. Enlarged pharyngeal ostium of the right eustachian tube and smooth and undamaged mucous membranes after BET.
Figure 3. Enlarged pharyngeal ostium of the right eustachian tube and smooth and undamaged mucous membranes after BET. 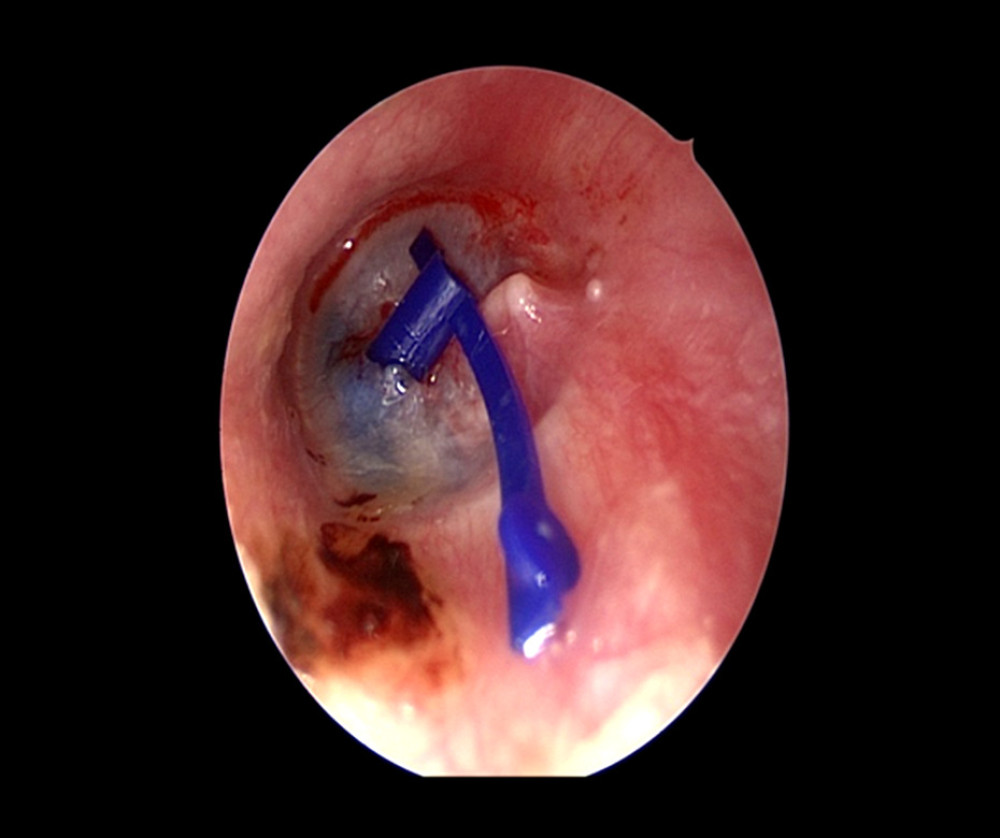 Figure 4. A T tube placed inside the right ear drum.
Figure 4. A T tube placed inside the right ear drum. 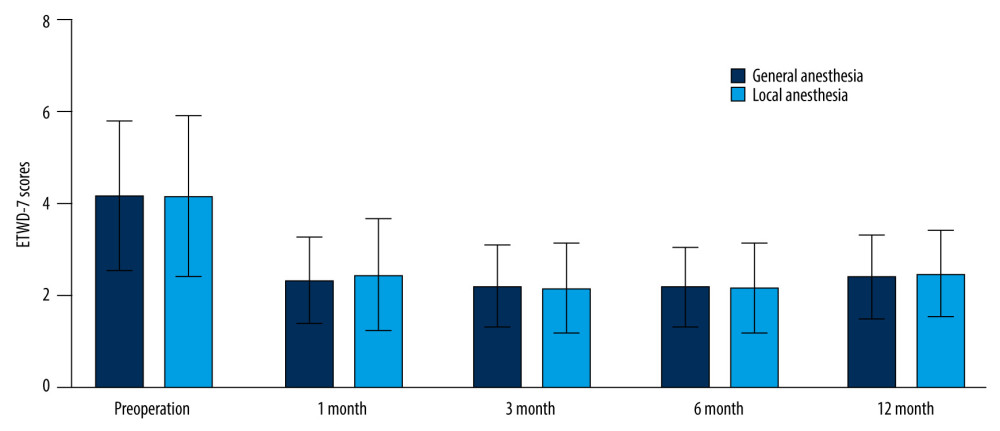 Figure 5. ETDQ-7 score between general anesthesia group and local anesthesia group before and after the operation.
Figure 5. ETDQ-7 score between general anesthesia group and local anesthesia group before and after the operation. 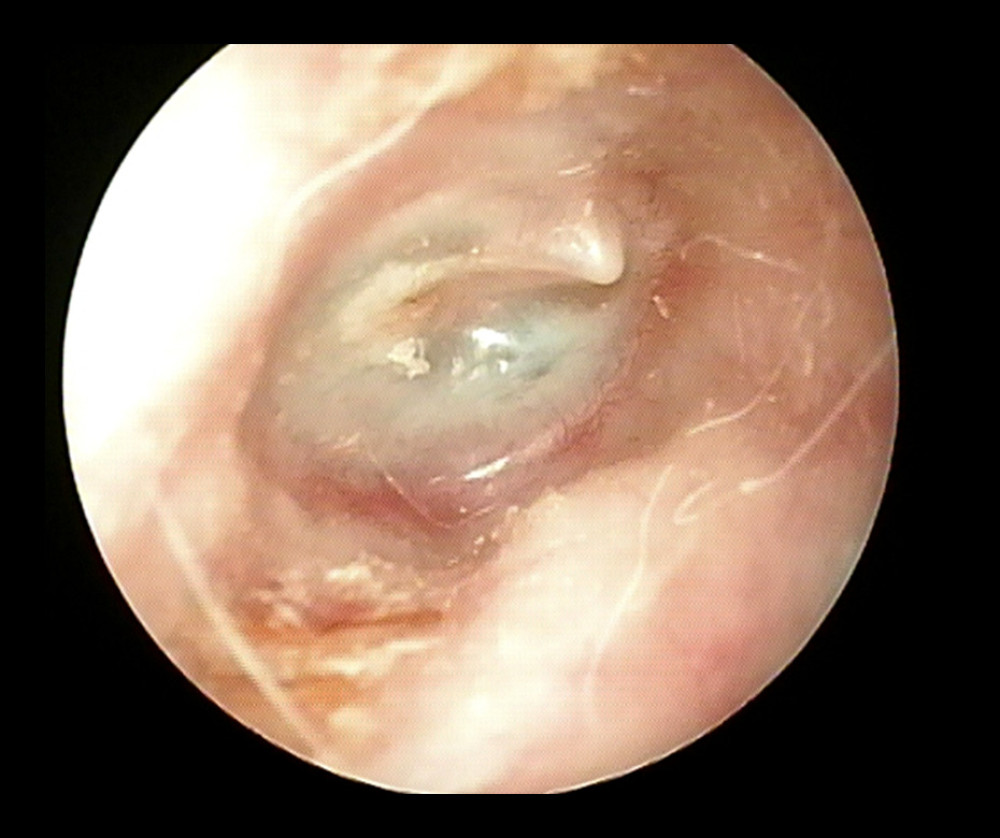 Figure 6. The otoscope was reexamined at 12 months after the operation, and the signs of the right tympanic membrane were intact, without perforation or invagination.
Figure 6. The otoscope was reexamined at 12 months after the operation, and the signs of the right tympanic membrane were intact, without perforation or invagination. References
1. Liang M, Xiong H, Cai Y, Effect of the combination of balloon Eustachian tuboplasty and tympanic paracentesis on intractable chronic otitis media with effusion: Am J Otolaryngol, 2016; 37; 442-46
2. Atkinson H, Wallis S, Coatesworth AP, Otitis media with effusion: Postgrad Med, 2015; 127; 381-85
3. Adil E, Poe D, What is the full range of medical and surgical treatments available for patients with Eustachian tube dysfunction?: Curr Opin Otolaryngol Head Neck Surg, 2014; 22; 8-15
4. Schroder S, Lehmann M, Ebmeyer J, Balloon Eustachian tuboplasty: A retrospective cohort study: Clin Otolaryngol, 2015; 40; 629-38
5. Poe DS, Hanna BM, Balloon dilation of the cartilaginous portion of the eustachian tube: Initial safety and feasibility analysis in a cadaver model: Am J Otolaryngol, 2011; 32; 115-23
6. Randrup TS, Ovesen T, Balloon eustachian tuboplasty: A systematic review: Otolaryngol Head Neck Surg, 2015; 152; 383-92
7. Ockermann T, Reineke U, Upile T, Balloon dilation eustachian tuboplasty: A feasibility study: Otol Neurotol, 2010; 31; 1100-3
8. Silvola J, Kivekas I, Poe DS, Balloon dilation of the cartilaginous portion of the Eustachian tube: Otolaryngol Head Neck Surg, 2014; 151; 125-30
9. Meyer TA, O’Malley EM, Schlosser RJ, A randomized controlled trial of balloon dilation as a treatment for persistent Eustachian tube dysfunction with 1-year follow-up: Otol Neurotol, 2018; 39; 894-902
10. Chen X, Xie L, Zeng H, Local versus general anesthesia for balloon dilation of the Eustachian tube: A single-center retrospective study in a Chinese population: Ear Nose Throat J, 2020 [Online ahead of print]
11. Catalano PJ, Jonnalagadda S, Yu VM, Balloon catheter dilatation of Eustachian tube: A preliminary study: Otol Neurotol, 2012; 33; 1549-52
12. Luukkainen V, Kivekäs I, Hammarén-Malmi S, Balloon Eustachian tuboplasty under local anesthesia: Is it feasible?: Laryngoscope, 2017; 127; 1021-25
13. Van Roeyen S, Van de Heyning P, Van Rompaey V, Responsiveness of the 7-item Eustachian Tube Dysfunction Questionnaire: J Int Adv Otol, 2016; 12; 106-8
14. Yin G, Tan J, Li P, Balloon dilation of Eustachian tube combined with tympanostomy tube insertion and middle ear pressure equalization therapy for recurrent secretory otitis media: J Otol, 2019; 14; 101-5
15. Luukkainen V, Jero J, Sinkkonen ST, Balloon Eustachian tuboplasty under monitored anaesthesia care with different balloon dilation devices: A pilot feasibility study with 18 patients: Clin Otolaryngol, 2019; 44; 87-90
16. Songu M, Aslan A, Unlu HH, Celik O, Neural control of eustachian tube function: Laryngoscope, 2009; 119; 1198-202
17. Toivonen J, Dean M, Kawai K, Poe D, Comparison of outcomes for balloon dilation of the Eustachian tube under local vs general anesthesia: Laryngoscope Investig Otolaryngol, 2022; 7; 1120-28
18. Chan W, Fahlbusch D, Dhillon P, Selva D, Assisted local anesthesia for powered endoscopic dacryocystorhinostomy: Orbit, 2014; 33; 416-20
19. Li L, Mao Y, Hu N, The effect of balloon dilatation eustachian tuboplasty combined with grommet insertion on the structure and function of the Eustachian tube in patients with refractory otitis media with effusion: Ann Palliat Med, 2021; 10; 7662-70
20. Locke MC, Davis JC, Brothers RJ, Love WE, Assessing the outcomes, risks, and costs of local versus general anesthesia: A review with implications for cutaneous surgery: J Am Acad Dermatol, 2018; 78; 983-88e984
21. Childers CP, Maggard-Gibbons M, Understanding costs of care in the Operating Room: JAMA Surg, 2018; 153; e176233
Figures
 Figure 1. Acoustic impedance measurement. (A) Pure tone audiogram suggests conductive hearing loss, air-bone gap is approximately 30 DB. (B) Acoustic immittance showed a type B tympanogram.
Figure 1. Acoustic impedance measurement. (A) Pure tone audiogram suggests conductive hearing loss, air-bone gap is approximately 30 DB. (B) Acoustic immittance showed a type B tympanogram. Figure 2. Nasal endoscopy of the right pharyngeal mucosa showing mild edema, and no new organisms in the nasopharynx.
Figure 2. Nasal endoscopy of the right pharyngeal mucosa showing mild edema, and no new organisms in the nasopharynx. Figure 3. Enlarged pharyngeal ostium of the right eustachian tube and smooth and undamaged mucous membranes after BET.
Figure 3. Enlarged pharyngeal ostium of the right eustachian tube and smooth and undamaged mucous membranes after BET. Figure 4. A T tube placed inside the right ear drum.
Figure 4. A T tube placed inside the right ear drum. Figure 5. ETDQ-7 score between general anesthesia group and local anesthesia group before and after the operation.
Figure 5. ETDQ-7 score between general anesthesia group and local anesthesia group before and after the operation. Figure 6. The otoscope was reexamined at 12 months after the operation, and the signs of the right tympanic membrane were intact, without perforation or invagination.
Figure 6. The otoscope was reexamined at 12 months after the operation, and the signs of the right tympanic membrane were intact, without perforation or invagination. Tables
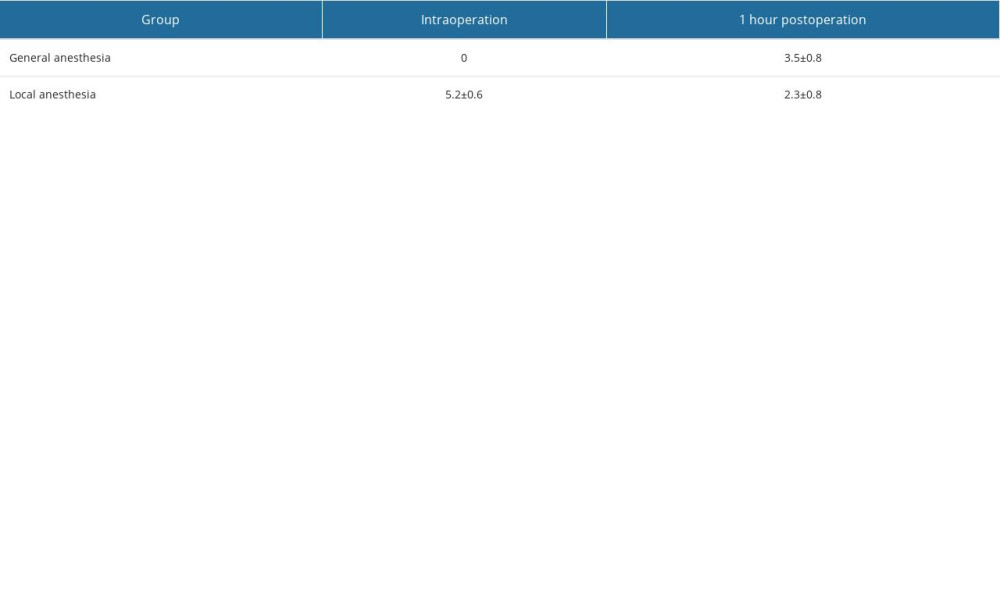 Table 1. Postoperative VAS scores.
Table 1. Postoperative VAS scores.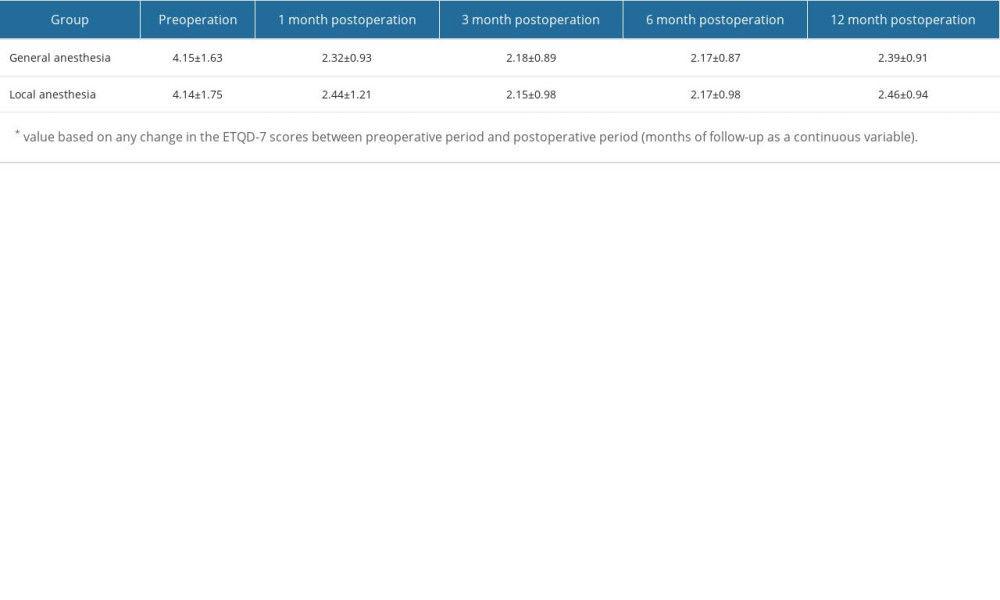 Table 2. Preoperative and postoperative ETQD-7 scores.
Table 2. Preoperative and postoperative ETQD-7 scores.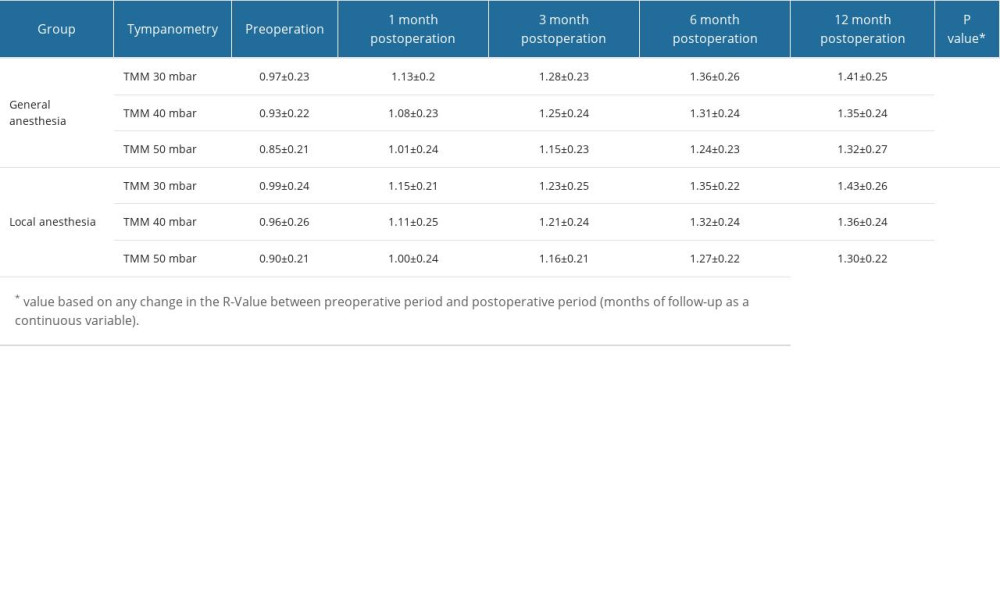 Table 3. R-value score results of tympanometry.
Table 3. R-value score results of tympanometry.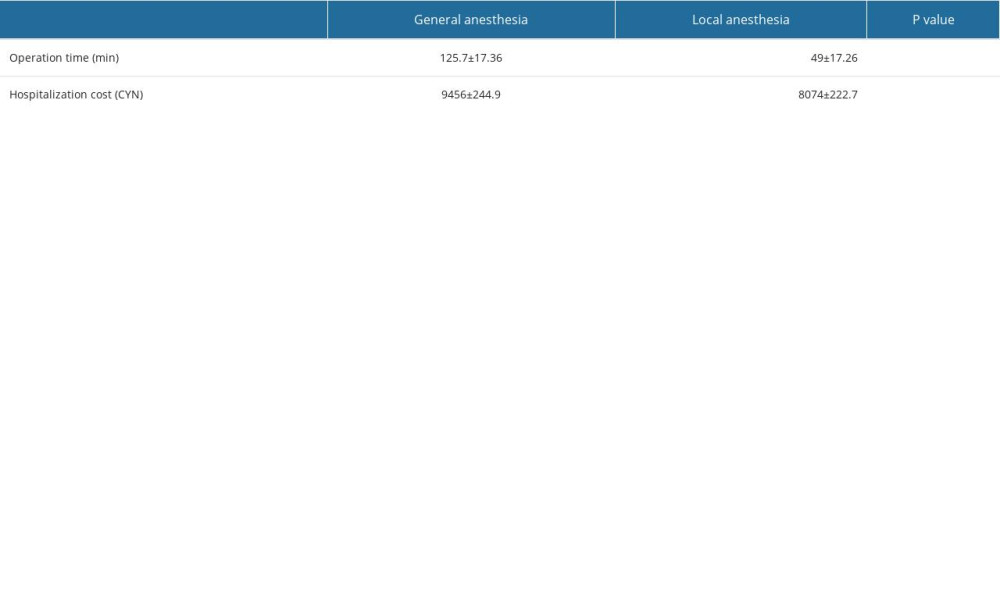 Table 4. Cost-effectiveness of operation under general anesthesia and local anesthesia.
Table 4. Cost-effectiveness of operation under general anesthesia and local anesthesia. Table 1. Postoperative VAS scores.
Table 1. Postoperative VAS scores. Table 2. Preoperative and postoperative ETQD-7 scores.
Table 2. Preoperative and postoperative ETQD-7 scores. Table 3. R-value score results of tympanometry.
Table 3. R-value score results of tympanometry. Table 4. Cost-effectiveness of operation under general anesthesia and local anesthesia.
Table 4. Cost-effectiveness of operation under general anesthesia and local anesthesia. In Press
07 Mar 2024 : Clinical Research
Knowledge of and Attitudes Toward Clinical Trials: A Questionnaire-Based Study of 179 Male Third- and Fourt...Med Sci Monit In Press; DOI: 10.12659/MSM.943468
08 Mar 2024 : Animal Research
Modification of Experimental Model of Necrotizing Enterocolitis (NEC) in Rat Pups by Single Exposure to Hyp...Med Sci Monit In Press; DOI: 10.12659/MSM.943443
18 Apr 2024 : Clinical Research
Comparative Analysis of Open and Closed Sphincterotomy for the Treatment of Chronic Anal Fissure: Safety an...Med Sci Monit In Press; DOI: 10.12659/MSM.944127
08 Mar 2024 : Laboratory Research
Evaluation of Retentive Strength of 50 Endodontically-Treated Single-Rooted Mandibular Second Premolars Res...Med Sci Monit In Press; DOI: 10.12659/MSM.944110
Most Viewed Current Articles
17 Jan 2024 : Review article
Vaccination Guidelines for Pregnant Women: Addressing COVID-19 and the Omicron VariantDOI :10.12659/MSM.942799
Med Sci Monit 2024; 30:e942799
14 Dec 2022 : Clinical Research
Prevalence and Variability of Allergen-Specific Immunoglobulin E in Patients with Elevated Tryptase LevelsDOI :10.12659/MSM.937990
Med Sci Monit 2022; 28:e937990
16 May 2023 : Clinical Research
Electrophysiological Testing for an Auditory Processing Disorder and Reading Performance in 54 School Stude...DOI :10.12659/MSM.940387
Med Sci Monit 2023; 29:e940387
01 Jan 2022 : Editorial
Editorial: Current Status of Oral Antiviral Drug Treatments for SARS-CoV-2 Infection in Non-Hospitalized Pa...DOI :10.12659/MSM.935952
Med Sci Monit 2022; 28:e935952








